CAM
Much has been written on this blog about Dr Michael Dixon, and about the "College of Medicine", which is the direct inheritor of the mantle of the late, unlamented, Prince’s Foundation for Integrated Health. At the time of the foundation of the College it was stated that "The College represents a new strategy to take forward the vision of HRH Prince Charles".
Michael Dixon has also been chairman of the NHS Alliance since 1998. That was one of very few organisations to support Andrew Lansley’s Health Bill. No doubt he will be happy for Crapita Capita to supply alternative nonsense at public expense.
Dr Dixon took offence to a review in The Times of Mark Henderson’s new book, The Geek Manifesto.
 .
.
The review, by David Aaronovitch, said, apropos of the 1023 campaign,
" . . .there was now, almost for the first time, a group of people who were not content to see claims made for discredited treatments without making everyone aware of the science that disproved those claims. And second, what they were doing had implications for public policy."
and
"The geeks represent, for me, one of the most encouraging recent developments in British public life."
This excellent review evidently upset Dr Dixon, because on 20th May, his letter appeared in the Times.
|
David Aaronovitch is right to argue for a robust scientific approach in medicine. However, he is not being logical or scientific when he says that if something is suspected to be placebo then it has no benefit and the NHS should not pay for it. What about scientific research on remedies that many believe to be placebo? These frequently show that there is a benefit but this is confined to those who believe in the treatment given. Surely, in such cases, it would be logical to say that the treatment was beneficial albeit in a specific group of “believers”. From there, it would be good science to compare the safety costs of this supposed placebo remedy with its currently given alternative before deciding whether “believers” should be able to receive such a remedy on the NHS. The problem here is that belief and mindset play an enormous part in healing – science needs to take account of this. Patients’ symptoms are frequently metaphors and effective treatment can often be symbolic and culturally dependent. The mind, in the right circumstances, can produce its own healing chemicals often mimicking those given in conventional medicine. Until science can explain healing in psychosocial as well as biomedical language, we must be cautious about “voting for the geeks” as Mr Aaronovitch suggests. It is far better surely that individual treatment should be tailored, within reason, to the patient and their beliefs and perspectives. Further more, might it not be wiser to direct NHS resources according to pragmatic trials of cost effectiveness and safety rather than a limited interpretation of science that excludes the effect of the mind? Dr Michael Dixon Chair of Council College of Medicine. |
This letter seemed remarkable to me. It is very close to being an admission that alternative medicine is largely placebo. It called for a reply.
We have been here before. Many people have discussed the dubious ethics of deceiving patients by giving placebos while pretending they are no such thing. There is wide agreement that it is not only unethical, but also unnecessary. Kevin Smith has written a scholarly essay on the topic. Edzard Ernst wrote Mind over matter? Margaret McCartney, the Glasgow GP, and author of The Patient Paradox, has explained it. Some views of Dr Dixon’s approach are less flattering than mine. For example, from the USA, Steven Novella’s Dr. Michael Dixon – “A Pyromaniac In a Field of (Integrative) Straw Men”. And, from Majikthyse, Michael Dixon caught red-handed!, and Dr Aust’s Dr Michael Dixon is annoyed. The list is almost endless.
.Two replies were published in the Times on 26 May (and they were the lead letters -bold print). One from the excellent Evan Harris, and one from me.
![]()
Here they are as text.
|
Sir, Dr Michael Dixon’s letter (May 21) is fascinating. He is, of course, a well-known advocate of alternative medicine. Yet he seems now to believe that much alternative medicine is just a placebo. That’s something the geeks have been saying for years, and he appears, at last, to have accepted it. That being the case, it follows that we have to ask whether placebos produce useful benefits, and whether it is ethical to prescribe them. Nobody denies the existence of placebo effects. But recent research has shown that they are usually both small and transient. Often they are not big enough to provide a useful degree of relief. For example, a recent paper on acupuncture in the British Journal of General Practice showed that it had a remarkably small placebo effect. And placebos have no effect at all on the course of cancer or infectious diseases. There has been an admirable movement in medicine for doctors to be open and honest with patients. Prescribing of medicines that contain no active ingredient involves lying to patients. That is old-fashioned and unethical. It is fair to ask why so many people seem to believe in alternative medicine, if even their placebo effects are small. The answer seems to lie in the “get better anyway” effect (known to geeks as regression to the mean). Most of the conditions for which placebos seem to work are things that wax and wane naturally. You take the “cure” when you are at your worst, and next day you are better. You would have been better anyway, but it’s hard to avoid attributing the improvement to whatever you took. That is why alternative medicine is advertised largely on the basis of anecdotal testimonials. And it is doubtless why Dr Dixon advocates “pragmatic” trials: that’s a euphemism for trials without a proper control group. Psychosocial problems may indeed be very important for some patients. But deceiving such patients with dummy pills is not the proper way to deal with their problems. D. Colquhoun, FRS Professor of Pharmacology, University College London Sir, Dr Michael Dixon argues that the NHS should fund placebo treatments such as homeopathy (though he stops short of agreeing that homeopathy is a placebo) on the basis that they can offer limited help to those who “believe” in them. It is no part of modern ethical medical practice to deceive patients into thinking — or failing to disabuse them of the belief — that an inert substance or ineffective medicine has beneficial effects. This can not be justified by the hope — or even expectation — of deriving for that patient the limited psychologically based improvement in symptoms that may follow from the deployment of the placebo. Pedlars of homeopathy for profit in the private sector will, alas, always seek to fool people into believing the hocus pocus of “memory of water” and the effects of infinite dilution and a lot of bottle-shaking. But doctors have responsibilities not to deceive their patients, even out of a paternalistic wish to assist them to manage their symptoms; and public policy demands that the NHS spends its resources only on treatments that work without deception in a cost-effective way. Dr Evan Harris Oxford |
Follow-up
The College of Medicine is well known to be the reincarnation of the late unlamented Prince of Wales Foundation for Integrated Health. I labelled it as a Fraud and Delusion, but that was perhaps over-generous. It seems to be morphing into a major operator in the destruction of the National Health Service through its close associations with the private health industry.
Their 2012 Conference was held on 3rd May. It has a mixture of speakers, some quite sound, some outright quacks. It’s a typical bait and switch event. You can judge its quality by the fact that the picture at the top of the page that advertises the conference shows Christine Glover, a homeopathic pharmacist who makes a living by selling sugar pills to sick people (and a Trustee of the College of Medicine).
Her own company’s web site says
The approaches are, of course, based on sugar pills. The claim is untrue and dangerous. My name for that is fraud. |
 |
When the "College of Medicine" started it was a company, but on January 30th 2012, it was converted to being a charity. But the Trustees of the charity are the same people as the directors of the company. They are all advocates of ineffective quack medicine. The contact is named as Linda Leung, who was Operations Director of the Prince’s Foundation until it closed, and then became Company Secretary for the “College of Medicine”.
The trustees of the charity are the same people who were directors of the company
- Dr Michael Dixon, general practitioner. Michael Dixon was Medical Director of the Prince’s Foundation until it closed down.
- Professor George Lewith, is Professor of Health Research in the Complementary Medicine Research Unit, University of Southampton. He was a Foundation Fellow of the Prince’s Foundation until it closed down. Much has been written about him here.
- Professor David Peters. is Professor of Integrated Healthcare and Clinical Director at the University of Westminster’s School of Integrated Health; He’s famous for allowing dowsing with a pendulum as a method of diagnosis for treatment with unproven herbal medicines,
He was a Foundation Fellow of the Prince’s Foundation until it closed down. - Mrs Christine Glover is a pharmacist who sells homeopathic pills. She was a Foundation Fellow of the Prince’s Foundation until it closed down.
The involvement of Capita
According to their web site
"A Founder of the College of Medicine is Capita."
Still more amazingly, the CEO of the College of Medicine is actually an employee of Capita too.
"Mark Ratnarajah is interim CEO of the College of Medicine as well as Business Director at Capita Health and Wellbeing."

|
That isn’t the end of it. The vice-president of the College of Medicine is Dr Harry Brunjes. There is an article about him in the May 2012 issue of Director Magazine. It has to be said that he doesn’t sound like a man with much interest in the National Health Service.. |
Within 9 years of graduating he set up in private practice in Harley Street. Five years later he set up Premier Medical, which, after swallowing a couple of rivals, he sold to Capita for £60 million. He is now recorded in a Companies House document as Dr Henry Otto Brunjes, a director of Capita Health Holdings Limited. This company owns all the shares in Capita Health and Wellbeing Limited, and it is, in turn, owned by Capita Business Services Limited. And they are owned by Capita Holdings Limited. I do hope that this baroquely complicated array of companies with no employees has nothing to do with tax avoidance.
Capita is, of course, a company with a huge interest in the privatisation of health care. It also has a pretty appalling record for ripping off the taxpayer.
It has long been known in Private Eye, as “Crapita” and “the world’s worst outsourcing firm”.
Capita were responsible for of the multimillion pound failed/delayed IT project for the NHS and HMRC. They messed up on staff administration services at Leicester Hospitals NHS Trust and the BBC where staff details were lost. They failed to provide sufficient computing systems for the Criminal Records Bureau, which caused lengthy delays. Capita were also involved in the failure of the Individual Learning Accounts following a £60M over-spend. And most recently, they have caused the near collapse of court translation services after their acquisition of Applied Language Services.
With allies like that, perhaps the College of Medicine hardly needs enemies. No doubt Capita will be happy to provide the public with quackery for an enormous fee from the taxpayer.
 |
One shouldn’t be surprised that the College is involved in Andrew Lansley’s attempts to privatise healthcare. Michael Dixon, Chair of the College of Medicine, also runs the "NHS Alliance", almost the only organisation that supported the NHS Bill. The quackery at his own practice defies belief (some it is described here). |
One would have thought that such a close association with a company with huge vested interests would not be compatible with charitable status. I’ve asked the Charity Commission about that. The Charity commission, sadly, makes no judgements about the worthiness of the objects of the charities it endorses. All sorts of dangerous quack organisations are registered charities, like, for example, Yes to Life.
Secrecy at the College of Medicine
One of the big problems about the privatisation of medicine and education is that you can’t use the Freedom of Information Act to discover what they are up to. A few private companies try to abide by that act, despite not being obliged to do so. But the College of Medicine is not one of them.
Capita They refuse to disclose anything about their relationship with Capita. I asked I asked Graeme Catto, who is a friend (despite the fact that I think he’s wrong). I got nothing.
"Critical appraisal" I also asked Catto for the teaching materials used on a course that they ran about "critical appraisal". Any university is obliged, by the decision of the Information Tribunal, to produce such material on request. The College of Medicine refused, point blank. What, one wonders, have they got to hide? Their refusal strikes me as deeply unethical.
The course (costing £100) on Critical Appraisal, ran on February 2nd 2012. The aims are "To develop introductory skills in the critical appraisal of randomised controlled trials (RCTs) and systematic reviews (SRs)". That sounds good. Have they had a change of heart about testing treatments?
But, as always, you have to look at who is running the course. Is it perhaps a statistician with expertise in clinical trials? Or is it a clinician with experience in running trials? There are plenty of people with this sort of expertise. But no, It is being run by a pharmacist, Karen Pilkington, from that hotbed of unscientific medicine, the University of Westminster.
Pilkington originally joined the University of Westminster as manager for a 4-year project to review the evidence on complementary therapies (funded by the Department of Health). All of her current activities centre round alternative medicine and most of her publications are in journals that are dedicated to alternative medicine. She teaches "Critical Appraisal" at Westminster too, so I should soon have the teaching materials, despite the College’s attempts to conceal them.
Three people who ought to know better
Ore has to admire, however grudgingly, the way that the quacks who run the College of Medicine have managed to enlist the support of several people who really should know better. I suppose they have been duped by that most irritating characteristic of quacks, the tendency to pretend they have the monopoly on empathetic treatment of patients. We all agree that empathy is good, but every good doctor has it. One problem seems to be that senior medical people are not very good at using Google. They don’t do their homework.

|
Professor Sir Graeme Catto MD DSc FRCP FMedSci FRSE is president of the College of Medicine. He’s Emeritus Professor of Medicine at the University of Aberdeen. He was President of the General Medical Council from 2002 to 2009, Pro Vice-Chancellor, University of London and Dean of Guy’s, King’s and St Thomas’ medical school between 2000 and 2005. He’s nice and well-meaning chap, but he doesn’t seem to know much about what’s going on in the College. |

|
Professor Sir Ian Kennedy LLD, FBA, FKC, FUCL, Hon.DSc(Glasgow), Hon.FRCP is vice-president of the College. Among many other things he is Emeritus Professor of Health Law, Ethics and Policy at University College London. He was Chair of the Healthcare Commission until 2003, when it merged with other regulators to form the Care Quality Commission. No doubt he can’t be blamed for the recent parlous performence of the CQC. |

|
Professor Aidan Halligan MA, MD, FRCOG, FFPHM, MRCPI Since March 200y he has been Director of Education at University College London Hospitals. From 2003 until 2005, he was Deputy Chief Medical Officer for England, with responsibility for issues of clinical governance, patient safety and quality of care. He’s undoubtedly a well-meaning man, but so focussed on his (excellent) homelessness project that he seems immune to the company he keeps. Perhaps the clue lies in the fact that when I asked him what he thought of Lansely’s health bill, he seemed to quite like it. |
It seems to me to be incomprehensible that these three people should be willing to sign a letter in the British Medical Journal in defence of the College, with co-signatories George Lewith (about whom much has been written here) and the homeopath Christine Glover. In so doing, they betray medicine, they betray reason, and most important of all, they betray patients. Perhaps they have spent too much time sitting on very important committees and not enough time with patients.
The stated aims of the College sound good.
"A force that combines scientific knowledge, clinical expertise and the patient’s own perspective. A force that will re-define what good medicine means − renewing the traditional values of service, commitment and compassion and creating a more holistic, patient-centred, preventative approach to healthcare."
But what they propose to do about it is, with a few exceptions, bad. They try to whip up panic by exaggerating the crisis in the NHS. There are problems of course, but they result largely from under-funding (we still spend less on healthcare than most developed countries), and from the progressive involvement of for-profit commercial companies, like Capita. The College has the wrong diagnosis and the wrong solution. How do they propose to take care of an aging population? Self-care and herbal medicines seem to be their solution.
|
The programme for the College’s workshop shows it was run by herbalist Simon Mills and by Dick Middleton an employee of the giant herbal company, Schwabe. You can see Middleton attempting to defend misleading labelling of herbal products on YouTube, opposed by me. |
|
It seems that the College of Medicine are aiding and abetting the destruction of the National Health Service. That makes me angry.(here’s why)
I can end only with the most poignant tweet in the run up to the passing of the Health and Social Care Act. It was from someone known as @HeardInLondon, on March 15th
"For a brief period during 20th century, people gave a fuck & looked after each other. Unfortunately this proved unprofitable." #SaveOurNHS
— HeardinLondon (@HeardinLondon) March 13, 2012
"For a brief period during 20th century, people gave a fuck and looked after each other. Unfortunately this proved unprofitable."
Unprofitable for Crapita, that is.
Follow-up
5 May 2012. Well well, if there were any doubt about the endarkenment values of the College, I see that the Prince of Wales, the Quacktitioner Royal himself, gave a speech at the College’s conference.
"”I have been saying for what seems a very long time that until we develop truly integrated systems – not simply treating the symptoms of disease, but actively creating health, putting the patient at the heart of the process by incorporating our core human elements of mind, body and spirit – we shall always struggle, in my view, with an over-emphasis on mechanistic, technological approaches.”
Of course we all want empathy. The speech, as usual, contributes precisely nothing.
12 June 2012. Oh my, how did I manage to miss the fact the the College’s president, Professor Sir Graeme Catto, is also a Crapita eployee. It’s over a year since he was apponted to Capita’s clinical governance board he says "  In a rapidly growing health and wellbeing marketplace, delivering best practice in clinical governance is of utmost importance. I look forward to working with the team at Capita to assist them with continuing to adopt a best in class approach.". The operative word is "marketplace".
In a rapidly growing health and wellbeing marketplace, delivering best practice in clinical governance is of utmost importance. I look forward to working with the team at Capita to assist them with continuing to adopt a best in class approach.". The operative word is "marketplace".
Since writing about anti-scientific degrees in Nature (March 2007), much has been revealed about the nonsense that is taught on these degrees. New Year’s day seems like a good time to assess how far we’ve got, five years on.
At the beginning of 2007 UCAS (the universities central admission service) offered 45 different BSc degrees in quackery, at 16 universities.
Now there are only 24 such degrees.
If you exclude chiropractic and osteopathy, which all run at private colleges, with some sort of "validation" from a university, there are now only 18 BSc/MSc courses being offered in eight universities.
Degrees in homeopathy, naturopathy and "nutritional therapy", reflexology and aromatherapy have vanished altogether from UCAS.
In the race to provide BScs in anti-science, Middlesex University has now overhauled the long-standing leader, Westminster, by a short head.
 Michael Driscoll, vice-chancellor of Middlesex |
|
Let’s see what’s gone.
The University of Central Lancashire (UCLAN) was the first to see sense. In August 2008 they announced closure of their “BSc” degree in homeopathy. On September 2008 they announced an internal review of their courses in homeopathy. herbalism and acupuncture. The report of this review closed down all of them in July 2009. I first asked for their teaching materials in July 2006. I finally got them in December 2010, after winning an appeal to the Information Commissioner, and then winning an appeal against that decision at an Information tribunal . By the time I got them, the course had been closed for over two years. That is just as well, because it turned out that UCLAN’s students were being taught dangerous nonsense. No wonder they tried so hard to conceal it.
Salford University was the next to go. They shut down their courses in complementary medicine, homeopathy and acupuncture. In January 2009 they announced " they are no longer considered “a sound academic fit” ". Shortly afterwards. a letter appeared in The Times from three heavyweights (plus me) congratulating the vice-chancellor on his decision.
University of Westminster
For many years, Westminster was the biggest supplier of BSc degrees in quackery. At the beginning of 2007 they offered 14 different BSc degrees in homeopathy, naturopathy, nutritional therapy, "complementary therapies", (western) herbal medicine and traditional Chinese medicine with acupuncture. Some of their courses were so bizarre that some of the students and even staff sent me slides which taught things like "amethysts emit high Yin energy". Like UCLAN, Westminster also held an internal review. Unlike UCLAN it came to the absurd conclusion that all would be well if they injected more science into the courses. The incompetence of the review meant that those who wrote it hadn’t noticed that if you try to put science into homeopathy or naturopathy, the whole subject vanishes in a puff of smoke. Nevertheless Westminster closed down entry to BSc homeopathy in March 2009 (though the subject remained as part of other courses).
Three years after the Nature article, all five BSc homeopathy degrees had shut their doors.
During 2011, Westminster shut down Naturopathy, Nutritional therapy, Therapeutic bodywork and Complementary Medicine. See, for example,
More dangerous nonsense from the University of Westminster: when will Professor Geoffrey Petts do something about it?
Now Westminster has only four courses in two subjects. They still teach some dangerous and untrue things, but I suspect the writing is on the wall for these too.
I have seen a document, dated 11 April 2011, which states
“The following courses have been identified as ‘at risk’ (School definition) and will be discussed at the APRG and University Review Group2, due to poor recruitment and high cost of delivery:
Integrated Health Scheme: BSc Complementary Medicine, Naturopathy; BSc Chinese Medicine; BSc Nutritional Therapy; BSc Herbal Medicine”
All but Chinese medicine and Herbal medicine have already gone. Almost there.
University of Wales
Since my first post in 2008 about the validation scam operated by the University of Wales, and some good investigations by BBC Wales TV, the outcome was the most spectacular so far. The entire institution collapsed. They no longer "validate" external degrees at dodgy business colleges, loony religious colleges or magic medicine colleges.
Another worthless validation: the University of Wales and nutritional therapy (October 2008) This is a ‘degree’ in nutrtional therapy. It is even more hilarious than usual, but it passed the validation anyway.
Scandal of the University of Wales and the Quality Assurance Agency (November 2010). This post followed the BBC Wales TV programme. At last the QAA began to notice, yet further confirmation of its utter ineptitude.
The University of Wales disgraced (but its vice chancellor is promoted) (October, 2011) The eventual collapse of the university was well-deserved. But it is very weird that the people who were responsible for it have still got their jobs. In fact the vice-chancellor, Marc Clement, was promoted despite his mendacious claim to be unaware of what was going on.
It remains to be seen how many of the many quack courses that were validated by the University of Wales will be taken on by other universities. The McTimoney College of Chiropractic is owned by BPP University (so much for their quality control, as explained in Private Eye). but still claims to be validated by Wales until 2017.
Some of the more minor players
Edinburgh Napier University. After an FOI request (rejected), Napier closed their herbal medicine degree in 2010.
Hot and cold herbal nonsense from Napier University Edinburgh: another course shuts. (June 2010)
As expected, the Scottish Information Commissioner agreed with that for England and Wales and ordered material to be sent. Edinburgh Napier University teaches reflexology, aromatherapy and therapeutic touch. Scottish Information Commissioner says you should know. Some of the horrors so discovered appeared in Yet more dangerous nonsense inflicted on students by Edinburgh Napier University. The embarrassment seems to have worked. Their remaining degrees in aromatherapy and reflexology have now vanished from UCAS too. All that remains is a couple of part time “Certificates of Credit” for aromatherapy and reflexology
Anglia Ruskin Univerity Not only have BSc degrees gone in aromatherapy and reflexology, but their midwifery degree now states "We are unable to accept qualifications in aromatherapy, massage and reflexology."
University of Derby Reflexology and aromatherapy have gone, though doubtless Spa management therapies have much nonsense left
University of Greenwich. BSc in Complementary Therapies (Nutritional Health) and BSc in Complementary Therapies (Nutritional Health) have been shut. The BSc Acupuncture is listed on their web site but it is under review, and is not listed in UCAS for 2012. (Acupuncture is run at International College of Oriental medicine, validated by Greenwich.). Only osteopathy (MOst) is still running, and that is a validation of an external course run at The European School of Osteopathy, in Maidstone
Thames Valley University was renamed the University of West London in 2010. The nonsense that was run there (e.g. Nutritional Fairy Tales from Thames Valley University) seems to have vanished. Their previous alt med guru, Nicola Robinson, appears now to be at London South Bank University (ranked 116 out of the 116 UK universities)
What’s left?
Chiropractic Surprisingly, given the total discreditation of chiropractic in the wake of the Simon Singh affair, and the internecine warfare that followed it, none of the chiropractic courses have shut yet. Some are clearly in trouble, so watch this space.
Osteopathy has also had no course closures since 2007. Like chiropractic it also suffers from internecine warfare. The General Osteopathic Council refuses to disown the utter nonsense of "craniosacral" osteopathy. But the more sensible practitioners do so and are roughly as effective as physiotherapists (though there are real doubts about how effective that is).
Excluding chiropractic and osteopathy, this is all that’s left. It now consists almost entirely of Chinese medicine and a bit of herbal.
Glyndwr university (Known as North East Wales Institute until 2008) Ranked 104 out of 116 UK universities
BSc Acupuncture (B341) BSc
BSc Complementary Therapies for Healthcare (B343)
Cardiff Metropolitan University (UWIC) (Known as University of Wales Institute Cardiff (UWIC) until Nov 2011.) The vice-chancellor of Cardiff Metropolitan, Antony Chapman, is in the QAA’s board of directors, so perhaps it isn’t surprising that the QAA has done nothing.
BSc Complementary Therapies (3 years) (B390)
BSc Complementary Therapies (4 yrs inc Foundation) (B300)
University of Lincoln
Acupuncture (B343) 3FT Hon BSc
Herbal Medicine (B342) 3FT Hon BSc
University of East London Ranked 113 out of 116 UK universities
Acupuncture (B343) 3FT Hon BSc
London South Bank University Ranked 116 out of 116 UK universities
Acupuncture (B343) 4FT Deg MCM
The Manchester Metropolitan University Ranked 93 out of 116 UK universities
Acupuncture (B343) 3FT Hon BSc
Middlesex University
Acupuncture (B348) 3FT Hon BSc
Ayurvedic Medicine (A900) 4FT Oth MCM
Herbal Medicine (B347) 3FT Hon BSc
Traditional Chinese Medicine (BT31) 4FT Hon BSc
University of Westminster
Chinese Medicine: Acupuncture (B343) 3FT Hon BSc
Chinese Medicine: Acupuncture with Foundation (B341) 4FT/5FT Hon BSc/MSci
Herbal Medicine (B342) 3FT Hon BSc
Herbal Medicine with Foundation Year (B340) 4FT/5FT Hon BSc/MSci
It seems that acupuncture hangs on in universities that are right at the bottom of the rankings.
Manchester Metropolitan gets the booby prize for actually starting a new course, just as all around are closing theirs. Dr Peter Banister, who was on the committee that approved the course (but now retired), has told me ” I am sceptical in the current economic climate whether it will prove to be successful”. Let’s hope he’s right.
But well done Westminster. Your position as the leader in antiscientific degrees has now been claimed by Middlesex University. Their "degrees" in Ayurveda mark out Middlesex University as the new King of Woo.
Over to you, Professor Driscoll. As vice-chancellor of Middlesex University, the buck stops with you.
Both still teach Chinese and herbal medicine, which are potentially dangerous. There is not a single product from either that has marketing authorisation from the MHRA, though the MHRA has betrayed its trust by allowing misleading labelling of herbal medicines without requiring any evidence whatsoever that they work, see, for example
Why degrees in Chinese medicine are a danger to patients
More quackedemia. Dangerous Chinese medicine taught at Middlesex University
Why does the MHRA refuse to label herbal products honestly? Kent Woods and Richard Woodfield tell me
Sub-degree courses
In contrast to the large reduction in the number of BSc and MSc degrees, there has actually been an increase in two year foundation degrees and HND courses in complementary medicine, at places right near the bottom of the academic heap. The subject is sinking to the bottom. With luck it will vanish entirely from universities before too long.
Research-intensive Universities
Although all of the degrees in magic medicine are from post-1992 universities, the subject has crept into more prestigious universities. Of these, the University of Southampton is perhaps the worst, because of the presence of George Lewith, and his defender, Stephen Holgate. Others have staunch defenders of quackery, including the University of Warwick, University of Edinburgh and St Batholomew’s.
Why have all these courses closed?
One reason is certainly the embarrassment caused by exposure of what’s taught on the courses. Professors Petts (Westminster) and Driscoll (Middlesex) must be aware that googling their names produces references to this and other skeptical blogs on the front page. Thanks to some plain brown emails, and, after a three year battle, the Freedom of Information Act, it has been possible to show here the nonsense that has been foisted on students by some universities. Not only is this a burden on the taxpayer, but, more importantly, some of it is a danger to patients.
When a course closes, it is often said that it is because of falling student numbers (though UCLAN and Salford did not use that excuse). Insofar as that is true, the credit must go to the whole of the skeptical movement that has grown so remarkably in the last few years. Ben Goldacre’s "ragged band of bloggers" have produced a real change in universities and in society as a whole.
The people who should have done the job have either been passive or an active hindrance. The list is long. Vice-chancellors and Universities UK (UUK), the Quality Assurance Agency (QAA), the Hiigher Education Funding Council England (HEFCE), Skills for Health, the Medicines and Health Regulatory Authority ( MHRA) , the Health Professions Council (HPC), the Department of Health, the Prince of Wales and his reincarnated propaganda organisation, the "College of Medicine", the King’s Fund, the Universities and Colleges Union (UCU), OfQual, Edexcel, National Occupational Standards and Qualifications and the Curriculum Authority (QCA).
Whatever happened to that "bonfire of the quangos"?
Follow-up
2 January 2012 The McTimoney College of Chiropractic (owned by BPP University) claims that its “validation” by the University of Wales will continue until 2017. This contradicts the statement from UoW. Watch this space.
3 January 2012. Thanks to Neil O’Connell for drawing my attention to a paper in Pain. The paper is particularly interesting because it comes from the Southampton group which has previously been sympathetic to acupuncture. Its authors include George Lewith. It shows, yet again that there is no detectable difference between real and sham acupuncture treatment. It also shows that the empathy of the practitioner has little effect: in fact the stern authoritarian practitioner may have been more effective.
Patients receiving acupuncture demonstrated clinically important improvements from baseline (i.e., a 29.5% reduction in pain), but despite this, acupuncture has no specific efficacy over placebo for this group of patients. The clinical effect of acupuncture treatment and associated controls is not related to the use of an acupuncture needle, nor mediated by empathy, but is practitioner related and may be linked to the perceived authority of the practitioner.”
Sadly. the trial didn’t include a no-treatment group, so it is impossible to say how much of the improvement is regression to the mean and how much is a placebo effect. The authors admit that it could be mostly the former.
Surely now the misplaced confidence in acupuncture shown by some medical and university people must be in tatters.
In yet another sign that even acupuncture advovates are beginning to notice that it doesn’t work, a recent article Paradoxes in Acupuncture Research: Strategies for Moving Forward, shows some fascinating squirming.
3 January 2012. The Daily Telegraph has carried a piece about closure of university courses, written by Michael Hanlon. On 31 January they carried a much longer piece.
3 January 2012. It is a great pity that some physiotherapists seem to have fallen hook, line and sinker for the myths of acupuncture. Physiotherapists are, by and large, the respectable face of manipulative therapy. Their evidence base is certainly not all one would wish, but at least they are free of the outrageous mumbo humbo of chiropractors. Well, most of them are, but not the Acupuncture Association of Chartered Physiotherapists (AACP), or, still worse, The Association of Chartered Physiotherapists in Energy Medicine, a group that is truly away with the fairies. These organisations are bringing a very respectable job into disrepute. And the Health Professions Council, which is meant to be their regulator, has, like most regulators, done nothing whatsoever to stop it.
5 January 2012. Times Higher Education gives a history of the demise of the University of Wales, Boom or Bust. It’s a useful timeline, but like so many journalists, it’s unwilling to admit that bloggers were on to the problem long before the BBC, never mind the QAA.
There was also a leader on the same topic, Perils of the export business. It again fails to take the QAA to task for its failures.
Interviews for Deutsche Welle and Middle East Broadcasting Center TV.
17 January 2012 Another question answered. I just learned that the ludicrous course in Nutritional Therapy, previously validated by the University of Wales (and a contributor to its downfall), is now being validated by, yes, you guessed, Middlesex University. Professor Driscoll seems determined to lead his univerity to the bottom of the academic heap. His new partnership with the Northern college of Acupuncture is just one of a long list of validations that almost rivals that of the late University of Wales. The course has, of course, an enthusiastic testimonial, from a student. It starts
I work full time as a team leader for a pension company but I am also a kinesiologist and work in my spare time doing kinesiology, reiki and Indian head massage.
Evidently she’s a believer in the barmiest and totally disproved forms of magic medicine. And Middlesex University will give her a Master of Science degree. I have to say I find it worrying that she’s a team leader for a pension company. Does she also believe in the value of worthless derivatives. I wonder?
18 January 2012. the story has gone international, with an interview that I did for Deutsche Welle, UK universities drop alternative medicine degree programs. I’m quoted as saying “They’re dishonest, they teach things that aren’t true, and things that are dangerous to patients in some cases”. That seems fair enough.
There is also an interesting item from July 2010 about pressure to drop payment for homeopathy by German health insurance
31 January 2012
The Daily Telegraph carried a prominent 1200 word account (the title wasn’t mine). The published version was edited slightly.
The offering of quack cancer treatments at an exorbitant price is simple cruelty. The nature of the Burzynski clinic has been known for some time. But it has come to a head with some utterly vile threatening letters sent to the admirable Andrew Lewis, because he told a few truths about Stanislaw Burzynski’s despicable outfit. Please read his original post, The False Hope of the Burzynski Clinic.
I have to add by two-pennorth worth to the row that has blown up in the blogosphere at the outrageous behaviour of Burzynski. I hope other bloggers will do the same. There is safety in numbers. We need a Streisand effect to face down these pathetic bullies. It’s the "I am Spartacus" principle.
I won’t repeat all the details. They have spread like wildfire round the web. Briefly, it was sparked off by tragic case of a 4-year old girl, Billie Bainbridge who has a rare form of brain cancer. Well-intentioned pop stars have been trying to raise £200,000 to "enrol her into a clinical trial" at Burzynski clinic in Texas, despite the fact that Dr Stanislaw Burzynski has already been on trial for cancer fraud. In fact his clinic is not allowed to treat cancer patients, but it has evaded that ban, for many years, by pretending to run clinical trials. Normally patients volunteer for clinical trials. Sometimes they are paid a modest amount. Never, in the civilised world, are people asked to pay hundreds of thousands of pounds to be a guinea pig. Dorothy Bishop has written about The Weird World of US ethics regulation.
There is nothing new about this. The Cancerbusters site won the Anus Maximus Award for the year 2000. The award was announced in the following words:
The top award this year goes to the acolytes of Dr Stanislaw Burzynski who have created an advertising site at www.cancerbusters.com using a five-year-old boy named Thomas Navarro. Thomas is dying of cancer and this site exploits that tragedy to try and get the law changed so that quacks can have the untrammelled right to deceive desperate, sick people by promising them magic cures for cancer, AIDS and other diseases for which no cure is yet available. While this site is specifically a Burzynski promotion, his competitors support the site and mention it because if the campaign is successful it will dramatically increase the size of the market for quackery and therefore their opportunities to make money. [The boy died in November 2001]
The letters sent to Andrew Lewis are unspeakably nasty. They come from someone who calls himself "Marc Stephens" who claims to represent the company.
|
Le Canard Noir / Andy Lewis, I represent the Burzynski Clinic, Burzynski Research Institute, and Dr. Stanislaw Burzynski. It has been brought to our attention that you have content on your websites http://www.quackometer.net/blog/2011/11/the-false-hope-of-the-burzynski-clinic.html that is in violation of multiple laws. Please allow this correspondence to serve as notice to you that you published libelous and defamatory information. This correspondence constitutes a demand that you immediately cease and desist in your actions defaming and libeling my clients. Please be advised that my clients consider the content of your posting to be legally actionable under numerous legal causes of action, including but not limited to: defamation Libel, defamation per se, and tortious interference with business contracts and business relationships. The information you assert in your article is factually incorrect, and posted with either actual knowledge, or reckless disregard for its falsity. The various terms you use in your article connote dishonesty, untrustworthiness, illegality, and fraud. You, maliciously with the intent to harm my clients and to destroy his business, state information which is wholly without support, and which damages my clients’ reputations in the community. The purpose of your posting is to create in the public the belief that my clients are disreputable, are engaged in on-going criminal activity, and must be avoided by the public. You have a right to freedom of speech, and you have a right to voice your opinion, but you do not have the right to post libelous statements regardless if you think its your opinion or not. You are highly aware of defamation laws. You actually wrote an article about defamation on your site. In addition, I have information linking you to a network of individuals that disseminate false information. So the courts will apparently see the context of your article, and your act as Malicious. You have multiple third parties that viewed and commented on your article, which clearly makes this matter defamation libel. Once I obtain a subpoena for your personal information, I will not settle this case with you. Shut the article down IMMEDIATELY. GOVERN YOURSELF ACCORDINGLY. Regards, Marc Stephens |
Then later, at the end of another “foam-flecked angry rant”
|
. . . If you had no history of lying, and if you were not apart of a fraud network I would take the time to explain your article word for word, but you already know what defamation is. I’ve already recorded all of your articles from previous years as well as legal notice sent by other attorneys for different matters. As I mentioned, I am not playing games with you. You have a history of being stubborn which will play right into my hands. Be smart and considerate for your family and new child, and shut the article down..Immediately. FINAL WARNING. Regards, Marc Stephens |
Despite the attempt at legal style, "Marc Stephens" is not registered as an attorney in Texas.
Andy Lewis did not yield to this crude bullying. His post is still there for all to read. Before the days of the internet he would have been on his own. But now already dozens of blogs have drawn attention to what’s going on. Soon it will be hundreds. Burzynski can’t sue all of us. It’s the Streisand effect, or the "I am Spartacus" response.
Come on. Marc Stephens, make my day.
Some notes on the science
The Burzynski treatment is piss. Literally. A mixture of substances extracted from the patient’s own urine is dubbed with the preoposterous pseudoscientific name "antineoplastons". There are no such things as "neoplastons". And the chemicals are now made in the lab like any other drug.
|
The main component seems to be a simple organic chemical, phenylacetic acid (PA). It is produced in normal metabolism but the liver copes with it by converting it to phenylacetyl glutamine (PAG), which is excreted in the urine.
|
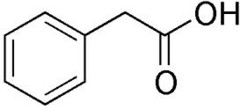
|
Saul Green has summarised the evidence
Burzynski has never demonstrated that A-2.1 (PA) or “soluble A-10” (PA and PAG) are effective against cancer or that tumor cells from patients treated with these antineoplastons have been “normalized.” Tests of antineoplastons at the National Cancer Institute have never been positive. The drug company Sigma-Tau Pharmaceuticals could not duplicate Burzynski’s claims for AS-2.1 and A-10. The Japanese National Cancer Institute has reported that antineoplastons did not work in their studies. No Burzynski coauthors have endorsed his use of antineoplastons in cancer patients.
Cancer Research UK has a summary of the current evidence, Hope or false hope?
Despite it being illegal to advertise cancer cures in most country, the list of people who flout the law to make money from the desperate is enormous/ You can find a list of them at Quackwatch. Burzynski isn’t the only one but he could well be the most expensive.
Latest developments
You can follow the ever-growing list of publications by people who are determined to resist Burzynski at Josephine Jones "Stanislaw, Streisand and Spartacus". There is also a list at anarchic_teapot’s blog
Follow-up
Saturday 26 November Another frothy threat from Burzynski’s alleged representative. Lot’s of RED ARROWS.
Monday 28 November The Streisand effect is developing rapidly. The definitive lists of posts are here and here. But there are two that I must mention.
Today Rhys Morgan has published Threats from The Burzynski Clinic. The same “Marc Stephens” has made the same sort of threats against him as he made against Lewis. Rhys Morgan is still at school, and is now 17 years old. He was the hero of the MMS scandal.
David Gorski, a real oncologist, has gone into the evidence in excellent detall with Stanislaw Burzynski: Bad medicine, a bad movie, and bad P.R.
I have in the past, taken an occasional interest in the philosophy of science. But in a lifetime doing science, I have hardly ever heard a scientist mention the subject. It is, on the whole, a subject that is of interest only to philosophers.
|
It’s true that some philosophers have had interesting things to say about the nature of inductive inference, but during the 20th century the real advances in that area came from statisticians, not from philosophers. So I long since decided that it would be more profitable to spend my time trying to understand R.A Fisher, rather than read even Karl Popper. It is harder work to do that, but it seemed the way to go.
|
 |
This post is based on the last part of chapter titled “In Praise of Randomisation. The importance of causality in medicine and its subversion by philosophers of science“. A talk was given at the meeting at the British Academy in December 2007, and the book will be launched on November 28th 2011 (good job it wasn’t essential for my CV with delays like that). The book is published by OUP for the British Academy, under the title Evidence, Inference and Enquiry (edited by Philip Dawid, William Twining, and Mimi Vasilaki, 504 pages, £85.00). The bulk of my contribution has already appeared here, in May 2009, under the heading Diet and health. What can you believe: or does bacon kill you?. It is one of the posts that has given me the most satisfaction, if only because Ben Goldacre seemed to like it, and he has done more than anyone to explain the critical importance of randomisation for assessing treatments and for assessing social interventions.
Having long since decided that it was Fisher, rather than philosophers, who had the answers to my questions, why bother to write about philosophers at all? It was precipitated by joining the London Evidence Group. Through that group I became aware that there is a group of philosophers of science who could, if anyone took any notice of them, do real harm to research. It seems surprising that the value of randomisation should still be disputed at this stage, and of course it is not disputed by anybody in the business. It was thoroughly established after the start of small sample statistics at the beginning of the 20th century. Fisher’s work on randomisation and the likelihood principle put inference on a firm footing by the mid-1930s. His popular book, The Design of Experiments made the importance of randomisation clear to a wide audience, partly via his famous example of the lady tasting tea. The development of randomisation tests made it transparently clear (perhaps I should do a blog post on their beauty). By the 1950s. the message got through to medicine, in large part through Austin Bradford Hill.
Despite this, there is a body of philosophers who dispute it. And of course it is disputed by almost all practitioners of alternative medicine (because their treatments usually fail the tests). Here are some examples.
“Why there’s no cause to randomise” is the rather surprising title of a report by Worrall (2004; see also Worral, 2010), from the London School of Economics. The conclusion of this paper is
“don’t believe the bad press that ‘observational studies’ or ‘historically controlled trials’ get – so long as they are properly done (that is, serious thought has gone in to the possibility of alternative explanations of the outcome), then there is no reason to think of them as any less compelling than an RCT.”
In my view this conclusion is seriously, and dangerously, wrong –it ignores the enormous difficulty of getting evidence for causality in real life, and it ignores the fact that historically controlled trials have very often given misleading results in the past, as illustrated by the diet problem.. Worrall’s fellow philosopher, Nancy Cartwright (Are RCTs the Gold Standard?, 2007), has made arguments that in some ways resemble those of Worrall.
Many words are spent on defining causality but, at least in the clinical setting the meaning is perfectly simple. If the association between eating bacon and colorectal cancer is causal then if you stop eating bacon you’ll reduce the risk of cancer. If the relationship is not causal then if you stop eating bacon it won’t help at all. No amount of Worrall’s “serious thought” will substitute for the real evidence for causality that can come only from an RCT: Worrall seems to claim that sufficient brain power can fill in missing bits of information. It can’t. I’m reminded inexorably of the definition of “Clinical experience. Making the same mistakes with increasing confidence over an impressive number of years.” In Michael O’Donnell’s A Sceptic’s Medical Dictionary.
At the other philosophical extreme, there are still a few remnants of post-modernist rhetoric to be found in obscure corners of the literature. Two extreme examples are the papers by Holmes et al. and by Christine Barry. Apart from the fact that they weren’t spoofs, both of these papers bear a close resemblance to Alan Sokal’s famous spoof paper, Transgressing the boundaries: towards a transformative hermeneutics of quantum gravity (Sokal, 1996). The acceptance of this spoof by a journal, Social Text, and the subsequent book, Intellectual Impostures, by Sokal & Bricmont (Sokal & Bricmont, 1998), exposed the astonishing intellectual fraud if postmodernism (for those for whom it was not already obvious). A couple of quotations will serve to give a taste of the amazing material that can appear in peer-reviewed journals. Barry (2006) wrote
“I wish to problematise the call from within biomedicine for more evidence of alternative medicine’s effectiveness via the medium of the randomised clinical trial (RCT).”
“Ethnographic research in alternative medicine is coming to be used politically as a challenge to the hegemony of a scientific biomedical construction of evidence.”
“The science of biomedicine was perceived as old fashioned and rejected in favour of the quantum and chaos theories of modern physics.”
“In this paper, I have deconstructed the powerful notion of evidence within biomedicine, . . .”
The aim of this paper, in my view, is not obtain some subtle insight into the process of inference but to try to give some credibility to snake-oil salesmen who peddle quack cures. The latter at least make their unjustified claims in plain English.
The similar paper by Holmes, Murray, Perron & Rail (Holmes et al., 2006) is even more bizarre.
“Objective The philosophical work of Deleuze and Guattari proves to be useful in showing how health sciences are colonised (territorialised) by an all-encompassing scientific research paradigm “that of post-positivism ” but also and foremost in showing the process by which a dominant ideology comes to exclude alternative forms of knowledge, therefore acting as a fascist structure. “,
It uses the word fascism, or some derivative thereof, 26 times. And Holmes, Perron & Rail (Murray et al., 2007)) end a similar tirade with
“We shall continue to transgress the diktats of State Science.”
It may be asked why it is even worth spending time on these remnants of the utterly discredited postmodernist movement. One reason is that rather less extreme examples of similar thinking still exist in some philosophical circles.
Take, for example, the views expressed papers such as Miles, Polychronis and Grey (2006), Miles & Loughlin (2006), Miles, Loughlin & Polychronis (Miles et al., 2007) and Loughlin (2007).. These papers form part of the authors’ campaign against evidence-based medicine, which they seem to regard as some sort of ideological crusade, or government conspiracy. Bizarrely they seem to think that evidence-based medicine has something in common with the managerial culture that has been the bane of not only medicine but of almost every occupation (and which is noted particularly for its disregard for evidence). Although couched in the sort of pretentious language favoured by postmodernists, in fact it ends up defending the most simple-minded forms of quackery. Unlike Barry (2006), they don’t mention alternative medicine explicitly, but the agenda is clear from their attacks on Ben Goldacre. For example, Miles, Loughlin & Polychronis (Miles et al., 2007) say this.
“Loughlin identifies Goldacre [2006] as a particularly luminous example of a commentator who is able not only to combine audacity with outrage, but who in a very real way succeeds in manufacturing a sense of having been personally offended by the article in question. Such moralistic posturing acts as a defence mechanism to protect cherished assumptions from rational scrutiny and indeed to enable adherents to appropriate the ‘moral high ground’, as well as the language of ‘reason’ and ‘science’ as the exclusive property of their own favoured approaches. Loughlin brings out the Orwellian nature of this manoeuvre and identifies a significant implication.”
If Goldacre and others really are engaged in posturing then their primary offence, at least according to the Sartrean perspective adopted by Murray et al. is not primarily intellectual, but rather it is moral. Far from there being a moral requirement to ‘bend a knee’ at the EBM altar, to do so is to violate one’s primary duty as an autonomous being.”
This ferocious attack seems to have been triggered because Goldacre has explained in simple words what constitutes evidence and what doesn’t. He has explained in a simple way how to do a proper randomised controlled trial of homeopathy. And he he dismantled a fraudulent Qlink pendant, purported to shield you from electromagnetic radiation but which turned out to have no functional components (Goldacre, 2007). This is described as being “Orwellian”, a description that seems to me to be downright bizarre.
In fact, when faced with real-life examples of what happens when you ignore evidence, those who write theoretical papers that are critical about evidence-based medicine may behave perfectly sensibly. Although Andrew Miles edits a journal, (Journal of Evaluation in Clinical Practice), that has been critical of EBM for years. Yet when faced with a course in alternative medicine run by people who can only be described as quacks, he rapidly shut down the course (A full account has appeared on this blog).
It is hard to decide whether the language used in these papers is Marxist or neoconservative libertarian. Whatever it is, it clearly isn’t science. It may seem odd that postmodernists (who believe nothing) end up as allies of quacks (who’ll believe anything). The relationship has been explained with customary clarity by Alan Sokal, in his essay Pseudoscience and Postmodernism: Antagonists or Fellow-Travelers? (Sokal, 2006).
Conclusions
Of course RCTs are not the only way to get knowledge. Often they have not been done, and sometimes it is hard to imagine how they could be done (though not nearly as often as some people would like to say).
It is true that RCTs tell you only about an average effect in a large population. But the same is true of observational epidemiology. That limitation is nothing to do with randomisation, it is a result of the crude and inadequate way in which diseases are classified (as discussed above). It is also true that randomisation doesn’t guarantee lack of bias in an individual case, but only in the long run. But it is the best that can be done. The fact remains that randomization is the only way to be sure of causality, and making mistakes about causality can harm patients, as it did in the case of HRT.
Raymond Tallis (1999), in his review of Sokal & Bricmont, summed it up nicely
“Academics intending to continue as postmodern theorists in the interdisciplinary humanities after S & B should first read Intellectual Impostures and ask themselves whether adding to the quantity of confusion and untruth in the world is a good use of the gift of life or an ethical way to earn a living. After S & B, they may feel less comfortable with the glamorous life that can be forged in the wake of the founding charlatans of postmodern Theory. Alternatively, they might follow my friend Roger into estate agency — though they should check out in advance that they are up to the moral rigours of such a profession.”
The conclusions that I have drawn were obvious to people in the business a half a century ago. (Doll & Peto, 1980) said
“If we are to recognize those important yet moderate real advances in therapy which can save thousands of lives, then we need more large randomised trials than at present, not fewer. Until we have them treatment of future patients will continue to be determined by unreliable evidence.”
The towering figures are R.A. Fisher, and his followers who developed the ideas of randomisation and maximum likelihood estimation. In the medical area, Bradford Hill, Archie Cochrane, Iain Chalmers had the important ideas worked out a long time ago.
In contrast, philosophers like Worral, Cartwright, Holmes, Barry, Loughlin and Polychronis seem to me to make no contribution to the accumulation of useful knowledge, and in some cases to hinder it. It’s true that the harm they do is limited, but that is because they talk largely to each other. Very few working scientists are even aware of their existence. Perhaps that is just as well.
References
Cartwright N (2007). Are RCTs the Gold Standard? Biosocieties (2007), 2: 11-20
Colquhoun, D (2010) University of Buckingham does the right thing. The Faculty of Integrated Medicine has been fired. https://www.dcscience.net/?p=2881
Miles A & Loughlin M (2006). Continuing the evidence-based health care debate in 2006. The progress and price of EBM. J Eval Clin Pract 12, 385-398.
Miles A, Loughlin M, & Polychronis A (2007). Medicine and evidence: knowledge and action in clinical practice. J Eval Clin Pract 13, 481-503.
Miles A, Polychronis A, & Grey JE (2006). The evidence-based health care debate – 2006. Where are we now? J Eval Clin Pract 12, 239-247.
Murray SJ, Holmes D, Perron A, & Rail G (2007).
Deconstructing the evidence-based discourse in health sciences: truth, power and fascis. Int J Evid Based Healthc 2006; : 4, 180–186.
Sokal AD (1996). Transgressing the Boundaries: Towards a Transformative Hermeneutics of Quantum Gravity. Social Text 46/47, Science Wars, 217-252.
Sokal AD (2006). Pseudoscience and Postmodernism: Antagonists or Fellow-Travelers? In Archaeological Fantasies, ed. Fagan GG, Routledge,an imprint of Taylor & Francis Books Ltd.
Sokal AD & Bricmont J (1998). Intellectual Impostures, New edition, 2003, Economist Books ed. Profile Books.
Tallis R. (1999) Sokal and Bricmont: Is this the beginning of the end of the dark ages in the humanities?
Worrall J. (2004) Why There’s No Cause to Randomize. Causality: Metaphysics and Methods.Technical Report 24/04 . 2004.
Worrall J (2010). Evidence: philosophy of science meets medicine. J Eval Clin Pract 16, 356-362.
Follow-up
Iain Chalmers has drawn my attention to a some really interesting papers in the James Lind Library
An account of early trials is given by Chalmers I, Dukan E, Podolsky S, Davey Smith G (2011). The adoption of unbiased treatment allocation schedules in clinical trials during the 19th and early 20th centuries. Fisher was not the first person to propose randomised trials, but he is the person who put it on a sound mathematical basis.
Another fascinating paper is Chalmers I (2010). Why the 1948 MRC trial of streptomycin used treatment allocation based on random numbers.
The distinguished statistician, David Cox contributed, Cox DR (2009). Randomization for concealment.
Incidentally, if anyone still thinks there are ethical objections to random allocation, they should read the account of retrolental fibroplasia outbreak in the 1950s, Silverman WA (2003). Personal reflections on lessons learned from randomized trials involving newborn infants, 1951 to 1967.
Chalmers also pointed out that Antony Eagle of Exeter College Oxford had written about Goldacre’s epistemology. He describes himself as a “formal epistemologist”. I fear that his criticisms seem to me to be carping and trivial. Once again, a philosopher has failed to make a contribution to the progress of knowledge.
There’s been no official announcement, but four more of Westminster’s courses in junk medicine have quietly closed.
For entry in 2011 they offer
| University of Westminster (W50) | qualification |
| Chinese Medicine: Acupuncture (B343) | 3FT Hon BSc |
| Chinese Medicine: Acupuncture with Foundation (B341) | 4FT/5FT Hon BSc/MSci |
| Complementary Medicine (B255) | 3FT Hon BSc |
| Complementary Medicine (B301) | 4FT Hon MHSci |
| Complementary Medicine: Naturopathy (B391) | 3FT Hon BSc |
| Herbal Medicine (B342) | 3FT Hon BSc |
| Herbal Medicine with Foundation Year (B340) | 4FT/5FT Hon BSc/MSci |
| Nutritional Therapy (B400) | 3FT Hon BSc |
But for entry in 2012
| University of Westminster (W50) | qualification |
| Chinese Medicine: Acupuncture (B343) | 3FT Hon BSc |
| Chinese Medicine: Acupuncture with Foundation (B341) | 4FT/5FT Hon BSc/MSci |
| Herbal Medicine (B342) | 3FT Hon BSc |
| Herbal Medicine with Foundation Year (B340) | 4FT/5FT Hon BSc/MSc |
At the end of 2006, Westminster was offering 14 different BSc degrees in seven flavours of junk medicine. In October 2008, it was eleven. This year it’s eight, and next year only four degrees in two subjects. Since "Integrated Health" was ‘merged’ with Biological Sciences in May 2010, two of the original courses have been dropped each year. This September there will be a final intake for Nutrition Therapy and Naturopathy. That leaves only two, Chinese Medicine (acupuncture and (Western) Herbal Medicine.
The official reason given for the closures is always that the number of applications has fallen. I’m told that the number of applications has halved over the last five or six years. If that’s right, it counts as a big success for the attempts of skeptics to show the public the nonsense that’s taught on these degrees. Perhaps it is a sign that we are emerging from the endarkenment.
Rumour has it that the remaining degrees will eventually close too. Let’s hope so. Meanwhile, here is another helping hand.
There is already quite a bit here about the dangers of Chinese medicine, e.g. here and, especially, here. A submission to the Department of Health gives more detail. There has been a lot on acupuncture here too. There is now little doubt that it’s no more than a theatrical, and not very effective, placebo. So this time I’ll concentrate on Western herbal medicine.
Western Herbal Medicine
Herbal medicine is just a branch of pharmacology and it could be taught as such. But it isn’t. It comes overlaid with much superstitious nonsense. Some of it can be seen in slides from Edinburgh Napier University (the difference being that Napier closed that course, and Westminster hasn’t)
Even if it were taught properly, it wouldn’t be appropriate for a BSc for several reasons.
First, there isn’t a single herbal that has full marketing authorisation from the MHRA. In other words, there isn’t a single herb for which there is good evidence that it works to a useful extent.
Second, the fact that the active principals in plants are virtually always given in an unknown dose makes them potentially dangerous. This isn’t 1950s pharmacology. It’s 1920s pharmacology, dating from a time before methods were worked out for standardising the potency of natural products (see Plants as Medicines).
Third, if you are going to treat illness with chemicals, why restrict yourself to chemicals that occur in plants?
It was the herbal medicine course that gave rise to the most virulent internal complaints at the University of Westminster. These complaints revealed the use of pendulum dowsing by some teachers on the course and the near-illegal, and certainly dangerous, teaching about herbs in cancer.
Here are a few slides from Principles of Herbal Medicine(3CT0 502). The vocabulary seems to be stuck in a time warp. When I first started in the late 1950s, words like tonic, carminative, demulcent and expectorant were common Over the last 40 years all these words have died out in pharmacology, for the simple reason that it became apparent that there were no such actions. But these imaginary categories are still alive and well in the herbal world.
There was a lecture on a categories of drugs so old-fashioned that I’ve never even heard the words: "nervines". and "adaptogens".
 |
  |
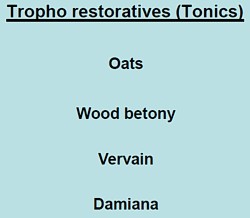 |
The "tonics" listed here seem quite bizarre. In the 1950s, “tonics” containing nux vomica (a small dose of strychnine) and gentian (tastes nasty) were common, but they vanished years ago, because they don’t work. None of those named here even get a mention in NCCAM’s Herbs-at-a-glance. Oats? Come on! |
|
The only ‘relaxant’ here for which there is the slightest evidence is Valerian. I recall tincture of Valerian in a late 1950s pharmacy. It smells terrible, According to NCCAM
Not much, for something that’s been around for centuries. And for chamomile
None of this near-total lack of evidence is mentioned on the slides. |
 |
What about the ‘stimulants‘? Rosemary? No evidence at all. Tea and coffee aren’t medicine (and not very good stimulants for me either).
|
Ginseng, on the other hand, is big business. That doesn’t mean it works of course. NCCAM says of Asian ginseng (Panax Ginseng).
|
 |
Thymoleptics – antidepressants are defined as "herbs that engender a feeling of wellbeing. They uplift the spirit, improve the mood and counteract depression".
Oats, Lemon balm, Damiana, Vervain. Lavender and Rosemary are just old bits of folklore
|
 |
The only serious contender here is St John’s Wort. At one time this was the prize exhibit for herbalists. It has been shown to be as good as the conventional SSRIs for treatment of mild to moderate depression. Sadly it has turned out that the SSRIs are themselves barely better than placebos. NCCAM says
- There is scientific evidence that St. John’s wort may be useful for short-term treatment of mild to moderate depression. Although some studies have reported benefits for more severe depression, others have not; for example, a large study sponsored by NCCAM found that the herb was no more effective than placebo in treating major depression of moderate severity.
"Adaptogens" are another figment of the herbalists’ imaginations. They are defined in the lecture thus.
|

|
Well, it would be quite nice if such drugs existed. Sadly they don’t.
- The evidence for using astragalus for any health condition is limited. High-quality clinical trials (studies in people) are generally lacking.
Another lecture dealt with "stimulating herbs". No shortage of them, it seems.

Well at least one of these has quite well-understood effects in pharmacology, ephedrine, a sympathomimetic amine. It isn’t used much because it can be quite dangerous, even with the controlled dose that’s used in real medicine. In the uncontrolled dose in herbal medicines it is downright dangerous.

|

|

|
|
This is what NCCAM says about Ephedra
- An NCCAM-funded study that analyzed phone calls to poison control centers found a higher rate of side effects from ephedra, compared with other herbal products.
- Other studies and systematic reviews have found an increased risk of heart, psychiatric, and gastrointestinal problems, as well as high blood pressure and stroke, with ephedra use.
- According to the U.S. Food and Drug Administration (FDA), there is little evidence of ephedra’s effectiveness, except for short-term weight loss. However, the increased risk of heart problems and stroke outweighs any benefits.
It seems that what is taught in the BSc Herbal Medicine degree consists largely of folk-lore and old wives’ tales. Some of it could be quite dangerous for patients.
A problem for pharmacognosists
While talking about herbal medicine, it’s appropriate to mention a related problem, though it has nothing to do with the University of Westminster.
My guess is that not many people have even heard of pharmacognosy. If it were not for my humble origins as an apprentice pharmacist in Grange Road, Birkenhead (you can’t get much more humble than that) I might not know either.
Pharmacognosy is a branch of botany, the study of plant drugs. I recall inspecting powered digitalis leaves under a microscope. In Edinburgh, in the time of the great pharmacologist John Henry Gaddum, medical students might be presented in the oral exam with a jar of calabar beans and required to talk about their anticholinesterase effects of the physostigmine that they contain.
The need for pharmacognosy has now all but vanished, but it hangs on in the curriculum for pharmacy students. This has engendered a certain unease about the role of pharmacognists. They often try to justify their existence by rebranding themselves as "phytotherapists". There are even journals of phytotherapy. It sounds a lot more respectable that herbalism. At its best, it is more respectable, but the fact remains that there no herbs whatsoever that have well-documented medical uses.
The London School of Pharmacy is a case in point. Simon Gibbons (Professor of Phytochemistry, Department of Pharmaceutical and Biological Chemistry). The School of Pharmacy) has chosen, for reasons that baffle me, to throw in his lot with the reincarnated Prince of Wales Foundation known as the “College of Medicine“. That organisation exists largely (not entirely) to promote various forms of quackery under the euphemism “integrated medicine”. On their web site he says "Western science is now recognising the extremely high value of herbal medicinal products . . .", despite the fact that there isn’t a single herbal preparation with efficacy sufficient for it to get marketing authorisation in the UK. This is grasping at straws, not science.
The true nature of the "College of Medicine" is illustrated, yet again, by their "innovations network". Their idea of "innovation" includes the Bristol Homeopathic Hospital and the Royal London Hospital for Integrated medicine, both devoted to promoting the utterly discredited late-18th century practice of giving people pills that contain no medicine. Some "innovation".
It baffles me that Simon Gibbons is willing to appear on the same programme as Simon Mills and David Peters, and George Lewith. Mills’ ideas can be judged by watching a video of a talk he gave in which he ‘explains’ “hot and cold herbs”. It strikes me as pure gobbledygook. Make up your own mind. He too has rebranded himself as "phytotherapist" though in fact he’s an old-fashioned herbalist with no concern for good evidence. David Peters is the chap who, as Clinical Director of the University of Westminster’s ever-shrinking School of Quackery, tolerates dowsing as a way to select ‘remedies’.
The present chair of Pharmacognosy at the School of Pharmacy is Michael Heinrich. He, with Simon Gibbons, has written a book Fundamentals of pharmacognosy and phytotherapy. As well as much good chemistry, it contains this extraordinary statement
“TCM [traditional Chinese medicine] still contains very many remedies which were selected by their symbolic significance rather than their proven effects; however this does not mean that they are all ‘quack’remedies! There may even be some value in medicines such as tiger bone, bear gall, turtle shell, dried centipedes, bat dung and so on. The herbs, however, are well researched and are becoming increasingly popular as people become disillusioned with Western Medicine.”
It is irresponsible to give any solace at all to the wicked industries that kill tigers and torture bears to extract their bile. And it is simple untrue that “herbs are well-researched”. Try the test,
A simple test for herbalists. Next time you encounter a herbalist, ask them to name the herb for which there is the best evidence of benefit when given for any condition. Mostly they refuse to answer, as was the case with Michael McIntyre (but he is really an industry spokesman with few scientific pretensions). I asked Michael Heinrich, Professor of Pharmacognosy at the School of Pharmacy. Again I couldn’t get a straight answer. Usually, when pressed, the two things that come up are St John’s Wort and Echinacea. Let’s see what The National Center for Complementary and Alternative Medicine (NCCAM) has to say about them. NCCAM is the branch of the US National Institutes of Health which has spent around a billion dollars of US taxpayers’ money on research into alternative medicine, For all that effort they have failed to come up with a single useful treatment. Clearly they should be shut down. Nevertheless, as an organisation that is enthusiastic about alternative medicine, their view can only be overoptimistic.
For St John’s Wort . NCCAM says
- There is scientific evidence that St. John’s wort may be useful for short-term treatment of mild to moderate depression. Although some studies have reported benefits for more severe depression, others have not; for example, a large study sponsored by NCCAM found that the herb was no more effective than placebo in treating major depression of moderate severity.
For Echinacea NCCAM says
- Study results are mixed on whether echinacea can prevent or effectively treat upper respiratory tract infections such as the common cold. For example, two NCCAM-funded studies did not find a benefit from echinacea, either as Echinacea purpurea fresh-pressed juice for treating colds in children, or as an unrefined mixture of Echinacea angustifolia root and Echinacea purpurea root and herb in adults. However, other studies have shown that echinacea may be beneficial in treating upper respiratory infections.
If these are the best ones, heaven help the rest.
Follow-up
On 23rd May 2008 a letter was sent to the vice-chancellor of the University of Westminster, Professor Geoffrey Petts
|
 |
Despite reminders, we were never afforded the courtesy of a reply to this, or any other letter.
Professor Petts has, however, replied to a letters sent to him recently by the Nightingale Collaboration. He said
“Whilst I understand your concerns, colleagues of the School of Life Sciences where these courses are offered do not share them. They are not teaching pseudo-science, as you claim,…”.
Neither of thse claims is true.I know at least two members of the Life Sciences Faculty who are very worried. One has now left and one has retired. The rest are presumably too scared to speak out.
It is most certainly not true to say they "are not teaching pseudo-science". Both the vice-chancellor and the Dean of Life Sciences, Jane Lewis, have been made aware of what;s happening repeatedly over several years, I can think of no other way to put it but to say Professor Petts is lying. Tha is not a good thing for vice-chancellors to do.
Much of what is taught at Westminster has now been revealed. This seems like a good moment to summarise what we know. Searching this blog for "University of Westminster" yields 39 hits. Of these, 11 show what’s taught at Westminster, so I’ll summarise them here for easy reference.
March 26th, 2007
The day after “Science degrees without the Science“ appeared in Nature, the University of Westminster issued a statement (now vanished, but see debate in THE). In my view, their statement provides the strongest grounds so far to believe that the BSc is inappropriate.
Let’s take a look at it.
|
“The BSc (Hons) Health Sciences: Homeopathy is a fully validated degree that satisfies internal and external quality assurance standards.”
|
Since that time, the university has closed down the BSc in Homeopathy. I have now seen many such validation documents and they are mostly box ticking exercises, not worth the paper they are written on. The worst offender is the University or Wales.
Westminster University BSc: “amethysts emit high yin energy”
April 23rd, 2008
http://dcscience.net/vib-therapies-43s.jpg
|
This shows the first set of slides that I got from Westminster (leaked by an angry insider). It has slides on crystal healing and dowsing, things that are at the lunatic fringe even by the standards of alternative medicine. it also relates that an academic who invited me to give a talk at the University of Westminster on the evidence for alternative medal was leaned on heavily by “VC, Provosts and Deans” to prevent that talk taking place. |

|
Crystal balls. Professor Petts in Private Eye
February 19th, 2009
Professor Petts makes an appearance in Private Eye. It could held that this counts as bringing your university into disrepute.
February 24th, 2009
BSc courses in homeopathy are closing. Is it a victory for campaigners, or just the end of the Blair/Bush era?
|
Professor Petts of Westminster seems to think that the problem can be solved by putting more science into the courses The rest of the world realises that as soon as you apply science to homeopathy or naturopathy, the whole subject vanishes in a puff of smoke, I fear that Professor Petts will have to do better,
|
 |
The Guardian carries a nice article by Anthea Lipsett, The Opposite of Science (or download pdf of print version).
The last BSc (Hons) Homeopathy closes! But look at what they still teach at Westminster University.
March 30th, 2009
In March 2007 I wrote a piece in Nature on Science degrees without the science. At that time there were five “BSc” degrees in homeopathy. A couple of weeks ago I checked the UCAS site for start in 2009, and found there was only one full “BSc (hons)” left and that was at Westminster University.
Today I checked again and NOW THERE ARE NONE.
A phone call to the University of Westminster tonight confirmed that they have suspended entry to their BSc (Hons) homeopathy degree.
Then I revealed another set of slides, showing a misunderstanding (by the teacher) of statistics, but most chillingly,some very dangerous ideas conveyed to students by Westminster’s naturopaths, and in the teaching of Traditional Chinese Medicine, and the great “detox” scam.

“if you get tuberculosis, it isn’t caused by Mycobacterium tuberculosis? And the symptoms are “constructive”? So you don’t need to do anything. It’s all for the best really.
This isn’t just nonsense. It’s dangerous nonsense.”
“Remember when shopping to favour fruits and vegetables which are in season and locally grown (and ideally organic) as they are more vibrationally compatible with the body.”
Locally grown vegetables are “more vibrationally compatible with the body”? Pure mystical gobbledygook. Words fail me.
More make-believe from the University of Westminster. This time it’s Naturopathy
June 25th, 2009
|
Some truly mind-boggling stuff that’s taught to students at Westminster, It includes "Emotrance". A primer on Emotrance says |
 |
"And then I thought of the lady in the supermarket whose husband had died, and I spend the following time sending her my best wishes, and my best space time quantum healing efforts for her void."
Then there are slides on pendulum diagnosis and “kinesiology”, a well-known fraudulent method of diagnosis. It is all perfectly mad.
Why degrees in Chinese medicine are a danger to patients
August 10th, 2009
More lunatic fantasies from Westminster, this time about Chinese medicine.
“Teaching students that the brain is made of marrow is not just absurd, but desperately dangerous for anyone unlucky (or stupid) enough to go to such a person when they are ill.”
|
There is a lot of stuff about cancer that is potentially homicidal.
|
 |
This is outrageous and very possibly illegal under the Cancer Act (1939). It certainly poses a huge danger to patients. It is a direct incentive to make illegal, and untrue claims by using weasel words in an attempt to stay just on the right side of the law. But that, of course, is standard practice in alternative medicine,
Emergent Chinese Omics at the University of Westminster/p>
August 27th, 2010
Systems biology is all the rage, No surprise then, to see the University of Westminster advertising a job for a systems biologist in the The Department of Molecular and Applied Biosciences. Well, no surprise there -until you read the small print.
Much has been written here about the University of Westminster, which remains the biggest provider of junk science degrees in the UK, despite having closed two of them.
If there is one thing more offensive than the use of meaningless mystical language, it is the attempt to hijack the vocabulary of real science to promote nonsense. As soon as a quack uses the words "quantum", "energy", "vibration", or now, "systems biology", you can be sure that it’s pretentious nonsense.
Hot of the press. Within a few hours of posting this, I was told that Volker Scheid, the man behind the pretentious Chinese medidine omics nonsense has been promoted to a full chair, And the Dean, Jane Lewis has congratulated him for speaking at a Chines Medicine symposium. Even quite sensible people like Lewis are being corrupted. The buck stops with Petts.
May 3rd, 2011
|
Yet more ghastly slides that are inflicted on Westminster students. How’s this for sheer barminess, taught as part of a Bachelor of Science degree? |
|
And
" Just in case you happen to have run out of Alaskan Calling All Angels Essence, you can buy it from Baldwin’s for £19.95. It’s “designed to invoke the nurturing, uplifting and joyful qualities of the angelic kingdom.”, and what’s more “can also use them any time to cleanse, energize, and protect your auric field.” Well that’s what it says.in the ad.
June 20th, 2011
This post gives details of two complaints, one from a student and one from a lecturer. The vice-chancellor certainly knows about them. So why, I wonder, did he say "“Whilst I understand your concerns, colleagues of the School of Life Sciences where these courses are offered do not share them.". He must know that this simply isn’t true. It is over a year now ( 10 July 2009 ) that a lecturer wrote to the vice-chancellor and Dean
|
“I expect that were the Department of Health to be aware of the unscientific teaching and promotion of practices like dowsing, (and crystals, iridology, astrology, and tasting to determine pharmacological qualities of plant extracts) on the Wmin HM [Westminster Herbal Medicine] Course, progress towards the Statutory Regulation of Herbal Medicine could be threatened.”
|
There’s only one thing wrong with this. The lecturer underestimated the stupidiity of the Department of Health which went ahead with statutory regulation despite being made aware of what was going on.
The latest example to come to light is cited by Andy Lewis on his Quackometer blog
“There are some even odder characters too, such as Roy Riggs B.Sc who describes himself as a “Holistic Geobiologist” and is “an “professional Earth Energy dowser”. He guest lectures at the London Westminster University’s School of Integrative Medicine and The Baltic Dowser’s Association of Lithuania.”
I do wonder who Professor Petts thinks he’s fooling. His denial of the obvious fact that his university is teaching pseudo-science serves only to discredit further the University of Westminster and his own integrity.
Follow-up
13 August 2011 I’m intrigued to notice that two days after posting this summary, googling “Geoffrey Petts” brings up this post as #3 on the first page. Actions have consequences.
Almost all the revelations about what’s taught on university courses in alternative medicine have come from post-1992 universities. (For readers not in the UK, post-1992 universities are the many new univerities created in 1992, from former polytechnics etc, and Russell group universities are the "top 20" research-intensive universities)
It is true that all the undergraduate courses are in post-1992 universities, but the advance of quackademia is by no means limited to them. The teaching at St Bartholomew’s Hospital Medical School, one of the oldest, was pretty disgraceful for example, though after protests from their own students, and from me, it is now better, I believe.

Quackery creeps into all universities to varying extents. The good ones (like Southampton) don’t run "BSc" degrees, but it still infiltrates through two main sources,
The first is via their HR departments, which are run by people who tend to be (I quote) "credulous and moronic" when it comes to science.
The other main source is in teaching to medical students. The General Medical Council says that medical students must know something about alterantive medicine and that’s quite right, A lot of their patients will use it. The problem is that the guidance is shockingly vague .
“They must be aware that many patients are interested in and choose to use a range of alternative and complementary therapies. Graduates must be aware of the existence and range of such therapies, why some patients use them, and how these might affect other types of treatment that patients are receiving.” (from Tomorrow’s Doctors, GMC)
In many medical schools, the information that medical students get is quite accurate. At UCL and at King’s (London) I have done some of the familiarisation myself. In other good medical schools, the students get some shocking stuff. St Bartholomew’s Hospital medical School was one example. Edinburgh University was another.
But there is one Russell group university where alternative myths are propagated more than any other that I know about. That is the University of Southampton.
In general, Southampton is a good place, I worked there for three years myself (1972 – 1975). The very first noise spectra I measured were calculated on a PDP computer in their excellent Institute of Sound and Vibration Research, before I wrote my own programs to do it.
But Southanpton also has a The Complementary and Integrated Medicine Research Unit . Oddly the unit’s web site, http://www.cam-research-group.co.uk, is not a university address, and a search of the university’s web site for “Complementary and Integrated Medicine Research Unit” produces no result. Nevertheless the unit is “within the School of Medicine at the University of Southampton”
Notice the usual euphemisms ‘complementary’ and ‘integrated’ in the title: the word ‘alternative’ is never used. This sort of word play is part of the bait and switch approach of alternative medicine.
The unit is quite big: ten research staff, four PhD students and two support staff It is headed by George Lewith.
Teaching about alternative medicine to Southampton medical students.
The whole medical class seems to get quite a lot compared with other places I know about. That’s 250 students (210 on the 5-year course plus another 40 from the 4-year graduate-entry route).
Year 1: Lecture by David Owen on ‘holism’ within the Foundation Course given to all 210 medical students doing the standard (5-year) course.
Year 2: Lecture by Lewith (on complementary medicine, focusing on acupuncture for pain) given within the nervous systems course to the whole medical student year-group (210 students).
Year 3 SBOM (scientific basis of medicine) symposium: The 3-hour session (“Complementary or Alternative Medicine: You Decide”). I’m told that attendance at this symposium is often pretty low, but many do turn up and all of them are officially ‘expected’ to attend.
There is also an optional CAM special study module chosen by 20 students in year 3, but also a small number of medical students (perhaps 2 – 3 each year?) choose to do a BMedSci research project supervised by the CAM research group and involving 16-18 weeks of study from October to May in Year 4. The CAM research group also supervise postgraduate students doing PhD research.
As always, a list of lectures doesn’t tell you much. What we need to know is what’s taught to the students and something about the people who teach it. The other interesting question is how it comes about that alternative medicine has been allowed to become so prominent in a Russell group university. It must have support from on high. In this case it isn’t hard to find out where it comes from. Here are some details.
Year 1 Dr David Owen
David Owen is not part of Lewith’s group, but a member of the Division of Medical Education headed by Dr Faith Hill (of whom, more below). He’s one of the many part-time academics in this area, being also a founder of The Natural Practice .
Owen is an advocate of homeopathy (a past president of the Faculty of Homeopathy). Homeopathy is, of course, the most barmy and discredited of all the popular sorts of alternative medicine. Among those who have discredited it is the head of the alt med unit, George Lewith himself (though oddly he still prescribes it).
And he’s also a member of the British Society of Environmental Medicine (BSEM). That sounds like a very respectable title, but don’t be deceived. It is an organisation that promotes all sorts of seriously fringe ideas. All you have to do is notice that the star speaker at their 2011 conference was none other than used-to-be a doctor, Andrew Wakefield, a man who has been responsible for the death of children from measles by causing an unfounded scare about vaccination on the basis of data that turned out to have been falsified. There is still a letter of support for Wakefield on the BSEM web site.
The BSEM specialises in exaggerated claims about ‘environmental toxins’ and uses phony allergy tests like kinesiology and the Vega test that misdiagnose allergies, but provide en excuse to prescribe expensive but unproven nutritional supplements, or expensive psychobabble like "neuro-linguistic programming".
Other registered "ecological physicians" include the infamous Dr Sarah Myhill, who, in 2010, was the subject of a damning verdict by the GMC, and Southampton’s George Lewith.
If it is wrong to expose medical students to someone who believes that dose-response curves have a negative slope (the smaller the dose the bigger the effect -I know, it’s crazy), then it is downright wicked to expose students to a supporter of Andrew Wakefield.
David Owen’s appearance on Radio Oxford, with the indomitable Andy Lewis appears on his Quackometer blog.
Year 2 Dr George Lewith
Lewith is a mystery wrapped in an enigma. He’s participated in some research that is quite good by the (generally pathetic) standards of the world of alternative medicine.
In 2001 he showed that the Vega test did not work as a method of allergy diagnosis. "Conclusion Electrodermal testing cannot be used to diagnose environmental allergies", published in the BMJ .[download reprint].
In 2003 he published "A randomized, double-blind, placebo-controlled proving trial of Belladonna 30C” [download reprint] that showed homeopathic pills with no active ingredients had no effects: The conclusion was "”Ultramolecular homeopathy has no observable clinical effects" (the word ultramolecular, in this context, means that the belladonna pills contained no belladonna).
In 2010 he again concluded that homeopathic pills were no more than placebos, as described in Despite the spin, Lewith’s paper surely signals the end of homeopathy (again). [download reprint]
What i cannot understand is that, despite his own findings, his private practice continues to prescribe the Vega machine and continues to prescribe homeopathic pills. And he continues to preach this subject to unfortunate medical students.
Lewith is also one of the practitioners recommended by BSEM. He’s a director of the "College of Medicine". And he’s also an advisor to a charity called Yes To Life. (see A thoroughly dangerous charity: YesToLife promotes nonsense cancer treatments).
3rd year Student Selected Unit
The teaching team includes:
- David Owen – Principal Clinical Teaching Fellow SoM, Holistic Physician
- George Lewith – Professor of Health Research and Consultant Physician
- Caroline Eyles – Homeopathic Physician
- Susan Woodhead – Acupuncturist
- Elaine Cooke – Chiropractic Practitioner
- Phine Dahle – Psychotherapist
- Keith Carr – Reiki Master
- Christine Rose – Homeopath and GP
- David Nicolson – Nutritionalist
- Shelley Baker – Aromatherapist
- Cheryl Dunford – Hypnotherapist
- Dedj Leibbrandt – Herbalist
More details of the teaching team here. There is not a single sceptic among them, so the students don’t get a debate, just propaganda.
In this case. there’s no need for the Freedom of Information Act. The handouts. and the powerpoints are on their web site. They seem to be proud of them
Let’s look at some examples
Chiropractic makes an interesting case, because, in the wake of the Singh-BCA libel case, the claims of chiropractors have been scrutinised as never before and most of their claims have turned out to be bogus. There is a close relationship between Lewith’s unit and the Anglo-European Chiropractic College (the 3rd year module includes a visit there). In fact the handout provided for students, Evidence for Chiropractic Care , was written by the College. It’s interesting because it provides no real evidence whatsoever for the effectiveness of chiropractic care. It’s fairly honest in stating that the view at present is that, for low back pain, it isn’t possible to detect any difference between the usefulness of manipulation by a physiotherapist, by an osteopath or by a chiropractor. Of course it does not draw the obvious conclusion that this makes chiropractic and osteopathy entirely redundant -you can get the same result without all the absurd mumbo jumbo that chiropractors and osteopaths love, or their high-pressure salesmanship and superfluous X-rays. Neither does it mention the sad, but entirely possible, outcome that none of the manipulations are effective for low back pain. There is, for example, no mention of the fascinating paper by Artus et al [download reprint]. This paper concludes
"symptoms seem to improve in a similar pattern in clinical trials following a wide
variety of active as well as inactive treatments."
This paper was brought to my attention through the blog run by the exellent physiotherapist, Neil O’Connell. He comments
“If this finding is supported by future studies it might suggest that we can’t even claim victory through the non-specific effects of our interventions such as care, attention and placebo. People enrolled in trials for back pain may improve whatever you do. This is probably explained by the fact that patients enrol in a trial when their pain is at its worst which raises the murky spectre of regression to the mean and the beautiful phenomenon of natural recovery.”
This sort of critical thinking is conspicuously absent from this (and all the other) Southampton handouts. The handout is a superb example of bait and switch: No nonsense about infant colic, innate energy or imaginary subluxations appears in it.
Acupuncture is another interesting case because there is quite a lot of research evidence, in stark contrast to the rest of traditional Chinese medicine, for which there is very little research.
|
There is a powerpoint show by Susan Woodhead (though it is labelled British Acupuncture Council). The message is simple and totally uncritical. It works. |

|
In fact there is now a broad consensus about acupuncture.
(1) Real acupuncture and sham acupuncture have been found to be indistinguishable in many trials. This is the case regardless of whether the sham is a retractable needle (or even a toothpick) in the "right" places, or whether it is real needles inserted in the "wrong" places. The latter finding shows clearly that all that stuff about meridians and flow of Qi is sheer hocus pocus. It dates from a pre-scientific age and it was wrong.
(2) A non-blind comparison of acupuncture versus no acupuncture shows an advantage for acupuncture. But the advantage is usually too small to be of any clinical significance. In all probability it is a placebo effect -it’s hard to imagine a more theatrical event than having someone in a white coat stick long needles into you, like a voodoo doll. Sadly, the placebo effect isn’t big enough to be of much use.
Needless to say, none of this is conveyed to the medical students of Southampton. Instead they are shown crude ancient ideas that date from long before anything was known about physiology as though they were actually true. These folks truly live in some alternative universe. Here are some samples from the acupuncture powerpoint show by Susan Woodhead.
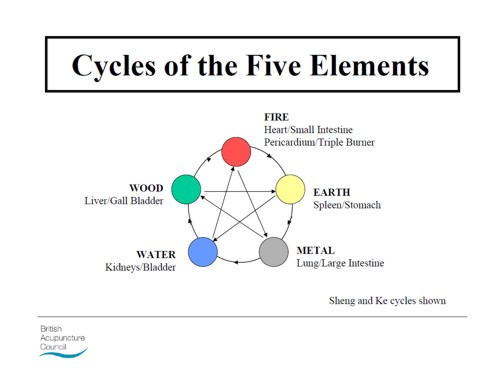


Well this is certainly a "different diagnostic language", but no attempt is made to say which one is right. In the mind of the acupuncurist it seems both are true. It is a characteristic of alternative medicine advocates that they have no difficulty in believing simultaneously several mutually contradictory propositions.
As a final exmple of barminess, just look at the acupuncture points (allegedly) on the ear The fact that it is a favoured by some people in the Pentagon as battlefield acupuncture, is more reminiscent of the mad general, Jack D. Ripper, in Dr Strangelove than it is of science.
There is an equally uncritical handout on acupuncture by Val Hopwood. It’s dated March 2003, a time before some of the most valuable experiments were done.
The handout says "sham acupuncture
is generally less effective than true acupuncture", precisely the opposite of what’s known now. And there are some bits that give you a good laugh, always helpful in teaching. I like
“There is little doubt that an intact functioning nervous system is required for acupuncture to produce
analgesia or, for that matter, any physiological changes”
and
Modern techniques: These include hybrid techniques such as electro-acupuncture . . . and Ryadoraku [sic] therapy and Vega testing.
Vega testing!! That’s been disproved dozens of times (not least by George Lewith). And actually the other made-up nonsense is spelled Ryodoraku.
It’s true that there is a short paragraph at the end of the handout headed "Scientific evaluation of acupuncture" but it doesn’t cite a single reference and reads more like excuses for why acupuncture so often fails when it’s tested properly.
Homeopathy. Finally a bit about that most boring of topics, the laughable medicine that contains no medicine, homeopathy. Caroline Eyles is a member for the Society of Homeopaths, the organisation that did nothing when its members were caught out in the murderous practice of recommending homeopathy for prevention of malaria. The Society of Homeopaths also endorses Jeremy Sherr, a man so crazy that he believes he can cure AIDS and malaria with sugar pills.
The homeopathy handout given to the students has 367 references, but somehow manages to omit the references to their own boss’s work showing that the pills are placebos. The handout has all the sciencey-sounding words, abused by people who don’t understand them.
"The remedy will be particularly effective if matched to the specific/particular characteristics of the individual (the ‘totality’ of the patient) on all levels, including the emotional and mental levels, as well as just the physical symptoms. ‘Resonance’ with the remedy’s curative power will then be at it’s [sic] best."
The handout is totally misleading about the current state of research. It says
"increasing clinical research confirms it’s [sic] clinical effectiveness in treating patients, including babies and animals (where a placebo effect would be hard to justify)."
|
The powerpont show by Caroline Eyles shows all the insight of a mediaeval vitalist |
|
Anyone who has to rely on the utterly discredited Jacques Benveniste as evidence is clearly clutching at straws. What’s more interesting about this slide the admission that "reproducibility is a problem -oops, an issue" and that RCTs (done largely by homeopaths of course) have "various methodological flaws and poor external validity". You’d think that if that was the best that could be produced after 200 yours, they’d shut up shop and get another job. But, like aging vicars who long since stopped believing in god, but are damned if they’ll give up the nice country rectory, they struggle on, sounding increasingly desperate.
How have topics like this become so embedded in a medical course at a Russell group university?
The details above are a bit tedious and repetitive. It’s already established that hardly any alternative medicine works. Don’t take my word for it. Check the web site of the US National Center for Complementary and Alternative Medicine (NCCAM) who, at a cost of over $2 billion have produced nothing useful.
A rather more interesting question is how a good university like Southampton comes to be exposing its medical students to teaching like this. There must be some powerful allies higher up in the university. In this case it’s pretty obvious who thay are.
Professor Stephen Holgate MD DSc CSc FRCP FRCPath FIBiol FBMS FMed Sci CBE has to be the primary suspect, He’s listed as one of Southampton’s Outstanding Academics. His work is nothing to do with alternative medicine but he’s been a long term supporter of the late unlamented Prince of Wales’ Foundation, and he’s now on the advisory board of it’s successor, the so called "College of Medicine" (for more information about that place see the new “College of Medicine” arising from the ashes of the Prince’s Foundation for Integrated Health, and also Don’t be deceived. The new “College of Medicine” is a fraud and delusion ). His description on that site reads thus.
"Stephen Holgate is MRC Clinical Professor of Immunopharmacology at the University of Southampton School of Medicine and Honorary Consultant Physician at Southampton University Hospital Trust. He is also chair of the MRC’s Populations and Systems Medicine Board. Specialising in respiratory medicine, he is the author of over 800 peer-reviewed papers and contributions to scientific journals and editor of major textbooks on asthma and rhinitis. He is Co-Editor of Clinical and Experimental Allergy, Associate Editor of Clinical Science and on the editorial board of 25 other scientific journals."
Clearly a busy man. Personally I’m deeply suspicious of anyone who claims to be the author of over 800 papers. He graduated in medicine in 1971, so that is an average of over 20 papers a year since then, one every two or three weeks. I’d have trouble reading that many, never mind writing them.
Holgate’s long-standing interest in alternative medicine is baffling. He’s published on the topic with George Lewith, who, incidentally, is one of the directors of the "College of Medicine"..
It may be unkind to mention that, for many years now, I’ve been hearing rumours that Holgate is suffering from an unusually bad case of Knight starvation.
The Division of Medical Education appears to be the other big source of support for. anti-scientific medicine. That is very odd, I know, but it was also the medical education people who were responsible for mis-educating medical students at. St. Bartholomew’s and at Edinburgh university. Southampton’s Division of Medical Education has a mind-boggling 60 academic and support staff. Two of them are of particular interest here.
Faith Hill is director of the division. Her profile doesn’t say anything about alternative medicine, but her interest is clear from a 2003 paper, Complementary and alternative medicine: the next generation of health promotion?. The research consisted of reporting anecdotes from interviews of 52 unnamed people (this sort of thing seems to pass for research in the social sciences). It starts badly by misrepresenting the conclusions of the House of Lords report (2000) on CAM. Although it comes to no useful conclusions, it certainly shows a high tolerance of nonsensical treatments.
Chris Stephens is Associate Dean of Medical Education & Student Experience. His sympathy is shown by a paper he wrote In 2001, with David Owen (the homeopath, above) and George Lewith: Can doctors respond to patients’ increasing interest in complementary and alternative medicine?. Two of the conclusions of this paper were as follows.
"Doctors are training in complementary and alternative medicine and report benefits both for their patients and themselves"
Well, no actually. It wasn’t true then, and it’s probably even less true now. There’s now a lot more evidence and most of it shows alternative medicine doesn’t work.
"Doctors need to address training in and practice of complementary and alternative medicine within their own organisations"
Yes they certainly need to do that.
And the first thing that Drs Hill and Stephens should do is look a bit more closely about what’s taught in their own university, I hope that this post helps them,
Follow-up
4 July 2011. A correspondent has just pointed out that Chris Stephens is a member of the General Chiropractic Council. The GCC is a truly pathetic pseudo-regulator. In the wake of the Simon Singh affair it has been kept busy fending off well-justified complaints against untrue claims made by chiropractors. The GCC is a sad joke, but it’s even sadder to see a Dean of Medical Education at the University of Southampton being involved with an organisation that has treated little matters of truth with such disdain.
A rather unkind tweet from (ex)-chiropractor @RichardLanigan.
“Chris is just another light weight academic who likes being on committees. Regulatory bodies are full of them”
The Atlantic is an American magazine founded (as The Atlantic Monthly) in Boston, Massachusetts, in 1857. It is a literary and cultural magazine with a very distinguished history. Its contributors include Mark Twain and Martin Luther King. So it was pretty exciting to be asked to write something for it, even with a 12 hour deadline.

Sadly though, in recent years, the coverage of science in The Atlantic has been less than good The inimitable David Gorski has explained the problem in Blatant pro-alternative medicine propaganda in The Atlantic. The immediate cause of the kerfuffle was the publication of an article, The Triumph of New-Age Medicine. It was written by a journalist, David Freedman. It is very long and really not very good. It has been deconstructed also by Steven Novella.
Freedman’s article is very long, but it boils down to saying I know it doesn’t work but isn’t it nice. The article was followed up with Fix or Fraud: a ‘debate’., The debate is rather disappointing. It suffers from the problem, not unknown at the BBC, of thinking that ‘balance’ means giving equal time to people who think the earth is flat as it gives to people who think it is a oblate spheroid. The debate consists of 800 word contributions from seven people, six of whom are flat earthers, and one of which is very good. Try Steven Salzberg, A ‘triumph’ of hype over reality for some real sense. One of the flat earthers is director of a National Institutes of Health institute, NCCAM.
And this is a magazine that published not only Mark Twain, but Abraham Flexner, the man who, in 1910, put US medical education on a firm scientific footing, You can read Flexner in their archive. Mark Twain said
[A reply to letters recommending remedies]:
Dear Sir (or Madam):–I try every remedy sent to me. I am now on No. 67. Yours is 2,653. I am looking forward to its beneficial results. – quoted in My Father Mark Twain, by Clara Clemens
"allopathy is good for the sane and homeopathy for the insane"
So here is the piece, produced rather rapidly, for the debate. This is the original unedited version, slightly longer than appears in The Atlantic.
The title for The Atlantic piece, America, Land of the Health Hucksters, was theirs not mine. There is no shortage of health hucksters in the UK. but at least they mostly haven’t become as embedded within univerities and hospitals as much as in the USA.
|
David Freeman’s article, “The Triumph of New Age Medicine” starts by admitting that most alternative treatments don’t work, and ends by recommending them. He takes a lot more words to say it, but that seems a fair synopsis. It is the sort of thing you might expect in a cheap supermarket magazine, not in Atlantic. The article is a prime example of rather effective sales technique, much beloved of used car salesmen and health hucksters. It’s called bait and switch. It’s true that medicine can’t cure everything. That’s hardly surprising given that serious research has been going on for barely 100 years, and it turns out that the humans are quite complicated. But the answer to the limitations of medicine is not to invent fairy stories, which is what the alternative medicine industry does. There is no sensible option but to keep the research going and to test its results honestly. It’s sad but true that Big Pharma has at times corrupted medicine, by concealing negative results. But that corruption has been revealed by real scientists, not by health hucksters. In the end, science is self-correcting and the truth emerges. Health hucksters, on the other hand, seem incapable of giving up their beliefs whatever the evidence says. The idea of patient-centered care is fashionable and care is great, if you can’t cure. But there’s a whole spectrum in the wellbeing industry, from serious attempts to make people happier, to the downright nuts. The problem is that caring for patients make a very good bait, and the switch to woo tends to follow not far behind. I write from the perspective of someone who lives in a country that achieves health care for all its citizens at half the cost of the US system, and gets better outcomes in life expectancy and infant mortality. The view from outside is that US medicine rather resembles US religion. It has been taken over by fundamentalists who become very rich by persuading a gullible public to believe things that aren’t true. One of Freedman’s problems is, I think, that he vastly overestimates the power of the placebo effect. It exists, for sure, but in most cases, it seems to be small, erratic and transient. Acupuncture is a good example. It’s quite clear now that real acupuncture and sham acupuncture are indistinguishable, so it’s also quite clear that the ‘principles’ on which it’s based are simply hokum. If you do a non-blind comparison of acupuncture with no acupuncture, there is in some trials (not all) a small advantage for the acupuncture group. But it is too small to be of much benefit to the patient. By far the more important reason why ineffective voodoo like acupuncture appears to work is the “get better anyway” effect (known technically as regression to the mean). You take the needles or pills when you are at your worst, the next day you feel better. It’s natural to attribute the fact that you feel better to the needles or pills, when all you are seeing is natural fluctuations in the condition. It’s like Echinacea will cure your cold in only seven days when otherwise it would have taken a week. If the article itself was naïve and uncritical, the follow up was worse. It is rather surprising to me that a magazine like Atlantic should think it worth printing an advertorial for Andrew Weil’s business. Surely, though, Josephine Briggs, as director of an NIH institute is more serious? Sadly, no. Her piece is a masterpiece of clutching at straws. The fact is that her institute has spent over $ 2 billion of US taxpayers’ money and, for all that money it has produced not a single useful treatment. All that NCCAM has done is to show that several things do not work, something we pretty much knew already. If I were a US taxpayer, I’d be somewhat displeased by that. It should be shut down now. At first sight Dean Ornish sounds more respectable. He bases his arguments on diet and life style changes, which aren’t alternative at all. He’s done some research too. The problem is that it’s mostly preliminary and inconclusive research, on the basis of which he vastly exaggerates the strength of the evidence for what can be achieved by diet alone. It’s classical bait and switch again. The respectable, if ill-founded, arguments get you the foot in the door, and the woo follows later. This is all very sad for a country that realized quite early that the interests of patients were best served by using treatments that had been shown to work. The Flexner report of 1910 led the world in the rational education of physicians. But now even places like Yale and Harvard peddle snake oil to their students through their "integrative medicine" departments. It’s hard to see why the USA is in the vanguard of substituting wishful thinking for common sense and reason. The main reason, I’d guess, is money. Through NCCAM and the Bravewell Collaborative, large amounts of money have been thrown to the winds and businesses like Yale and Harvard have been quick to abandon their principles and grab the money. Another reason for the popularity of alternative medicine in parts of academia is that it’s a great deal easier to do ‘science’ when you are allowed to make up the answers. The "integrative medicine" symposium held at Yale in 2008 boggled the mind. Dr David Katz listed a lot of things he’d tried and which failed to work, His conclusion was not that they should be abandoned, but that we needed a "more fluid concept of evidence". You can see it on YouTube, Senator Tom Harkin’s promotion of NCCAM has done for the U.S. reputation in medicine what Dick Cheney did for the U.S. reputation in torture. It is hard to look at the USA from outside without thinking of the decline and fall of the Roman Empire. One had hoped that era was over with the election of Obama, but the hucksters won’t give up without a fight. They are making too much money to do that. |
Follow-up
The comments that appeared in The Atlantic on this piece were mostly less than enlightening -not quite what one expected of an intellectual magazine. Nevertheless I tried to answer all but the plain abusive comments.
More interesting, though, was an editorial by Jennie Rothenberg Gritz, the Atlantic Senior Editor who asked me to contribute. The Man Who Invented Medical School. It picked up on my mention of Abraham Flexner, and his famous 1910 report [download from Carnegie Foundation] which first put US medial education on a form rational footing. based on science. Now, 100 years later that’s being unpicked both in the USA and here. ms Gritz seemed to think that Flexner would have approved of Dean Ornish. In a response I begged to differ. I’m pretty sure that Felxner would have been furious of he could have seen the reecent march of quackademia, particularly, but not exclusively, in the USA. It is exactly the sort of thing his report set out, successfully, to abolish. He wrote, for example,
“the practitioner is subjected, year in, year out, to the steady bombardment of the unscrupulous manufacturer, persuasive to the uncritical, on the principle that “what I tell you three times is true.” Against bad example and persistent asseveration, only precise scientific concepts and a critical
appreciation of the nature and limits of actual demonstration can protect the young physician.” (Flexner report, 1910, pp 64-65)
It is this very “appreciation of the nature and limits of actual demonstration” that is now being abandoned by the alternative medicine industry. despite the fact that real medicine was in its infancy at the time he w as writing, he was very perceptive about the problems. Perhaps Freedman should read the report.
David Katz seems to have spotted my piece in The Atlantic, and has responded at great length in the Huffington Post (quite appropriate, given the consistent support of HuffPo for nonsense medicine). HuffPo allows only short comments with no links so I’ll reply to him here.
I fear that Dr Katz doth protest a great deal too much. He seems to object to a comment that I made about him in The Atlantic.
“… [He] listed a lot of things he’d tried and which failed to work. His conclusion was not that they should be abandoned, but that we needed a ‘a more fluid concept of evidence.'”
You don’t have to take my word for it. You can take it from the words of Dr Katz.
"What do we do when the evidence we have learned, or if we care to be more provocative, with which we have been indoctrinated, does now fully meet the needs of our patients"
It seems odd to me to regard teaching about how you distinguish what;s true and what isn’t as "indoctrination", though I can understand that knowledge of that subject could well diminish the income of alternative practitioners. You went on to say
"Some years ago the CDC funded us with a million dollars to do what they referred to initially as a systematic review of the evidence base for complementary and alternative medicine, Anybody who’s ever been involved in systematic reviews knows that’s a very silly thing. . . . Well we knew it was silly but a million dollars sounded real [mumbled] took the money and then we figurered we’d figure out what to do with it [smiles broadly]. That’s what we did ". . .
I do hope you told the CDC that you did not spend the million dollars for the sensible purpose for which it was awarded.
This infusion of calcium, magnesium and D vitamins and vitamin C ameliorates the symptoms of fibromyalgia. . . . We did typical placebo controlled randomized double-blind trial for several months . . . we saw an improvement in both our treatment and placebo groups . . .
You then describe how you tested yoga for asthma and homeopathy for attention deficit hyperactivity disorder, Neither of them worked either. Your reaction to this string of failures was just to say “we need a more fluid concept of evidence”
After telling an anecdote about one patient who got better after taking homeopathic treatment you said £I don’t care to get into a discussion of how, or even whether, homeopathy works”. Why not? It seems it doesn’t matter much to you whether the things you sell to patients work or not.
You then went on to describe quite accurately that anti-oxidants don’t work and neither do multivitamin supplements for prevention of cardiovascular problems, And once again you fail to accept the evidence, even evidence you have found yourself. Your response was
“So here too is an invitation to think more fluidly about of evidence. Absence of evidence is not evidence of absence.”
That last statement is the eternal cry of every quack. It’s true, of course, but that does not mean that absence of evidence gives you a licence to invent the answer. But inventing the answer is what you do, time after time, You seem quite incapable of saying the most important thing that anyone in your position should. I don’t know the answer.
Universities, like most businesses, cite glowing testimonials from grateful students, I doubt whether universities are any more honest than anyone else in their choice of what to publish. When I asked to see any letters that had been sent to the university, I was sent only one and extracts from it appear in the last post on Westminster. More dangerous nonsense from the University of Westminster: when will Professor Geoffrey Petts do something about it? But I knew (don’t ask how) that there had been more than that, and a slightly widened FOIA request produced some interesting results (though I’m aware of other letters that were not supplied -not good).
As always, the information came with the caveat
"Copyright in our response to your request belongs to the University of Westminster. All rights are reserved. This document is for personal use only and may not be copied, or stored in any electronic form, or reproduced in any other way or used for any other purpose, either in whole or in part, without the prior written consent of the University of Westminster.".
Why else would anyone ask for information but to make it public? And since the letter was sent in electronic form, it would be hard to comply with the second part. As always, I rely on the fair quotation and public interest defences to quote parts of the letters.
The main players here are Peter Davies (Head of herbal medicine and nutritional therapy), Julie Whitehouse (Course Leader for MSci Herbal Medicine and the BSc Honours Health Sciences), David Peters (Clinical director of Westminster’s School of Integrated Health), and the dean of the School of Life Sciences. Jane Lewis. There’s no woo about Jane Lewis. I suspect she’d have got rid of all the nonsense, given a chance. Who, I wonder, is stopping her?
Julie Whitehouse is, I see, a co-author of Brock et al. (2010) American skullcap (Scutellaria lateriflora): an ancient remedy for today’s anxiety, British Journal of Wellbeing1 (4), 25-30. I had no idea there was such a journal. UCL does not subscribe so if anyone has a reprint I’d love to see it. Judging by the abstract it’s yet more ‘preliminary work’. That’s very typical. Next to no CAM research gets past the preliminary report.
Some testimonials
Here are some quotations from “a part-time student on the herbal medicine (HM) BSc course, currently in my 3rd year of study. I have first class honours degree in ecology, am a qualified staff nurse, and am an experienced performance and business manager."
|
cc Professor Jane Lewis, Dean of School: Biosciences "Dear Professor Petts, I hope you do not mind me writing to you personally. I am a part-time student on the herbal medicine (HM) BSc course, currently in my 3rd year of study. I have first class honours degree in ecology, am a qualified staff nurse, and am an experienced performance and business manager. I regard myself as scientist." "I would like to express to you my disappointment and frustration with my own studies at Westminster. I thought (erroneously, I have since discovered) that I was paying for a Bachelor of Science degree, and that science and scientific thinking would underpin my studies. How wrong I have been. Based on my experience at Westminster, two things really need to be done to restore credibility in the herbal medicine degree, viz. removing the antiscience and pseudoscience, and strengthening the scientific basis of both our core and herbal medicine modules. The current degree is confusing and infuriating in that it really does not know what it is." "Here is a quote from a handout (on ‘The Galenic Constitutional System in Practice’) given to 3rd year herbalists last semester: ‘Treating particular disease/conditions is more successful if the disease can be analysed in terms on hot, cold, wet and dry’. If I showed this to any modern (not 17th century) doctor they would be rolling around on the floor in hysterics and condemning this type of nonsense in the strongest possible language. I am ashamed to tell anybody what we are being taught. Is this clandestine teaching or is the University actually sanctioning this pre-scientific view of medicine?" Anti-science ideas need to be, not only banished from teaching material, but also robustly challenged every time they are raised by students (or lecturers) in the polyclinic or the classroom. But, constantly challenging anti-scientific and erroneous ideas is very wearing and wearying for me as a student, as I am sure it is for scientists on your staff. (I should say here that there are some excellent scientists who have supported and encouraged me in my studies at Westminster; Dr Gillian Shine in the core modules and Christopher Robbins in HM, leap to mind). academic institution. I should not feel threatened by challenging what I am taught when it is plainly pseudoscience or antiscience and my University should be supporting me in my challenge, which I am sure you will. |
And from the same student, this time addressed to Julie Whitehouse and copied to the dean, Jane Lewis (in 2009) [some details removed to preserve patient confidentiality].
|
… a patient attended who had been treated with a Reiki [typo for Reishi] mushroom tincture and another herbal tincture (about 6 herbs) by an HM clinic supervisor. The patient had also been advised to do ‘body brushing’ which I understand was for ‘detoxification’. This lady is being treated by an oncologist for [***] cancer and is currently undergoing chemotherapy. I do not believe her oncology team were informed before we initiated treatment and the bottles of tincture were not labelled with what they contained. I have serious ethical problems with treating anyone with cancer with herbs, but someone in the middle of chemotherapy? Not only are patients’ lives being put at risk, but students are not getting clear messages about the limitations of HM or the professional ethics involved in treating someone with cancer. I have seen patient files with ‘anti-mitotic’ or ‘anti-cancer’ herbs written in the notes. I question whether this is also bordering on the illegal. At the very least it betrays a naive belief that herbs can treat cancer. I was ignored earlier this year when I queried students being encouraged to go to a herbalist’s cancer seminars in Bristol (and she claimed to cure cancer) and this case highlights to me the dangers of Wmin condoning and teaching the ‘we treat people not diseases’ mantra. |
This second letter elicited a response from the university, and the response is worth looking at.
The response
|
2 What was done following the complaint 021209 Clinical Director met with the tutor. Reviewed notes. No indication that the patient was seeking ‘alternatives’ to chemo, nor that she was led to believe the prescription was designed to do other than support her coping with chemo which in her experience had previously been physically demanding and distressing. Procedures regarding communication with oncologists, informed consent, labeling of medicines need reviewing and reinforcing. Action by Course leader/herbal team. Report back to PC Exec 210110 151209 The student who (though she had not been present during this session, had objected to way this case was handled met with the course leader in the presence of the Senior Clinical supervisor and another tutor. The meeting was supportive rather than confrontational. The student was asked to reflect on the consequences of her (frequent) impulsive emailing and the time and effort she demands of others – and to consider the Code of Conduct she has signed. |
So the whistle-blowing student seems to have been patted on the head and told to shut up. Nevertheless the complaint had some effect, though not much.
|
050110 Course leader proposed to review current Polyclinic policies and procedures, and discuss current practice in cases of serious disease and how doctors are informed and patients consented
|
The response included "Extracts from Smith J, Rowan N & Sullivan (2000) Medicinal Mushrooms: Their therapeutic properties and current medical usage with special emphasis on cancer treatment” from Cancer Research UK."
|
In almost all the examples that will be discussed in this chapter the polysaccharides act mainly as immune- stimulants with little or no adverse drug reactions. Furthermore, several of these extracts have been shown to stimulate apoptosis in cancer cells (e.g. Fullerton et al., 2000). While there are examples where the mushroom polysaccharides have shown efficacy against specific types of cancer as monotherapy, the overwhelming successes have been demonstrated when they function together with proven and accepted chemotherapeutic agents.
|
I could not find that document at Cancer Research UK though there is a similar report, dated May 2002, "Medicinal Mushrooms: Their therapeutic properties and current medical usage with special emphasis on cancer treatments" by Smith, Rowan and Sullivan. It can be downloaded at the Cancer Research UK page, Medicinal Mushrooms and Cancer. That page, last updated 7 August 2006, lists John Smith BSc MSc PhD DSc FIBiol FRSE as Emeritus Professor of Applied Microbiology, University of Strathclyde. amd Chief Scientific Officer, MycoBiotech Ltd, Singapore, and Richard Sullivan BSc MD PhD as Head of Clinical Programmes, Cancer Research UK (a job he left in 2008). Professor John Smith is still Chief Scientific Advisor to Mycobiotech Inc, based in Singapore. This company sells various mushroom products. They are all marketed as “nutriceuticals” or “functional foods”, not as pharmaceuticals. These descriptions are a very common way of making medicinal claims for products, while describing them as foods to avoid the strict regulations about claims made for medicines.
It does not seem to me to be a good idea for Cancer Research UK to have advice on its web site from someone with a very obvious financial interest.
The quotations from the Smith report are obviously intended to defend the practice of prescribing mushrooms to people on chemotherapy. But the fact that in 2011, five years after the CRUK page, Mycobiotech still has no approved medicine approved for cancer speaks for itself. They sell Shiitake Herbal Soups. They also sell Essence of Shiitake which, they say, contains Lentinan, “which has been confirmed through research, to be an immuno-enhancer. Lentinan has been found to reduce tumour growth and to prolong the life of cancer patients”. That sounds to me like a rather strong medicinal claim for a “food”. Even Nutra-ingredients, the industry site for nutriceuticals, doesn’t claim much for it.
Now back to Westminster’s response to the student’s complaint.
|
I have found no evidence that herbal practitioners in the Polyclinic are making explicit claims to treat cancer. |
And, from David Peters.
|
DP**There is one item in the notes however which I think we need to comment on. While the paper-trail in all other respects shows that the herbal prescription was supportive, one herb in the prescription is categorised as ‘anti-tumour’. Although I am convinced after reviewing the notes and talking with the tutor involved, that the aim was to support the patient through her chemotherapy, this part of the prescription nonetheless signifies some ambivalence at least, about whether the aim was or was not to treat cancer
|
But then, from Julie Whitehouse
|
JW Yes there is antitumour as an action for many herbs and nutritional components – and several relevant actions including anything as general as anti- oxidant even – it doesn’t mean we are suggesting they are being used as treatment
|
It doesn’t take much reading between the lines to see the tension between Whitehouse and Peters. The former is very reluctant to give up the myths, the latter is slightly more cautious about claims to treat cancer.
Let’s be clear about one thing. The student was dead right. There is so little reliable information about mushrooms that neither Cochrane Reviews nor NCCAM has anything relevant to say about them. Antioxidants are a myth, much beloved by marketing people and "boosting the immune system" is the universal mantra of every advocate of magic medicine when they can’t think of anything else to make up. Why can’t Peters and Whitehouse admit it?
More complaints
This one is from a member of staff who teaches on the herbal medicine course. It was addressed to Julie Whitehouse and copied to the dean and vice-chancellor.(10 July 2009).
|
"During last week (5-9th May) I witnessed a member of the Herbal Team and a student dowsing with a pendulum to divine herbal drugs to prescribe for the student. When I approached and spoke, they defensively hid the pendulum and were clearly embarrassed. I discussed what they were doing. They freely said they were prescribing herbal medicine and cited other staff as their ‘authority’ and ‘instructors’. Diagnosing or prescribing by pendulum has no scientific credibility. Further, it is dangerous for prescribing as it both fails to identify any appropriate drugs (except by chance) and may select dangerous drugs for a patient. I know other staff have raised with you the teaching or use of such mediaeval and unscientific practices on the Wmin HM course." "I feel that such practice in the HM Course teaching or in the Polyclinic should be proscribed. I would like to suggest that you address and resolve this matter urgently. Dowsing is in conflict with the VC’s recent letter to SIH staff, specifically expecting more evidence of science within the teaching of CT Courses." "I expect that were the Department of Health to be aware of the unscientific teaching and promotion of practices like dowsing, (and crystals, iridology, astrology, and tasting to determine pharmacological qualities of plant extracts) on the Wmin HM Course, progress towards the Statutory Regulation of Herbal Medicine could be threatened." |
The writer seems to have overestimated the sense in the Department of Health. They were aware of these practices (I told them) but nevertheless went ahead with a silly form of statutory regulation.
The same lecturer wrote on 27 July 2009
|
"This happened with a supervisor, students and patient in the consultation room. The patient was invited to dowse her own "remedies" using a pendulum. A set of Bach Flower remedies (also proscribed in the HM Clinics) was placed in front of the patient and a pendulum was produced. On the basis of the dowsing, a prescription of ‘remedies’ was dispensed." "Although Julie says dowsing has been proscribed, she has been unable to present and document saying as such. Bach Flower Remedies have been proscribed for HM Clinics." |
Some of the replies were sent to me. Julie Whitehouse replied to the lecturer and Peter Davies on 10 August 2009
|
“I have written and circulated the text to be put into the handbook and have had approval from most members of the herbal team – but [the lecturer who complained] was not there at the time – hope he approves of the statement. It does not specifically say we do not dowse – but it does I think state clearly what we do – we surely do not want a list of what we don’t do – where would it end – there could be many things in a list of what we don’t do.”
|
So she explicitly refused to ban the use of dowsing in Westminster’s clinic. The lecturer replied, pointing out the unreasonableness of this attitude.
|
Dear Julie, I am afraid that I have not received any copy (home or University) of your ‘statement’ so cannot comment. Please resend me another copy. I don’t understand your not wanting ‘a list of what we don’t do – where would it end’. It is commonplace to have proscribed activities in both social and professional activities, and these are usually for clear reasons of safety and public good. Eg.: Herbal practice is constrained by the prohibitions in the Medicines Act 1968 and following, the maximum dosages under Schedule III of that Act, the prohibited herbal drugs under the MCA, Trading Standards regulations, etc. |
It seems that, despite the vice-chancellor’s assurance that the courses would become more scientific, there are still apologists for diagnosis with a pendulum, and for treating cancer with mushrooms at Westminster University.
This saga sounds only top characteristic. Complaints through official channels usually get you nowhere with big organisations. Sadly, the only way to get change is public embarrassment.
Some action from Vice-chancellor Geoftrey Petts is long overdue.
Follow-up
A kind reader sent me a copy of Brock, Whitehouse, Tewfik & Towell,. (2010) American skullcap (Scutellaria lateriflora): an ancient remedy for today’s anxiety, British Journal of Wellbeing1 (4), 25-30.. This is the paper that I described above, on the basis of the abstract, as "preliminary study".. Now that I’ve seen it I realise it isn’t study at all. They simply emailed 377 members of the National Institute of Medical Herbalists to ask what they thought of S. laterifloria. Only 62 replied (16%) and their anecdotes are listed in the paper. It is this sort of worthless information that gets herbal medicine a bad name.
10 August 2011. I notice that Professor Petts has replied to a letters sent to him by the Nightingale Collaboration. He said “Whilst I understand your concerns, colleagues of the School of Life Sciences where these courses are offered do not share them. They are not teaching pseudo-science, as you claim,…”. Well I know at least two member of the Life Sciences department who are very worried. One has now left and one has retired. The rest are presumably too scared to speak out. How he has the nerve to claim that they don’t teach pseudo-science all the teaching materials that have been revealed on this blog is hard to imagine. It is simply not true and he must know it. I find it deeply worrying when vice-chancellors say things which they know to be untrue.
The latest example to come to light is cited by Andy Lewis on his Quackometer blog
“There are some even odder characters too, such as Roy Riggs B.Sc who descibes himself as a “Holistic Geobiologist” and is “an “professional Earth Energy dowser”. He guest lectures at the London Westminster University’s School of Integrative Medicine and The Baltic Dowser’s Association of Lithuania.”
I do wonder who Professor Petts thinks he’s fooling.
One wonders about the standards of peer review at the British Journal of General Practice. The June issue has a paper, "Acupuncture for ‘frequent attenders’ with medically unexplained symptoms: a randomised controlled trial (CACTUS study)". It has lots of numbers, but the result is very easy to see. Just look at their Figure.
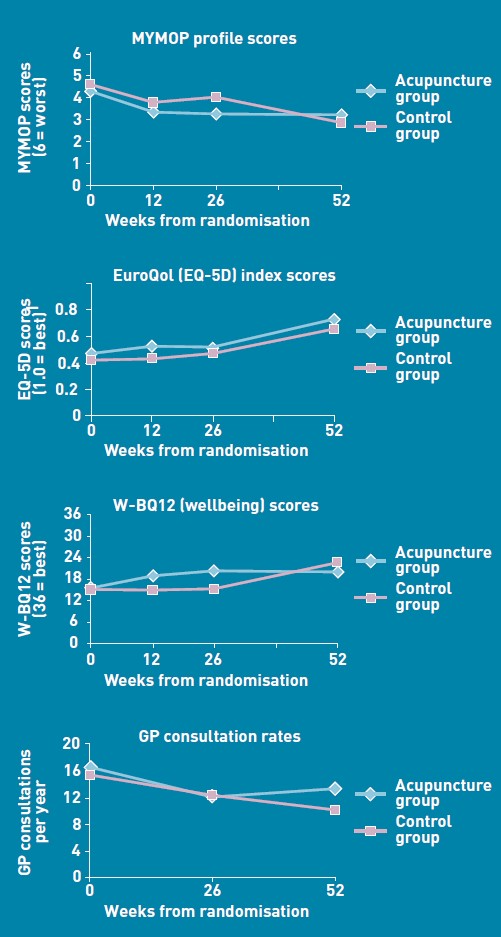
There is no need to wade through all the statistics; it’s perfectly obvious at a glance that acupuncture has at best a tiny and erratic effect on any of the outcomes that were measured.
But this is not what the paper said. On the contrary, the conclusions of the paper said
|
Conclusion The addition of 12 sessions of five-element acupuncture to usual care resulted in improved health status and wellbeing that was sustained for 12 months. |
How on earth did the authors manage to reach a conclusion like that?
The first thing to note is that many of the authors are people who make their living largely from sticking needles in people, or advocating alternative medicine. The authors are Charlotte Paterson, Rod S Taylor, Peter Griffiths, Nicky Britten, Sue Rugg, Jackie Bridges, Bruce McCallum and Gerad Kite, on behalf of the CACTUS study team. The senior author, Gerad Kite MAc , is principal of the London Institute of Five-Element Acupuncture London. The first author, Charlotte Paterson, is a well known advocate of acupuncture. as is Nicky Britten.
The conflicts of interest are obvious, but nonetheless one should welcome a “randomised controlled trial” done by advocates of alternative medicine. In fact the results shown in the Figure are both interesting and useful. They show that acupuncture does not even produce any substantial placebo effect. It’s the authors’ conclusions that are bizarre and partisan. Peer review is indeed a broken process.
That’s really all that needs to be said, but for nerds, here are some more details.
How was the trial done?
The description "randomised" is fair enough, but there were no proper controls and the trial was not blinded. It was what has come to be called a "pragmatic" trial, which means a trial done without proper controls. They are, of course, much loved by alternative therapists because their therapies usually fail in proper trials. It’s much easier to get an (apparently) positive result if you omit the controls. But the fascinating thing about this study is that, despite the deficiencies in design, the result is essentially negative.
The authors themselves spell out the problems.
“Group allocation was known by trial researchers, practitioners, and patients”
So everybody (apart from the statistician) knew what treatment a patient was getting. This is an arrangement that is guaranteed to maximise bias and placebo effects.
"Patients were randomised on a 1:1 basis to receive 12 sessions of acupuncture starting immediately (acupuncture group) or starting in 6 months’ time (control group), with both groups continuing to receive usual care."
So it is impossible to compare acupuncture and control groups at 12 months, contrary to what’s stated in Conclusions.
"Twelve sessions, on average 60 minutes in length, were provided over a 6-month period at approximately weekly, then fortnightly and monthly intervals"
That sounds like a pretty expensive way of getting next to no effect.
"All aspects of treatment, including discussion and advice, were individualised as per normal five-element acupuncture practice. In this approach, the acupuncturist takes an in-depth account of the patient’s current symptoms and medical history, as well as general health and lifestyle issues. The patient’s condition is explained in terms of an imbalance in one of the five elements, which then causes an imbalance in the whole person. Based on this elemental diagnosis, appropriate points are used to rebalance this element and address not only the presenting conditions, but the person as a whole".
Does this mean that the patients were told a lot of mumbo jumbo about “five elements” (fire earth, metal, water, wood)? If so, anyone with any sense would probably have run a mile from the trial.
"Hypotheses directed at the effect of the needling component of acupuncture consultations require sham-acupuncture controls which while appropriate for formulaic needling for single well-defined conditions, have been shown to be problematic when dealing with multiple or complex conditions, because they interfere with the participative patient–therapist interaction on which the individualised treatment plan is developed. 37–39 Pragmatic trials, on the other hand, are appropriate for testing hypotheses that are directed at the effect of the complex intervention as a whole, while providing no information about the relative effect of different components."
Put simply that means: we don’t use sham acupuncture controls so we can’t distinguish an effect of the needles from placebo effects, or get-better-anyway effects.
"Strengths and limitations: The ‘black box’ study design precludes assigning the benefits of this complex intervention to any one component of the acupuncture consultations, such as the needling or the amount of time spent with a healthcare professional."
"This design was chosen because, without a promise of accessing the acupuncture treatment, major practical and ethical problems with recruitment and retention of participants were anticipated. This is because these patients have very poor self-reported health (Table 3), have not been helped by conventional treatment, and are particularly desperate for alternative treatment options.".
It’s interesting that the patients were “desperate for alternative treatment”. Again it seems that every opportunity has been given to maximise non-specific placebo, and get-well-anyway effects.
There is a lot of statistical analysis and, unsurprisingly, many of the differences don’t reach statistical significance. Some do (just) but that is really quite irrelevant. Even if some of the differences are real (not a result of random variability), a glance at the figures shows that their size is trivial.
My conclusions
(1) This paper, though designed to be susceptible to almost every form of bias, shows staggeringly small effects. It is the best evidence I’ve ever seen that not only are needles ineffective, but that placebo effects, if they are there at all, are trivial in size and have no useful benefit to the patient in this case..
(2) The fact that this paper was published with conclusions that appear to contradict directly what the data show, is as good an illustration as any I’ve seen that peer review is utterly ineffective as a method of guaranteeing quality. Of course the editor should have spotted this. It appears that quality control failed on all fronts.
Follow-up
In the first four days of this post, it got over 10,000 hits (almost 6,000 unique visitors).
Margaret McCartney has written about this too, in The British Journal of General Practice does acupuncture badly.
The Daily Mail exceeds itself in an article by Jenny Hope whch says “Millions of patients with ‘unexplained symptoms’ could benefit from acupuncture on the NHS, it is claimed”. I presume she didn’t read the paper.
The Daily Telegraph scarcely did better in Acupuncture has significant impact on mystery illnesses. The author if this, very sensibly, remains anonymous.
Many “medical information” sites churn out the press release without engaging the brain, but most of the other newspapers appear, very sensibly, to have ignored ther hyped up press release. Among the worst was Pulse, an online magazine for GPs. At least they’ve publish the comments that show their report was nonsense.
The Daily Mash has given this paper a well-deserved spoofing in Made-up medicine works on made-up illnesses.
“Professor Henry Brubaker, of the Institute for Studies, said: “To truly assess the efficacy of acupuncture a widespread double-blind test needs to be conducted over a series of years but to be honest it’s the equivalent of mapping the DNA of pixies or conducting a geological study of Narnia.” ”
There is no truth whatsoever in the rumour being spread on Twitter that I’m Professor Brubaker.
Euan Lawson, also known as Northern Doctor, has done another excellent job on the Paterson paper: BJGP and acupuncture – tabloid medical journalism. Most tellingly, he reproduces the press release from the editor of the BJGP, Professor Roger Jones DM, FRCP, FRCGP, FMedSci.
"Although there are countless reports of the benefits of acupuncture for a range of medical problems, there have been very few well-conducted, randomised controlled trials. Charlotte Paterson’s work considerably strengthens the evidence base for using acupuncture to help patients who are troubled by symptoms that we find difficult both to diagnose and to treat."
Oooh dear. The journal may have a new look, but it would be better if the editor read the papers before writing press releases. Tabloid journalism seems an appropriate description.
Andy Lewis at Quackometer, has written about this paper too, and put it into historical context. In Of the Imagination, as a Cause and as a Cure of Disorders of the Body. “In 1800, John Haygarth warned doctors how we may succumb to belief in illusory cures. Some modern doctors have still not learnt that lesson”. It’s sad that, in 2011, a medical journal should fall into a trap that was pointed out so clearly in 1800. He also points out the disgracefully inaccurate Press release issued by the Peninsula medical school.
Some tweets
Twitter info 426 clicks on http://bit.ly/mgIQ6e alone at 15.30 on 1 June (and that’s only the hits via twitter). By July 8th this had risen to 1,655 hits via Twitter, from 62 different countries,
@followthelemur Selina
MASSIVE peer review fail by the British Journal of General Practice http://bit.ly/mgIQ6e (via @david_colquhoun)
@david_colquhoun David Colquhoun
Appalling paper in Brit J Gen Practice: Acupuncturists show that acupuncture doesn’t work, but conclude the opposite http://bit.ly/mgIQ6e
Retweeted by gentley1300 and 36 others
@david_colquhoun David Colquhoun.
I deny the Twitter rumour that I’m Professor Henry Brubaker as in Daily Mash http://bit.ly/mt1xhX (just because of http://bit.ly/mgIQ6e )
@brunopichler Bruno Pichler
http://tinyurl.com/3hmvan4 Made-up medicine works on made-up illnesses (me thinks Henry Brubaker is actually @david_colquhoun)
@david_colquhoun David Colquhoun,
HEHE RT @brunopichler: http://tinyurl.com/3hmvan4 Made-up medicine works on made-up illnesses
@psweetman Pauline Sweetman
Read @david_colquhoun’s take on the recent ‘acupuncture effective for unexplained symptoms’ nonsense: bit.ly/mgIQ6e
@bodyinmind Body In Mind
RT @david_colquhoun: ‘Margaret McCartney (GP) also blogged acupuncture nonsense http://bit.ly/j6yP4j My take http://bit.ly/mgIQ6e’
@abritosa ABS
Br J Gen Practice mete a pata na poça: RT @david_colquhoun […] appalling acupuncture nonsense http://bit.ly/j6yP4j http://bit.ly/mgIQ6e
@jodiemadden Jodie Madden
amusing!RT @david_colquhoun: paper in Brit J Gen Practice shows that acupuncture doesn’t work,but conclude the opposite http://bit.ly/mgIQ6e
@kashfarooq Kash Farooq
Unbelievable: acupuncturists show that acupuncture doesn’t work, but conclude the opposite. http://j.mp/ilUALC by @david_colquhoun
@NeilOConnell Neil O’Connell
Gobsmacking spin RT @david_colquhoun: Acupuncturists show that acupuncture doesn’t work, but conclude the opposite http://bit.ly/mgIQ6e
@euan_lawson Euan Lawson (aka Northern Doctor)
Aye too right RT @david_colquhoun @iansample @BenGoldacre Guardian should cover dreadful acupuncture paper http://bit.ly/mgIQ6e
@noahWG Noah Gray
Acupuncturists show that acupuncture doesn’t work, but conclude the opposite, from @david_colquhoun: http://bit.ly/l9KHLv
8 June 2011 I drew the attention of the editor of BJGP to the many comments that have been made on this paper. He assured me that the matter would be discussed at a meeting of the editorial board of the journal. Tonight he sent me the result of this meeting.
|
Subject: BJGP Dear Prof Colquhoun We discussed your emails at yesterday’s meeting of the BJGP Editorial Board, attended by 12 Board members and the Deputy Editor The Board was unanimous in its support for the integrity of the Journal’s peer review process for the Paterson et al paper – which was accepted after revisions were made in response to two separate rounds of comments from two reviewers and myself – and could find no reason either to retract the paper or to release the reviewers’ comments Some Board members thought that the results were presented in an overly positive way; because the study raises questions about research methodology and the interpretation of data in pragmatic trials attempting to measure the effects of complex interventions, we will be commissioning a Debate and Analysis article on the topic. In the meantime we would encourage you to contribute to this debate throught the usual Journal channels Roger Jones Professor Roger Jones MA DM FRCP FRCGP FMedSci FHEA FRSA |
It is one thing to make a mistake, It is quite another thing to refuse to admit it. This reply seems to me to be quite disgraceful.
20 July 2011. The proper version of the story got wider publicity when Margaret McCartney wrote about it in the BMJ. The first rapid response to this article was a lengthy denial by the authors of the obvious conclusion to be drawn from the paper. They merely dig themselves deeper into a hole. The second response was much shorter (and more accurate).
|
Thank you Dr McCartney Richard Watson, General Practitioner The fact that none of the authors of the paper or the editor of BJGP have bothered to try and defend themselves speaks volumes. Like many people I glanced at the report before throwing it away with an incredulous guffaw. You bothered to look into it and refute it – in a real journal. That last comment shows part of the problem with them publishing, and promoting, such drivel. It makes you wonder whether anything they publish is any good, and that should be a worry for all GPs. |
30 July 2011. The British Journal of General Practice has published nine letters that object to this study. Some of them concentrate on problems with the methods. others point out what I believe to be the main point, there us essentially no effect there to be explained. In the public interest, I am posting the responses here [download pdf file]
Thers is also a response from the editor and from the authors. Both are unapologetic. It seems that the editor sees nothing wrong with the peer review process.
I don’t recall ever having come across such incompetence in a journal’s editorial process.
Here’s all he has to say.
|
The BJGP Editorial Board considered this correspondence recently. The Board endorsed the Journal’s peer review process and did not consider that there was a case for retraction of the paper or for releasing the peer reviews. The Board did, however, think that the results of the study were highlighted by the Journal in an overly-positive manner. However,many of the criticisms published above are addressed by the authors themselves in the full paper.
|
If you subscribe to the views of Paterson et al, you may want to buy a T-shirt that has a revised version of the periodic table.

5 August 2011. A meeting with the editor of BJGP
Yesterday I met a member of the editorial board of BJGP. We agreed that the data are fine and should not be retracted. It’s the conclusions that should be retracted. I was also told that the referees’ reports were "bland". In the circumstances that merely confirmed my feeling that the referees failed to do a good job.
Today I met the editor, Roger Jones, himself. He was clearly upset by my comment and I have now changed it to refer to the whole editorial process rather than to him personally. I was told, much to my surprise, that the referees were not acupuncturists but “statisticians”. That I find baffling. It soon became clear that my differences with Professor Jones turned on interpretations of statistics.
It’s true that there were a few comparisons that got below P = 0.05, but the smallest was P = 0.02. The warning signs are there in the Methods section: "all statistical tests were …. deemed to be statistically significant if P < 0.05". This is simply silly -perhaps they should have read Lectures on Biostatistics. Or for a more recent exposition, the XKCD cartoon in which it’s proved that green jelly beans are linked to acne (P = 0.05). They make lots of comparisons but make no allowance for this in the statistics. Figure 2 alone contains 15 different comparisons: it’s not surprising that a few come out "significant", even if you don’t take into account the likelihood of systematic (non-random) errors when comparing final values with baseline values.
Keen though I am on statistics, this is a case where I prefer the eyeball test. It’s so obvious from the Figure that there’s nothing worth talking about happening, it’s a waste of time and money to torture the numbers to get "significant" differences. You have to be a slavish believer in P values to treat a result like that as anything but mildly suggestive. A glance at the Figure shows the effects, if there are any at all, are trivial.
I still maintain that the results don’t come within a million miles of justifying the authors’ stated conclusion “The addition of 12 sessions of five-element acupuncture to usual care resulted in improved health status and wellbeing that was sustained for 12 months.” Therefore I still believe that a proper course would have been to issue a new and more accurate press release. A brief admission that the interpretation was “overly-positive”, in a journal that the public can’t see, simply isn’t enough.
I can’t understand either, why the editorial board did not insist on this being done. If they had done so, it would have been temporarily embarrassing, certainly, but people make mistakes, and it would have blown over. By not making a proper correction to the public, the episode has become a cause célèbre and the reputation oif the journal will suffer permanent harm. This paper is going to be cited for a long time, and not for the reasons the journal would wish.
Misinformation, like that sent to the press, has serious real-life consequences. You can be sure that the paper as it still stands, will be cited by every acupuncturist who’s trying to persuade the Department of Health that he’s a "qualified provider".
There was not much unanimity in the discussion up to this point, Things got better when we talked about what a GP should do when there are no effective options. Roger Jones seemed to think it was acceptable to refer them to an alternative practitioner if that patient wanted it. I maintained that it’s unethical to explain to a patient how medicine works in terms of pre-scientific myths.
I’d have love to have heard the "informed consent" during which "The patient’s condition is explained in terms of imbalance in the five elements which then causes an imbalance in the whole person". If anyone had tried to explain my conditions in terms of my imbalance in my Wood, Water, Fire, Earth and Metal. I’d think they were nuts. The last author. Gerad Kite, runs a private clinic that sells acupuncture for all manner of conditions. You can find his view of science on his web site. It’s condescending and insulting to talk to patients in these terms. It’s the ultimate sort of paternalism. And paternalism is something that’s supposed to be vanishing in medicine. I maintained that this was ethically unacceptable, and that led to a more amicable discussion about the possibility of more honest placebos.
It was good of the editor to meet me in the circumstances. I don’t cast doubt on the honesty of his opinions. I simply disagree with them, both at the statistical level and the ethical level.
30 March 2014
I only just noticed that one of the authors of the paper, Bruce McCallum (who worked as an acupuncturist at Kite’s clinic) appeared in a 2007 Channel 4 News piece. I was a report on the pressure to save money by stopping NHS funding for “unproven and disproved treatments”. McCallum said that scientific evidence was needed to show that acupuncture really worked. Clearly he failed, but to admit that would have affected his income.
Watch the video (McCallum appears near the end).
One of my first posts about nonsense taught in universities was about the University of Westminster (April 2008): Westminster University BSc: “amethysts emit high yin energy”. since then, there have been several more revelations.
 Professor Petts |
The vice-cnancellor of Westminster, Professor Geoffrey Petts, with whom the buck stops, did have an internal review but its report was all hot air and no action resulted (see A letter to the Times, and Progress at Westminster). That earned Professor Petts an appearence in Private Eye Crystal balls. Professor Petts in Private Eye (and it earned me an invitation to a Private Eye lunch, along with Francis Wheen, Charlie Booker, Ken Livingstone . . ). It also earned Petts an appearence in the Guardian (The opposite of science). |
By that time Salford University had closed down all its CAM, and the University of Central Lancashire was running an honest internal review which resulted in closure of (almost) all of their nonsense degrees. But Westminster proved more resistant to sense and, although they closed down homeopathy, they still remain the largest single provider of degrees in junk medicine. See, for example More make-believe from the University of Westminster. This time it’s Naturopathy, and
The last BSc (Hons) Homeopathy closes! But look at what they still teach at Westminster University.
It’s interesting that Westminster always declined to comply with Freedom of Information requests, yet I had more from them than from most places. All the information about what’s taught at Westminster came from leaks from within the university. Westminster has more moles than a suburban garden. They were people with conscience who realised that the university was harming itself. They would claim that they were trying to save the university from some remarkably bad management. I claim also that I’m working in the interests of the university.
In the wake of the victory at the Information Tribunal, I sent a Freedom of Information Act (FOIA) request for for samples of teaching materials from all of their courses. This time they couldn’t legally refuse. The first batch has just arrived, so here are a few selected gems of utter nonsense. Well, it is worse than nonsense because it endangers the health of sick people.
A letter to the university from a student
Before getting on to the slides, here’s a letter that was supplied under FOIA. It was sent anonymously to the university. I was told that this was the only letter of complaint but I happen to know that’s not true so I’ve asked again. This one was forwarded to the vice-chancellor in 2008, and to the review committee. Both seem to have ignored it. Judging from the wording, one would guess that it came from one of their own undergraduates. :Here are some extracts.[download whole letter]
|
It is a flagrant contradiction of a ‘science’ in the BSc to have these practices, but it also jeopardises our profession, which is under DoH review and being constantly attacked in the media Gustifiable I suggest). We are taught that simply tasting plant tinctures can tell us which part of the body they work. on and what they do in the body. We are given printed charts with an outline of the body on to record our findings on. This is both nonsense, but is dangerous as it implies that the pharmacology of plant tinctures can be divined by taste alone. In class we are taught that we can divine the drug actions or use of an unknown plant simply by tasting an alcohol extract. Science? or dangerous fantasy. There are lecturers taking clinics who allow students to dowse and partake themselves in dowsing or pendulums to diagnose and even to test suitability of plant drugs. Dowsing is taught to us by some lecturers and frowned upon by others but we feel it brings the herbal medicine into a poor light as it is unscientific and bogus nonsense. We are concerned that we have seen the course leader brush over this practice as though she is frightened to make a stand. |
The letter seems to refer to a course in herbal medicine. That is a subject that could be studied scientifically, though to do so would leave students unemployed because so few herbal treatments have been shown to work. It obviously is not being studied scientifically: but even teaching students about dowsing and pendulums does not seem to have stirred the vice-chancellor into action.
David Peters: wishful thinking?
David Peters is a nice man. He’s the Clinical Director of Westminster’s School of Integrated Health. I debated with him on the excellent Radio 4 Programme, Material World.
His lecture on "Complementary Healthcare in the NHS" showed some fine wishful thinking.

It shows the progress of the euphemisms that quacks use to try to gain respectability, but little else. Interestingly, later slides show a bit more realism.


So he has noticed that the tide has turned and that a lot of people are no longer willing to be palmed off with new age gobbledygook. And yes, courses are shutting. Perhaps his course will be the next to shut?
According to an internal Westminster email that found its way to me,
The following courses have been closed/identified for closure due to poor recruitment :
- BSc degrees in Homeopathy and Remedial Massage & Neuromuscular Therapy, students completing by September 2011
- MA degrees in International Community development, Community development and Faith-based Community development, students completing by September 2011
- BSc degree Complementary Medicine
- Graduate diploma BMS
The following courses have been identified as ‘at risk’ (School definition) and will be discussed at the APRG and University Review Group2, due to poor recruitment and high cost of delivery:
- Integrated Health Scheme: BSc Complementary Medicine, Naturopathy; BSc Chinese Medicine; BSc Nutritional Therapy; BSc Herbal Medicine
The BSc (Hons) degree in naturopathy
Naturopathy us pretty bizarre, because it consists largely of doing nothing at all, beyond eating vegetables . Being ill is good for you.
Perhaps the best source to judge claims is the US National Center for Complementary and Alternive Medicine (NCCAM), a branch of the National Institutes of Health. This is the outfit that has spent over a billion dollars of US taxpayers’ money testing alternative medicines and for all that money has not come up with a single useful treatment. They never link to any sort of critical comment, and are nothing if not biassed towards all things alternative. If they can’t come up with evidence. nobody can. Two useful links to NCCAM are Herbs at a glance, and Health Topics A – Z.
Uses of herbal teas in naturopathic dietary care
I was sent a set of over 50 slides on "Herbal Teas/Decoctions (3CMWS03, 1/02, Uses of herbal teas in naturopathic dietary care). About half of them amount to little more than ‘how to make a cup of tea’. but then we get onto uses, but then a lot of fantasy ensues.
What NNCAM says about dandelion. There is no compelling scientific evidence for using dandelion as a treatment for any medical condition.
What Westminster says


Well I know what a diuretic is, but "blood purifier" and "liver tonic" are meaningless gobbledygook. We’ve been through this before with Red Clover (see Michael Quinion’s .look at the term "blood cleanser"). Using words like them is the very opposite of education.
What NCCAM says.about chamomile: Chamomile has not been well studied in people so there is little evidence to support its use for any condition.
What Westminster says

So, judging by NCCAM, these claims are unjustified. It’s teaching folk-lore as though it meant something.
More dangerous advice comes when we get to the ‘repertories’.

Infections can kill you, They are one of the modest number of things that pharmacology can usually cure, rather than treat symptomatically. If you go to a Westminster-trained naturopath with a serious infection and follow their advice to put garlic in your socks, you will not just be smelly, You could die.
Allergy and Intolerance 3CMwS03 18/02
|
Treating allergies, misdiagnosed by fraudulent tests, is very big business for the ‘health food industry’, This lecture, by R. Newman Turner ND, DO, BAc, started tolerably but descended to a nadir when it mentions, apparently seriously, two of the best known fraudulent methods of allergy diagnosis, the Vega test and "Applied Kinesiology". Kinesiology Sounds sort of sciencey, but Applied Kinesiology is actually a fraudulent and totally ineffective diagnostic method invented by (you guessed) a chiropractor. It has been widely used by alternative medicine to misdiagnose food allergies. It does not work (Garrow, 1988: download reprint). |
|
Could this be the same R Newman Turner who wrote a book on Naturopathic First Aid? The mind boggles.
Naturopathic Detoxification 23 CMES03 25/02 Detox Myth of Fact
|
This lecture was the responsibility of Irving S Boxer ND DO MRN LCH, a naturopath, homeopath and osteopath in private practice. Don’t be fooled by the implied question in the title. It might have been taken to suggest a critical approach. Think again. There is all the usual make-believe about unspecified and imaginary toxins that you must get rid of with enemas and vegetables. |
|
|
The skin brushing does not quite plumb the depths of Jacqueline Young’s Taking an air bath , but presumably it is something similar. "Liver activation" by castor oil packs is pure unadulterated gobblydygook. The words mean nothing. Their attempt to divide all foods into those that cleanse and those that clog sounds reminiscent of the Daily Mail’s ontological oncology project. |
 
|
The practice of healing (3CMSS01 2/12)
Next we retreat still further into fantasy land

|

|
All pure hokum, of course’ She could have added "craniosacral therapy" (at present the subject of a complaint against the UCL Hospitals Trust (that’s the NHS, not UCL) to the Advertising Standards Authority,
 |
 |
Is that definition quite clear?
In fact this sort of nonsense about rays coming from your hands was disproved experimentally, in a rather famous paper, the only paper in the Journal of the American Medical Association to have been written by a 9-year old. Emily Rosa. She (with some help from her parents) devised a simple test for her 4th (US) grade science fair project. It was later repeated under more controlled conditions and written up for JAMA [download reprint] . It showed that the claims of ‘therapeutic touch" practitioners to be able to detect "auras" were totally false. No subsequent work has shown otherwise. Why, then, does the University of Westminster teach it as part of a Bachelor of Science degree?
You can see Emily Rosa herself explain why “therapeutic touch is bullshit” with Penn and Teller, in Penn and Teller Expose Therapeutic Touch.
Environmental stress
The last bit of hokum (for the moment) is one of the best. This one has every myth under the sun (including some I hadn’t heard of).

|
The lecturer, Val Bullen, was also responsible for the infamous "Amethysts emit high Yin energy" slide. One of her own students desribes her as "sweet but deluded". I have nothing against Ms Bullen, She can believe whatever she wants. My problem is with the vice-chancellor, Prof Geoffrey Petts, who seems to think that this sort of stuff is appropriate for a BSc. |

|
Everything barmy is here. Mobile phones, power lines, underwater streams, ley lines, sick building syndrome, are all reasons why you don’t feel 100 percent, Actually my reason is having to read this junk. The "definitions" are, as always, just meaningless words.
|
But don’t despair. Help is at hand.

Just in case you happen to have run out of Alaskan Calling All Angels Essence, you can buy it from Baldwin’s for £19.95. It’s "designed to invoke the nurturing, uplifting and joyful qualities of the angelic kingdom.", and what’s more "can also use them any time to cleanse, energize, and protect your auric field." Well that’s what it says.in the ad.
Yarrow Environmental Solution looks like good stuff too. Only £7.95 for 7.5 ml. For that you get a lot. It will
" . . strengthen and protect against toxic environmental influences, geopathic stress, and other hazards of technology-dominated modern life. This includes the disruptive effects of radiation on human energy fields from X-rays, televisions, computer monitors, electromagnetic fields, airplane flights or nuclear fall-out."
OK stop giggling. This is serious stuff, taught in a UK university as part of a BSc degree, and awarded a high score by the Quality Assurance Agency (QAA).
Professor Petts, are you listening? I believe it is you, not I, who is bringing your university into disrepute.
The slides shown here are copyright of the University of Westminster or of the author of the lecture. They are small sample of what I was sent and are reproduced under the “fair quotation” provision, in the public interest.
Follow-up
5 May 2011. By sheer coincidence, Emily and Linda Rosa were passing through London. They called for lunch and here’s a picture (with Ben Goldacre) in UCL’s (endangered) Housman room. Linda kindly gave me a copy of her book Attachment Therapy on Trial: The Torture and Death of Candace Newmaker. [Download reprint of Rosa’s paper..]

.
6 May 2011. Talking of the “vibrational medicine” fantasy, I had an email that pointed out a site that plumbs new depths in fantasy physics. It’s on the PositiveHealthOnline website: A post there, Spirals and Energy in Nature, was written by Robert McCoy. He claims to have worked on microprocessor layout design, but anyone with school physics could tell that the article is sheer nonsense. In a way it is much more objectionable that the silly slides with coloured rays used in the Westminster course. McCoy’s post seeks to blind with sciencey-sounding language, that in fact makea no sense at all. Luckily my retweet of the site attracted the attention of a real physicist, A.P. Gaylard, who made a very welcome return to blogging with Fantasy physics and energy medicine. He dismantles the physics, line-by-line, in a devastating critique. This sort of junk physics is far more dangerous than the perpetual motion pundits and the cold-fusion fantasists. At PositiveHealthOnline it is being used to push pills that do you no good and may harm you. It is a danger to public health.
This is a slightly-modified version of the article that appeared in BMJ blogs yesterday, but with more links to original sources, and a picture. There are already some comments in the BMJ.
The original article, diplomatically, did not link directly to UCL’s Grand Challenge of Human Wellbeing, a well-meaning initiative which, I suspect, will not prove to be value for money when it comes to practical action.
Neither, when referring to the bad effects of disempowerment on human wellbeing (as elucidated by, among others, UCL’s Michael Marmot), did I mention the several ways in which staff have been disempowered and rendered voiceless at UCL during the last five years. Although these actions have undoubtedly had a bad effect on the wellbeing of UCL’s staff, it seemed a litlle unfair to single out UCL since similar things are happening in most universities. Indeed the fact that it has been far worse at Imperial College (at least in medicine) has probably saved UCL from being denuded. One must be thankful for small mercies.
There is, i think, a lesson to be learned from the fact that formal initiatives in wellbeing are springing up at a time when university managers are set on taking actions that have exactly the opposite effect. A ‘change manager’ is not an adequate substitute for a vote. Who do they imagine is being fooled?
The A to Z of the wellbeing industry
From angelic reiki to patient-centred care
Nobody could possibly be against wellbeing. It would be like opposing motherhood and apple pie. There is a whole spectrum of activities under the wellbeing banner, from the undoubtedly well-meaning patient-centred care at one end, to downright barmy new-age claptrap at the other end. The only question that really matters is, how much of it works?
Let’s start at the fruitcake end of the spectrum.
One thing is obvious. Wellbeing is big business. And if it is no more than a branch of the multi-billion-dollar positive-thinking industry, save your money and get on with your life.
In June 2010, Northamptonshire NHS Foundation Trust sponsored a “Festival of Wellbeing” that included a complementary therapy taster day. In a BBC interview one practitioner used the advertising opportunity, paid for by the NHS, to say “I’m an angelic reiki master teacher and also an angel therapist.” “Angels are just flying spirits, 100 percent just pure light from heaven. They are all around us. Everybody has a guardian angel.” Another said “I am a member of the British Society of Dowsers and use a crystal pendulum to dowse in treatment sessions. Sessions may include a combination of meditation, colour breathing, crystals, colour scarves, and use of a light box.” You couldn’t make it up.
The enormous positive-thinking industry is no better. Barbara Ehrenreich’s book, Smile Or Die: How Positive Thinking Fooled America and the World, explains how dangerous the industry is, because, as much as guardian angels, it is based on myth and delusion. It simply doesn’t work (except for those who make fortunes by promoting it). She argues that it fosters the sort of delusion that gave us the financial crisis (and pessimistic bankers were fired for being right). Her interest in the industry started when she was diagnosed with cancer. She says
”When I was diagnosed, what I found was constant exhortations to be positive, to be cheerful, to even embrace the disease as if it were a gift. If that’s a gift, take me off your Christmas list,”
It is quite clear that positive thinking does nothing whatsoever to prolong your life (Schofield et al 2004; Coyne et al 2007; 2,3), any more than it will cure tuberculosis or cholera. “Encouraging patients to “be positive” only may add to the burden of having cancer while providing little benefit” (Schofield et al 2004). Far from being helpful, it can be rather cruel.
Just about every government department, the NHS, BIS, HEFCE, and NICE, has produced long reports on wellbeing and stress at work. It’s well known that income is correlated strongly with health (Marmot, M., 2004). For every tube stop you go east of Westminster you lose a year of life expectancy (London Health Observatory). It’s been proposed that what matters is inequality of income (Wilkinson & Pickett, 2009). The nature of the evidence doesn’t allow such a firm conclusion (Lynch et al. 2004), but that isn’t really the point. The real problem is that nobody has come up with good solutions. Sadly the recommendations at the ends of all these reports don’t amount to a hill of beans. Nobody knows what to do, partly because pilot studies are rarely randomised so causality is always dubious, and partly because the obvious steps are either managerially inconvenient, ideologically unacceptable, or too expensive.
Take two examples:
Sir Michael Marmot’s famous Whitehall study (Marmot, M., 2004) has shown that a major correlate of illness is lack of control over one’s own fate: disempowerment. What has been done about it?
In universities it has proved useful to managers to increase centralisation and to disempower academics, precisely the opposite of what Marmot recommends.
|
As long as it’s convenient to managers they are not going to change policy. Rather, they hand the job to the HR department which appoints highly paid “change managers,” who add to the stress by sending you stupid graphs that show you emerging from the slough of despond into eternal light once you realise that you really wanted to be disempowered after all. Or they send you on some silly “resilience” course. |
|
A second example comes from debt. According to a BIS report (Mental Capital and Wellbeing), debt is an even stronger risk factor for mental disorder than low income. So what is the government’s response to that? To treble tuition fees to ensure that almost all graduates will stay in debt for most of their lifetime. And this was done despite the fact that the £9k fees will save nothing for the taxpayer: in fact they’ll cost more than the £3k fees. The rise has happened, presumably, because the ideological reasons overrode the government’s own ideas on how to make people happy.
Nothing illustrates better the futility of the wellbeing industry than the response that is reported to have been given to a reporter who posed as an applicant for a “health, safety, and wellbeing adviser” with a local council. When he asked what “wellbeing” advice would involve, a member of the council’s human resources team said: “We are not really sure yet as we have only just added that to the role. We’ll want someone to make sure that staff take breaks, go for walks — that kind of stuff.”
The latest wellbeing notion to re-emerge is the happiness survey. Jeremy Bentham advocated “the greatest happiness for the greatest number,” but neglected to say how you measure it. A YouGov poll asks, “what about your general well-being right now, on a scale from 1 to 10.” I have not the slightest idea about how to answer such a question. As always some things are good, some are bad, and anyway wellbeing relative to whom? Writing this is fun. Trying to solve an algebraic problem is fun. Constant battling with university management in order to be able to do these things is not fun. The whole exercise smacks of the sort of intellectual arrogance that led psychologists in the 1930s to claim that they could sum up a person’s intelligence in a single number. That claim was wrong and it did great social harm.
HEFCE has spent a large amount of money setting up “pilot studies” of wellbeing in nine universities. Only one is randomised, so there will be no evidence for causality. The design of the pilots is contracted to a private company, Robertson Cooper, which declines to give full details but it seems likely that the results will be about as useless as the notorious Durham fish oil “trials”(Goldacre, 2008).
Lastly we get to the sensible end of the spectrum: patient-centred care. Again this has turned into an industry with endless meetings and reports and very few conclusions. Epstein & Street (2011) say
“Helping patients to be more active in consultations changes centuries of physician-dominated dialogues to those that engage patients as active participants. Training physicians to be more mindful, informative, and empathic transforms their role from one characterized by authority to one that has the goals of partnership, solidarity, empathy, and collaboration.”
That’s fine, but the question that is constantly avoided is what happens when a patient with metastatic breast cancer expresses a strong preference for Vitamin C or Gerson therapy, as advocated by the YesToLife charity. The fact of the matter is that the relationship can’t be equal when one party, usually (but not invariably) the doctor, knows a lot more about the problem than the other.
What really matters above all to patients is getting better. Anyone in their right mind would prefer a grumpy condescending doctor who correctly diagnoses their tumour, to an empathetic doctor who misses it. It’s fine for medical students to learn social skills but there is a real danger of so much time being spent on it that they can no longer make a correct diagnosis. Put another way, there is confusion between caring and curing. It is curing that matters most to patients. It is this confusion that forms the basis of the bait and switch tactics (see also here) used by magic medicine advocates to gain the respectability that they crave but rarely deserve.
If, as is only too often the case, the patient can’t be cured, then certainly they should be cared for. That’s a moral obligation when medicine fails in its primary aim. There is a lot of talk about individualised care. It is a buzzword of quacks and also of the libertarian wing which says NICE is too prescriptive. It sounds great, but it helps only if the individualised treatment actually works.
Nobody knows how often medicine fails to be “patient-centred.”. Even less does anyone know whether patient-centred care can improve the actual health of patients. There is a strong tendency to do small pilot trials that are as likely to mislead as inform. One properly randomised trial (Kinmonth et al., 1998) concluded
“those committed to achieving the benefits of patient centred consulting should not lose the focus on disease management.”
Non-randomised studies may produce more optimistic conclusions (e.g. Hojat et al, 2011), but there is no way to tell if this is simply because doctors find it easy to be empathetic with patients who have better outcomes.
Obviously I’m in favour of doctors being nice to patients and to listening to their wishes. But there is a real danger that it will be seen as more important than curing. There is also a real danger that it will open the doors to all sorts of quacks who claim to provide individualised empathic treatment, but end up recommending Gerson therapy for metastatic breast cancer. The new College of Medicine, which in reality is simply a reincarnation of the late unlamented Prince’s Foundation for Integrated Health, lists as its founder Capita, the private healthcare provider that will, no doubt, be happy to back the herbalists and homeopaths in the College of Medicine, and, no doubt, to make a profit from selling their wares to the NHS.
In my own experience as a patient, there is not nearly as much of a problem with patient centred care as the industry makes out. Others have been less lucky, as shown by the mid-Staffordshire disaster (Delamothe, 2010), That seems to have resulted from PR being given priority over patients. Perhaps all that’s needed is to save money on all the endless reports and meetings (“the best substitute for work”), ban use of PR agencies (paid lying) and to spend the money on more doctors and nurses so they can give time to people who need it. This is a job that will be hindered considerably by the government’s proposals to sell off NHS work to private providers who will be happy to make money from junk medicine.
Reference
Wilkinson. R & Pickett, K. 2009 , The Spirit Level, ISBN 978 1 84614 039 6
A footnote on Robertson Cooper and "resilience"
I took up the offer of Robertson Cooper to do their free "resilience" assessment, the company to which HEFCE has paid an undisclosed amount of money.
The first problem arose when it asked about your job. There was no option for scientist, mathematician, university or research, so I was forced to choose "education and training". (a funny juxtaposition since training is arguably the antithesis of education). It had 195 questions. mostly as unanswerable as in the YouGov happiness survey. I particularly liked question 124 "I see little point in many of the theoretical models I come across". The theoretical models that I come across most are Markov models for the intramolecular changes in a receptor molecule when it binds a ligand (try, for example, Joint distributions of apparent open and shut times of single-ion channels and maximum likelihood fitting of mechanisms). I doubt the person who wrote the question has ever heard of a model of that sort. The answer to that question (and most of the others) would not be worth the paper they are written on.
The whole exercise struck me as the worst sort of vacuous HR psychobabble. It is worrying that HEFCE thinks it is worth spending money on it.
Follow-up
As promised in my last post about Edinburgh Napier University, I wrote to the vice-chancellor of the university, Professor Dame Joan K. Stringer DBE, BA (Hons) CertEd PhD CCMI FRSA FRSE, to invite her to respond.
|
7 February, 2011 Dear Professor Stringer, I should be grateful if you could let me know about your opinion of the degrees that you offer in Aromatherapy and Reflexology I have posted on my blog a bit of the material that was sent to me as result of recent FoI requests. See https://www.dcscience.net/?p=4049 I submit that degrees like this detract from the intellectual respectability of what is, not doubt, in other respects a good university, but since you are mentioned in the post, it’s only fair to give you the chance to defend yourself. In fact you’d be very welcome to do so publicly by commenting on the post. Best regards David Colquhoun |
Over a month later, I have received no response at all. This seems to me to be a bit discourteous.
There is nothing new in failing to get any answer to letters to vice-chancellors. The only VC who has ever thanked me for opening his eyes is Terence Kealey, of the University of Buckingham. All the rest have stayed silent. I can interpret this silence only as guilt. They know it’s nonsense, but dare not say so. Of course it isn’t infrequent for the course to close down after public exposure of the nonsense they teach. So perhaps the letters get read, even if they don’t elicit a reply.
Meanwhile the university sent me more materials that are used to teach their students. So here is another sample, largely from what’s taught to the unfortunate “reflexology” students.
Remember, these pre-scientific myths are not being taught as history or anthropology. They are taught as though they were true, to students who are then let loose on patients, so they can make money from anyone who is gullible enough to believe what they say.

There are no "excess body energies". It’s made-up nonsense.
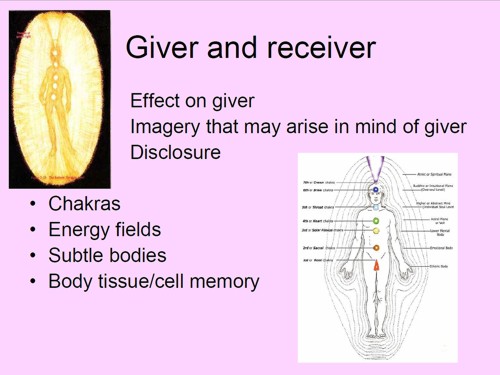
The diagram is pure imagination. It dates form a time before we knew anything about physiology, yet it is still being taught as though it meant something.

The admission that there is controversy is interesting. But it doesn’t seem to deter Napier’s teachers in the slightest.

How can anyone in the 21st century believe that the heart is "king of our emotional existence”?. That’s just preposterous pre-scientific myth,

You must be joking.


"Vibrational medicine" is a non-existent subject. Pure gobbledygook.
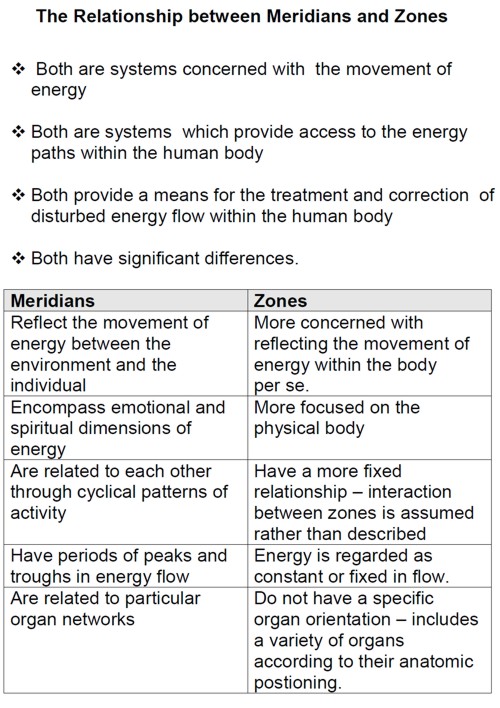
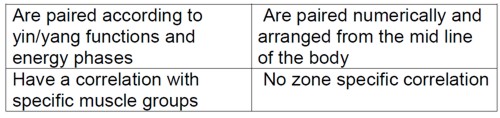
This is partly old, partly quite new. It is all preposterous made-up nonsense. There isn’t the slightest reason to think that "zones" or "meridians" exist. In fact there is good evidence from acupuncture studies to think that they don’t exist.
Now some slides from course CPT08102. The mention of the word ‘energy’ in the alternative world always rings alarm bells. Here’s why.

Well, it’s a good question. Pity about the answer.

Shouldn’t that read "as a practising reflexologist it is important than you have a MISunderstanding of the energy that surrounds us"?.

![]()
What logic? Have these people never heard of Hodgkin & Huxley (the answer, I imagine, is no)?

The mention of Kim Jobst immediately raises suspicions. He is a homeopath and endorser of the obviously fraudulent Q-link
pendant.
"when you as a reflexologist palpate the foot you not only produce the physical responses in the CNS but also enter the energetic body and move energy , , ". Well, no you don’t. This is purely made-up nonsense. The words sound "sciencey" but the meaning of the words is utterly obscure.

Yes we do live in an interconnected world. And sadly, that interconnectedness is used to spread myth and misinformation, usually with the aim of making money.
I guess Edinburgh Napier University makes money by teaching ancient myths as though they were true. In so doing they destroy their academic reputation.

Here you are tested to see how much nonsense you have memorised successfully. If only they had sent ‘model answers’.
Remember, these pre-scientific myths are not being taught as history or anthropology. They are taught as though they were true, to students who are then let loose on patients, so they can make money from anyone who is gullible enough to believe what they say.
A 2009 systematic review of randomised controlled trials concludes that “The best evidence available to date does not demonstrate convincingly that reflexology is an effective treatment for any medical condition.”. So forget it.
How about it Professor Stringer? Isn’t it time to clean up your university?
Follow-up
|
The Science Museum is a wonderful place. As a child it seemed magical. So all the more disappointing to find that it houses an exhibition that promotes quackery. The exhibition is uncritical and sometimes downright dangerous. It does not teach you anything about science, it teaches anti-science and uncritical thinking. It was not originally like this. Most of the objects in the exhibition were originally part of Henry Wellcome’s Wellcome Museum of Medical History, based at 183 Euston Road. It was moved on permanent loan to the Science Museum in 1977 where it was known as The Wellcome Museum of the History of Medicine. |
|
Recently the Wellcome-Trust sponsored exhibition was the subject of a blog post at Purely a figment of your imagination, written by Alex Davenport. That reminded me that last June I was sent a lot of pictures of the exhibition but never got round to finishing writing them up. Here, somewhat tardily, is some of what I got.
It seems that the Wellcome Trust is not to blame, The free advertising for quacks was something added to the Wellcome collection by the Science Museum itself.
At the time, I wrote to the Science Museum to find out what was going on. The response was very disappointing, merely bland PR stuff. I was told that the person responsible for the display was Lisa O’Sullivan, Senior Curator of Medicine, but she was on sabbatical, so no response from her.
The clue to what went wrong came in a letter from Dr. Tim Boon, the Science Museum’s Chief Curator. The letter was relayed via the Museum’s Press Officer. A subsequent letter to Boon himself was not answered.
"Therefore, in addition to the overwhelming majority of the Upper Wellcome gallery that tells the story of the history of Western medicine since the rise of Civilisation up to the modern era, we devote a small section to these more anthropological concerns in our display called ‘Living Medical Traditions’.
Our message in this display is that these traditions are not ‘alternative’ systems in some parts of the world. Instead they are often the only choice of medical care to those communities. We do not make any claims for the validity of these traditions. For example, we include the use of acupuncture but do not say that acupuncture ‘works’. "
Unfortunately this is really not true: the tone is very much that it does work. The reason is clear in the next paragraph.
"As with all Science Museum galleries independent experts were consulted when developing this gallery. In this instance advice was sought from leading academics in the history of non-western medical traditions as well as practitioners and users of these traditions. We maintained editorial control throughout.”
Aha they asked "experts", but of course it is always possible to find some ‘expert’ to advocate any view, however barmy. The only experts that were consulted, we are told, is historians and practitioners of anti-scientific medicine. No scientists. Clearly the Museum allowed the quacks to write their own script, with no supervision from anyone who understands the science, It is meant to be a Science Museum, not a museum of anthropology.
The nonsense of quack medicine provides an excellent opportunity to explain simply how science tries to separate truth from falsehood. The Museum has not only missed that opportunity but it has actively promoted anti-science.
The Museum declined to name these mystery experts, but one of them is revealed in the 2006 newsletter of the British Medical Acupuncture Society [download the newsletter]. An article by Jonathan Freedman shows the delight of acupuncturists.
"The BMAS were approached by the Museum last Summer and asked if any members would be able to contribute a case study about acupuncture to feature in the ‘personal stories’ section of the exhibition."
"I think the final product has worked extremely well and shows Western Medical Acupuncture in a positive light. A selection of needles is displayed along with the BMAS leaflet and my own practice acupuncture leaflet."
In fact the Science Museum’s good name is used by Freedman to advertise his private practice.
Here is the free advertising in the Science Museum.

Traditional Chinese Medicine
There is plenty of this and it is totally uncritical. All it does is repeat the gobbledygook used by practitioners. In fact it was largely written by them.



There are recorded commercials too. Listen to this one.

Advertising for cupping at the Asanté Clinic.
In the recording, Dr Ke diagnoses an asthma patient as having mucus in the lungs -by looking at his tongue (no kidding) -and recommends cupping. He says
“We need to clear this mucus, or the phlegm, in the chest by using cupping, It’s improving, sort of, the flow of the water, and flow out, in other words, suck out the badness from the body”
This, needless to say, is total rubbish.
The recording took place at the Asanté Clinic, on the Archway campus of the University of Middlesex. Ah yes, Middlesex. Take a look at ‘More quackedemia. Dangerous Chinese medicine taught at Middlesex University‘.
Unani medicine, Another advertisement for a private clinic.
|
|
|
Listen to a diagnosis being made by looking at the iris.
Iridology is, of course, total bunk Just one of the many phoney methods of diagnosis used by alternative practitioners, as an aid to selling you an expensive treatment.
Ayervedic medicine
Listen to another advertisement, for private Ayurveda clinic
The display that accompanies the recording is totally uninformative. The practitioners have been allowed to advertise their wares with no trace of critical thought. No trace of science.
|
|
|
|
|
|
|
|
|
The power of blogs
I guess this incident is yet another example of the power of blogs. My own letters to the science museum produced precisely nothing, as is usually the case if you go through the “proper channels”. Alex Davenport’s blog,on the other hand, stung the Science Museum into a public response. It’s true that the response is much the same as the patronising PR junk that was sent to me last year, though it was labelled as being by Susannah Shute, Web Content Coordinator. The response even linked to a picture of the homeopathy exhibit.
It seems a bit more pressure is needed to persuade the museum to change this particular exhibition into science, rather than its present anti-science.
Follow-up
13 April 2011. Simon Singh arranged a meeting with the new director of the Science Museum, Ian Blatchford, and deputy director Heather Mayfield Our deputation consisted of Simon Singh, Alex Davenport, Marianne Baker and me. It was Alex’s blog on the science museum exhibit, and my post on the museum which followed it shortly, that caused the meeting. Alex had a follow-up blog too. I hadn’t realised that Simon had resigned as a trustee of the museum five years ago, in protest about the (dreadful) alternative medicine exhibit. I had various stonewalling responses to my attempts to pursue the matter out of the limelight, so eventually went public. After the blogs appeared, the Science Museum published a response which was, sadly, entirely vacuous. We had an excellent discussion, during which Ian Blatchford said he regretted the official response and changes to the exhibit are promised. there is an account of the meeting here.
We were sent a revised version, which was improved, but not, we said improved enough.
10 May 2011. Got an email from the person who originally brought the problem to my attention.
“Visited Science museum yesterday , wonderful news – all offensive material gone, and different ok stuff there”.
Well done, Science Museum.


















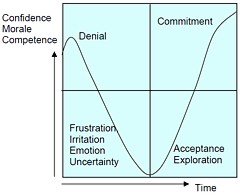
 >
>