Today brings a small setback for those of us interested in spreading sensible ideas about science. According to a press release
“The BMJ Group is to begin publishing a medical journal on acupuncture from next year, it was announced today (Tuesday 11 November 2008).
This will be the first complementary medicine title that the BMJ Group has published.”
And they are proud of that? What one earth is going on? The BMJ group is a publishing company which says, of itself,
“Our brand stands for medical credibility. We are one of the world’s best known and most respected medical publishers.”
Well perhaps it used to be.
They have certainly picked a very bad moment for this venture. In the last year there have been at least five good books that assess the evidence carefully and honestly. Of these, the ones that are perhaps the best on the subject of acupuncture are Singh & Ernst’s Trick or Treatment and Barker Bausell’s Snake Oil Science. Both Ernst and Bausell have first hand experience of acupuncture research. And crucially, none of these authors has any financial interest in whether the judgement goes for acupuncture or against it.
Here are quotations from Singh & Ernst’s conclusions
“Reliable conclusions from systematic reviews make it clear that acupuncture does not work for a whole range of conditions, except as a placebo.”
“There are some high quality trials that support the use of acupuncture for some types of pain and nausea, but there are also high quality trials that contradict this conclusion. In short, the evidence is neither consistent nor convincing – it is borderline.”
The House of Lords’ report in 2000 tended to give acupuncture the benefit of the (very considerable) doubt that existed at the time the report was written. Since that time there have been a lot of very well-designed trials of acupuncture.
Now it is quite clear that, for most (and quite possibly all) conditions, acupuncture is no more than a particularly theatrical placebo. Perhaps that is not surprising insofar as the modern western practice of acupuncture owes more to Chinese nationalistic propaganda that started in the time of Mao-Tse Tung than it owes to ancient wisdom (which often turns out to be bunk anyway).
The BMJ Group has decided to endorse acupuncture at a time when it is emerging that the evidence for any specific effect is very thin indeed. Well done.
The journal in question is this.
Acupuncture in Medicine is a quarterly title, which aims to build the evidence base for acupuncture. It is currently self-published by the British Medical Acupuncture Society (BMAS).
One good thing can be said about the Society and the Journal. That is that they don’t espouse all the mumbo-jumbo about ‘meridians’ and ‘Qi’. This, of course, puts them at odds with the vast majority of acupuncture teaching. This sort of internecine warfare between competing sects is characteristic of all sorts of alternative medicine. But that is just ideology. What matters is whether or not sticking needles in you is actually anything more than a placebo.
British Medical Acupuncture Society (BMAS)
The British Medical Acupuncture Society (BMAS). is “a registered charity established to encourage the use and scientific understanding of acupuncture within medicine for the public benefit.”. The phrase “encourage the use” suggests that they do not even envisage the possibility that it might not work. Their web site includes these claims.
Acupuncture can help in a variety of conditions:
- Pain relief for a wide range of painful conditions
- Nausea, especially postoperative nausea and vomiting
- Overactive bladder, also known as bladder detrusor instability
- Menstrual and menopausal problems, eg period pains and hot flushes
- Allergies such as hay fever and some types of allergic rashes
- Some other skin problems such as ulcers, itching and localised rashes
- Sinus problems and more
Presumably the word “help” is chosen carefully to fall just short of “cure”. The claims are vaguely worded, but let’s see what we can find about them from systematic reviews. It appears that the BMAS is being rather optimistic about the evidence.
BMJ Clinical Evidence is considered reliable and is particular interesting because it is owned by the BMJ Publishing Group.
Low Back Pain (chronic) Acupuncture is listed as being of “unknown effectiveness”.
Dysmenorrhoea Acupuncture is listed as being of “unknown effectiveness”.
Osteoarthritis of the knee. Acupuncture is listed as being of “unknown effectiveness”.
Psoriasis (chronic plaque) Acupuncture is listed as being of “unknown effectiveness”.
Neck pain “Acupuncture may be more effective than some types of sham treatment (not further defined) or inactive treatment (not further defined) at improving pain relief at the end of treatment or in the short term (less than 3 months), but not in the intermediate term (not defined) or in the long term (not defined)”
Headache (chronic tension-type) Acupuncture is listed as being of “unknown effectiveness”.
What about the greatest authority, the Cochrane Reviews?
Cochrane Reviews
Low back pain The data do not allow firm conclusions about the effectiveness of acupuncture for acute low-back pain. For chronic low-back pain, acupuncture is more effective for pain relief and functional improvement than no treatment or sham treatment immediately after treatment and in the short-term only. Acupuncture is not more effective than other conventional and “alternative” treatments. The data suggest that acupuncture and dry-needling may be useful adjuncts to other therapies for chronic low-back pain. Because most of the studies were of lower methodological quality, there certainly is a further need for higher quality trials in this area.
Chronic asthma. There is not enough evidence to make recommendations about the value of acupuncture in asthma treatment. Further research needs to consider the complexities and different types of acupuncture.
But most of the vaguely-worded claims made by BMAS have not been the subject of Cochrane reviews. The obvious interpretation of that is that there is not enough evidence to make it worth writing a review. In which case, why does BMAS claim that acupuncture can “help”?
Bandolier is another excellent source of high quality information, This was their view in September 2006
“Large, high-quality randomised trials of acupuncture have been published since the reviews. In fibromyalgia, chemotherapy-induced nausea and vomiting, breech presentation, tension headache, and migraine, all were negative compared with sham acupuncture. One in osteoarthritis of the knee, had statistical improvement over sham acupuncture at three months, but not later. Both large trials and this review of reviews come to the same general conclusion; that over a whole range of conditions and outcomes acupuncture cannot yet be shown to be effective.”
After thousands of years of acupuncture (or at least almost 40 years in the West) there seems to be very little to show for it.
The journal: Acupuncture in Medicine
What about the journal in question? Like all journals devoted to alternative medicine, it claims to be evidence-based. And like all journals devoted to alternative medicine it suffers from a fatal conflict of interest. If this journal were ever to conclude that acupuncture is a placebo, it would destroy the journal and the livelihoods of many of the people who write for it.
Scanning the first three issues of 2008 shows that it is very much like other alternative medicine journals. Most of the papers don’t address the critical question, is it a placebo. And most papers end up rather limply, with a statement along the lines “acupuncture may be useful for ***. More research is needed.”
The editor in chief of the journal is Dr Adrian White, and its editor is Michael Cummings. White is quoted by Ernst in the Guardian in 2004.
“We need to provide hard evidence to support what we all see in our clinics every day: that the modern approach to acupuncture works, and is highly relevant to the new, patient-centred NHS.” .
That means the answer is assumed in advance. That just isn’t science.. ‘We know the answer, all we have to do now is get some evidence’.
Why should the BMJ Group want to do a thing like this?
The press release says
Commenting on the move, BMJ and BMJ Journals Publishing Director, Peter Ashman, said “The journal is a good complement for our existing portfolio of journals and we’re certain that the Society’s members and other subscribers will appreciate the benefits of the decision the BMAS has made on their behalf.”
He continued: “The BMAS is ambitious for its journal to grow and flourish and we’re looking forward to working with the Society to develop an editorial and commercial strategy which will achieve the aims of BMAS and those of its members, while reaching out to the wider global community interested in this fascinating area of medicine.”
Yes, you got it. Money. The same motive that causes some vice-chancellors to bring their university into disrepute by awarding BSc degrees in subjects that are not only not science, but which are oftenly openly anti-science.
Conscience doesn’t seem to bother these people, so let’s put the problem in purely cash terms.
Both the BMJ Group and the vice-chancellors will have to decide whether the cash they gain is sufficient to counterbalance the corrosive effects of their actions on their own reputations.
Follow-up
Only a couple of days later, two new trials show acupuncture is no different from sham controls for helping IVF pregnancy rates. James Randerson in the Guardian writes thus.
“Acupuncture aimed at improving IVF success rates is widely offered by fertility clinics in the UK. In the first of the studies, researchers in Hong Kong split 370 women receiving IVF into two groups. One group received real acupuncture before and after having an IVF embryo implanted into their uterus. The other had the same procedure, except the treatment used retractable needles that did not penetrate the skin.”
“Of the 185 who received the sham treatment, 91 achieved a clinical pregnancy (foetal heartbeat identified using ultrasound) and 71 had a successful delivery. This compared with 72 clinical pregnancies in the true acupuncture group and 55 live births. The differences between the groups were not statistically significant.”
“In a second study, researchers in Chicago used a similar design in which 124 women received true or sham acupuncture. The control group had their skin punctured by real acupuncture needles, but not at genuine “Qi-lines” on the body. In the true acupuncture group, 43.9% achieved a clinical pregnancy, compared with 55.2% of the women given the sham treatment. “
The original paper for the first study can be seen here.


The instructions for authors in “Acupuncture in Medicine” raise a few eyebrows. And I quote:
“The editors encourage authors to use a lively writing style. Think clearly what you wish to say, and then state it in the words you would use if you were talking to a colleague. Many authors assume they should use a formalised style for writing scientific papers, thinking this shows that their work is objective. In fact, this just makes papers difficult to read. For example, please avoid the passive voice where possible by using the first person, and by checking the text for any unnecessary passive constructions. Use short words, and do not use three when one will do. When a technical word has to be repeated because there is no real alternative, then repeat it. Be careful with abbreviations: any that are unfamiliar may cause the reader to hesitate. So do not use many, but once you have introduced one keep using it.”
I guess those PR fellas know their “target demographic”!
At a time where the great acupuncture research project has clearly demonstrated that acupuncture is not effective above and beyond placebo it seems odd to launch a whole new journal in its honour.
On the subject of acupuncture now that good methodologies have been applied and have found the expected negative results, pro-acupuncture researchers are left with fudging their conclusions as a way of peddling their placebo. Take a recent systematic review for low back pain.
The results say “There is moderate evidence that acupuncture is more effective than no treatment, and strong evidence of no significant difference between acupuncture and sham acupuncture”.
No surpises there. Now sit back take a breath and read the conclusion in the abstract which says:
“Acupuncture versus no treatment, and as an adjunct to conventional care, should be advocated in the European Guidelines for the treatment of chronic LBP”.
Unbelievable interpretive license (not to mention political meddling)! And this in a respectable journal. A failure of peer review. Ho hum.
Ref: Yuan J, Purepong N, Kerr DP et al. Effectiveness of Acupuncture for Low Back Pain. A Systematic Review. Spine 2008;33:23: E887-900
i have no problems with the suggestions on style in writing. There is indeed no need to adopt the passive voice when writing academic papers and in this age with word limits on papers using three words where one will do only limits what you can say.
In fact if you do what I am wont to do and delve into the stack and look at say the Royal Society and Zoological Society journals from the latter decades of the 19thC the style is active and personal. Those guys also had space to basically list their raw data. There are some very nice pictures too, beautiful watercolours of plants, corals etc and some good microphotography.
How very depressing!
I’ll bet the BMAS is ambitious for its journal to grow and flourish, specially via the BMJ group. Lots of street cred.
A glance at the BMAS website might lead you to think that all its members are medically qualified. However, further scrutiny reveals that, ‘Membership is open to any UK registered health professionals with an interest in acupuncture’. A chiropractor can be described as a health professional, registered with the Chiropractic Council (see DC’s posting on chiropractic).
Whilst the BMAS may not endorse meridians and qi, they seem to like Traditional Chinese Medicine.
Some members of the BMAS are not only trained as orthodox health professionals, but are also trained in TCM.
Trouble is, it gives green lights to universities everywhere to……. Oh H**l’s teeth, this whole business is getting more and more like a sort of Alice in Wonderland approach to medicine.
.
The BMAS is a registered charity established to stimulate and promote the use and scientific understanding of acupuncture as part of the practice of medicine for the public benefit. Note that ‘use’ comes before science nothing new there then.
I wonder whether the BMAS is leaping into this opportunity pdq before the government consultation on the Pitillo report on the regulation of acupuncture and TCM. (That is if indeed the consultation ever happens. My e-mail from the DoH, received on Thu, 18 Sep 2008, said, “The Department is hoping to launch the consultation within the next few weeks”. Maybe my idea of a few weeks is on the small side. No sign of it yet though.).
Sigh again.
Thought I had better add this post again as neoconnell’s post references it.
_____________________________________________
I read that abstract. As someone who prefers rocks to gallstones I wonder if someone can help me out here.
My take on the abstract is:
1) The study realtes to non-specific LBP therefore I wonder how “cures” can be specifically targeted. No comparison of like with like as they are presumably covering a multiplicity of possible causes.
2) Is it valid to look at acupuncture where conventional medicine is used as a control group.
3) Surely the statement that acupuncture is more effective than no treatment is fairly obvious – errr placebo probably, spontaneous recovery from a non-specific LBP, general variation in the level of pain, tendency to get better when pain is worse etc
Surely the results are insufficient to justify the conclusion that acupuncture should be advocated in the European Guidelines (or indeed any conclusion).
So sham acupuncture is as effective as acupuncture – shome mishtake shurely ! Does this not tend to confirm Point 3 above and work against the underlying (supposed) reasons why acupuncture works.
Or have I misunderstood something.
In response to peoples comments yesterday (it will make more sense when the other posts reappear):
Dear all, I happily take your point taken re: the style guidelines – A bit unfair of me and I must try to be less old fashioned!
In reply to John Hoopers second comment:
It is common to study non specific low back pain in trials as unfortunately in the large majority of cases of back pain no specific causative pathology can be identified (around 85% of cases). Indeed there are very few tissue based or symptom based markers that predict prognosis in back pain.
The use of conventional care as a comparison group is a contentious one. In terms of the chronic back pain population it is a poor comparison as most patients have already unsuccessfully been down this path and thus will not experience a strong placebo effect (hence acupuncture appears more effective as it is a powerful placebo with all the mystique and theatrics).
As for your third point – absolutely!
The interesting thing is now many trials have “sham” arms involving non-invasive needles, needles in “unimportant” places (by the rules of TCM) or shallow needles that don’t elicit sensation. When there is no difference between this and “real” acupuncture the authors make a conceptual sidestep and claim that the sham must also have represented real acupuncture. It’s a nifty trapdoor to escape dodgy results!
As for the WHO. I would love to think they could be a robust regulator but they have a chequered history in acupuncture and some odd ideas about evidence based medicine – check out le canard noir on this (genuinely appalling):
http://www.quackometer.net/blog/2008/11/world-health-organisation-traditional.html
Maybe it is a clever form of sabotage? The BMJ will enforce strict peer review, therefore stopping the acupuncturists ever actually publishing an article?
Thinking a bit more about this I assume that the “sham acupuncture” fits in the same category as expensive placebos being more “effective” than cheap ones and dfiferent coloured placebos being “better” for different ailments.
I does bring to mind the old vaccination joke: “don’t worry – it’s just a small prick with a needle”.
They’ve stopped claiming they can help people stop smoking?!
I was very dismayed the other day when the secretaries asked me – since I’m supposed to be ‘sciency’ – why they were supposed to magnetise the needles they had stuck in their ears to make them stop smoking.
Too bad I was at a loss for words. I shoulda said something about gnomes’ weapons being magnetic and thus the tobacco demons, who’re hunted by gnomes in the wild, are scared of everything magnetic.
Makes as much sence as qi and meridians.
Sili
An understandable mistake but I think you menat goblins not gnomes
You could try telling them that:
“”””Your body needs iron so it can make haemogoblin, a substance in red blood cells that carries oxygen from the lungs to body tissues. Brain activity, breathing, cellular respiration and every activity of the body depends on there being enough iron in the blood to make haemogoblin””””””””
“”””The body contains between 3.5 and 4.5g of iron, 2/3 of which is present in haemogoblin””””
Magnetising the acupuncture needle aligns the flow of blood and forces the haemogoblins to head for magnetic north (which is obviously upwards) thus enhancing brain activity and facilitating respiration and the release of elfdorphins.
Tell them you saw it on the internet so it must be true.
David
I have to disagree with your objections to BMJ publications taking on “Acupuncture in Medicine”. I think that this move should be welcomed, but the welcome should be accompanied by two warnings.
The move should be welcomed because this presents us with an opportunity to ensure that studies on acupuncture are fair and scientific.
The journal’s advice to authors says that “Authors of controlled trials are advised to consult the CONSORT statement. Lancet 2001;357(9263):1191-4”.
They haven’t noticed (or do not want authors to notice) that the CONSORT website states: “Considered an evolving document, the CONSORT Statement is subject to periodic changes as new evidence emerges. This website contains the current definitive version of the CONSORT Statement and up-to-date information on extensions”.
We should therefore suggest:
(i) Acupuncture in Medicine should require authors of clinical trials to follow the CONSORT guidelines as published on the CONSORT website.
(ii) An extension to the CONSORT guidelines should be developed for acupuncture studies. The extension should require careful, transparent documentation of:
a. the type of acupuncture (“classical”, Western, electro, pressure), and
b. the type of control (sham acupuncture, other theatrical placebo, untheatrical placebo, “usual/standard” care, no care/watchful waiting).
c. How patients and assessors were blinded, and how blinding was maintained and verified
We should point out two dangers:
(i) Because it is impossible to prove that a treatment does not work, negative findings are likely to be used as a motivation for further research. We need agreed criteria (or, at least a debate on what criteria would be suitable) for deciding when further research is not justified. It would be useful to have guidelines on how to work out the costs vs likely benefits of further research, and how to direct (most) research resources to the most promising questions.
(ii) Reporting standards such as the CONSORT statements are intended to improve the quality of research. However, human nature being what it is, standards are likely to often be seen as box-ticking chores. And, sometimes they will be used creatively, to give the appearance of rigour, while disguising bias or fraud.
Footnotes
(i) My introduction to standards being used creatively to disguise bias was the “systematic” review: Efficacy of spinal manipulation and mobilization for low back pain and neck pain: a systematic review and best evidence synthesis: Bronfort G, Haas M, Evans RL, Bouter LM.
My most recent (and most dispiriting)discovery of creative box ticking is the British Homeopathic Association and Faculty of Homeopathy’s CPD forms http://www.trusthomeopathy.org/faculty/fac_cpd.html.
(ii) Wallace Sampson in 2005 pointed out that “Since 1999, the NIH [National Institutes of Health] has spent almost $1.5 billion in grants for research into alternative methods. NCCAM [National Center for Complementary and Alternative Medicine] has spent almost half that amount and has found no evidence of efficacy and little evidence of inefficacy.” Sampson W. Studying herbal remedies. N Engl J Med. 2005 Jul 28;353(4):337-9.
(iii) What the BMJ ought to have in their stable is a “Journal of placebo studies”. We need to know much more accurately what makes one placebo more effective than another.
Of course, if the BMJ Group were to really impose higher standards, I’d agree. But I doubt whether they will. That depends on editors (unchanged) and referees (largely, no doubt, acupuncture enthusiasts) than it depends on the publisher.
Wallace Sampson also had an excellent piece on Quackwatch, Why NCCAM should be defunded. See also Kimball Attwood: The Ongoing Problem with the National Center for Complementary and Alternative Medicine.
The situation in the USA is even worse than here in some ways, for the simple reason that they have more money to bribe universities.
Here is an updated version of spending on NCCAM
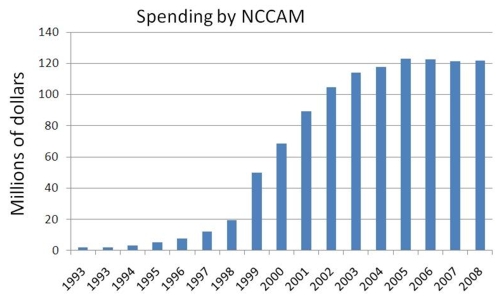
The problem is the journal will merely generate more research into acupuncture, most likely performed by acupuncture supporters. In a recent edition of Acupuncture in Medicine there is a narrative review of the issue of dosage in trials. We apparently do not know what the ideal dosage is and thus the trials may have used “inadequate” acupuncture. In the article there are some telling points raised, not least that acupuncturists can’t decide on a suitable dosage for trials! This seems pretty damning for current practice.
The only reason acupuncture is researched extensively is because it exists, it is widely used, acupuncture groups are effective advocates for their art and acupuncturists and patients “know” that it works.
The dosage argument is just rescue bias. And I suspect that’s what we might expect more of from this journal…
Ref:
White, A., Cummings, M. , Barlas, P., Cardini, F , Filshie, J , Foster, N.E. , Lundeberg, T. , Stener-Victorin, E. , Witt, C.
Defining an adequate dose of acupuncture using a neurophysiological approach – A narrative review of the literature
Acupunct Med. 2008 Jun;26(2):111-20
Researching highly implausible treatments just generates noise. The combination of inevitable false positives, publication bias and even fraud will ensure that there are enough ‘positive’ results to keep supporters happy and sceptics forever explaining why we have to be cautious. Homeopathy is the perfect example of this. The corpus of scientific literature in homeopathy is what we get when a popular placebo therapy is researched. It has its positive results, its small and underpowered studies, its large and methodologically flawed studies and several large good studies that show no result. Researching acupuncture will undoubtedly produce a similar looking body of results, satisfying no-one.
I agree with you Andy (I cannot keep calling you LCN, the Black Duck etc).
I read this today . . . . . ..
Click to access ruta6.pdf
. . . . .which seems to be a stunning success and a total vindication for homeowhatsit (although it might just as well have been acuthingy or faith healing).
You can probably dissect this more effectively than me but my take on it is:
– very sample sample size (15)
– no control group
– no idea of patients being on any other medication before or during the trial (assuming they were)
– no rationale for the choice of ruta as a remedy – why not antimatter ? (Apart from the fact that the Romans used it !)
– confusion between a herb (which might well kill cells) and a 30C dilution of said herb (which almost certainly will not)
– (and much as I am loathe to say it) it is from India where all positive HY trials seem to originate from – for whatever reason.
My take is that this is a few case notes showing a strong placebo effect with some bias built into the whole thing.
As ever I am happy to be proved wrong.
I’ve just checked out the link to the acupuncture fertility trial on the miniblog. You really have to admire the doublethink on display in the report.
They find : “Placebo acupuncture was associated with a significantly higher overall pregnancy rate
when compared with real acupuncture.”
They conclude: “Placebo acupuncture may not be inert”.
Were it not so dishonest it would be comedy gold.
The sad thing about this is that some people will be so desperate to have a child they will clutch at straws like this.
My sister in law was in exactly this position. Two failed IVF treatments and only one chance at treatment left.
She was contemplating all the woo she discovered on the net. I gently suggested that she should try her last IVF chance and explore the mumbo-jumbo afterwards (you have to be a bit considerate in situations like this. Don’t be a w****r is not really appropriate).
Luckily this worked and her baby is due in January – which is good news and a sort of victory for proper medicine.
NeoConnel – The finding and conclusion you refer to above would make the Ministry of Truth blush. I read this as “the bogus thing is apparently better than the real thing therefore the bogus thing may be more real than the real thing which has less effectivenes than the bogus thing which is not as useless as the real thing”. Or is that Coke I am thinking about.
That seems the fair interpretation!
As the case of your sister-in-law demonstrates, people are most susceptible to nonsense when they are at their most vulnerable and it is no surpise that woo-sters specifically target vulnerable populations. A bit like cults really!
Interesting that the BMJ Group is now advertising for a Clinical Director of the BMJ Evidence Centre. Their blurb states that, inter alia,
“You will articulate our vision and mission to key stakeholders and opinion leaders, and confirm our position as a leading organisation in the field of evidence-based medicine.”
Well I suppose there’s a lot to be said for a journal of negative results, which is what `Acupuncture in Medicine’ is likely to be.
[…] other week I wearily noted the announcement that the BMJ Group has taken over the journal of the British Medical Acupuncture Society. The Group seems inordinately proud of its first foray into complementary medicine – no doubt […]
The NICE guidelines for managing low back pain are due out in May 2009. The draft is available and the document is undergoing consultation.
They are set to recommend acupuncture as: “Evidence suggests that seeing an acupuncturist was better than usual care but not much difference between acupuncture and sham. However, sham acupuncture is used as an active form of treatment by some practitioners, therefore this should be considered as a possible treatment.”
A conscious decision to offer people a pretend therapy?
It is surprising how many people don’t actually read the evidence – even when it’s on your own blog. The Cochrane review of acupuncture is cited above: ‘acupuncture is more effective for pain relief and functional improvement than no treatment or sham treatment immediately after treatment’
What is it about ‘more effective’ and ‘sham’ that is so difficult to understand? Or perhaps, more accurately, difficult to accept?
Fortunately the BMJ are open to the possibility that acupuncture may have biological effects, as we are in Acupuncture in Medicine.
Needleman
What I wrote in the blog makes it clear that there remain a few areas of uncertainty. Singh & Ernst make that quite clear.
Like just about all alternative medicine advocates, you are being rather selective. The review that your quote was for low back pain only, and its conclusion, which you don’t quite was
“The data do not allow firm conclusions about the effectiveness of acupuncture for acute low-back pain.”
For most of the other conditions which acupuncturists claim regularly to be able to benefit, the evidence is quite clear that sham and ‘real’ don’t differ perceptibly. I think you should read Barker Bausell’s book. It is really very thorough.
The upsurge of interest in all sorts of alternative medicine in the last 30 years has had one benefit. In some areas (especially homeopathy and acupuncture) some really good trials have been done. The outcome is that, for homeopathy, the game is up. And for acupuncture, you are left grasping at a few straws.
Ah, but the key there is the “immediately after treatment” bit. Lasting benefits are left wanting. If you feel more of a prick(!) at the time perhaps you may feel more convinced to feel better. And we had better not ignore the line ” most of the studies were of lower methodological quality”
Consider the review by Derry et al. (2006) that concluded that when that when controlling for methodological and interpretive limitations, no robust evidence could be found that acupuncture is effective for any indication.
Or indeed the most recent SR of acupuncture for low back pain mentioned above (Yuan et al. 2008) that included the most recent, biggest and best designed trials (well designed but poorly interpreted – can’t have it all) that finds “strong evidence of no significant difference between acupuncture and sham acupuncture”. I wonder what it is about “no more effective than sham” that is so difficult to accept.
The interesting thing with that review is that there was only moderate evidence (only 1 quality trial or a few poor quality trials) that acupuncture was more effective than no treatment.
The bulk of the evidence suggests that for any clinically meaningful outcome acupuncture is no more effective than sham, but both (like most things) are better than doing nowt. That might explain the reluctance of some of us to but into it. That and the implausible nature of the therapy.
Ref:
Derry, C.J., Derry, S., McQuay, H.J., & Moore, R.A. (2006). Systematic review of systematic reviews of acupuncture published 1996-2005. Clinical Medicine, Journal of the Royal College of Physicians of London, 6(4), 381-386.
Yuan et al. See prior post.
I realised my previous comment was missing some “boguses”.
It should have read “the bogus bogus thing is apparently less bogus than the bogus real thing therefore the bogus bogus thing may be less bogus than the bogus real thing which has more bogusness than the bogus bogus thing which is less bogus than the bogus real thing”.
Apologies for the omission.
I got conned by needleman and his ilk. Under sufferance I went to a needlist (mid-80s) to stop me smoking. Seemed about as valid as any other way. Didn’t work. Wanted a fag as soon as I came out of the needle parlour (on extremely spurious advice I had binned my fags and lighter).
I waited until I had saved the cost of the needling and stared smoking again. I found the long term threat of lung cancer preferable to poking a piece of wood in my ear.
Useless nonsense.
I quoted acupuncture for back pain, but I could as easily have quoted the one on knee pain from the blog, from the highly respected Bandolier, ‘One in osteoarthritis of the knee, had statistical improvement over sham acupuncture at three months’.
The fact remains that acupuncture is used much more for musculoskeletal conditions than for everything else, and it is for these conditions that the negative results are counterbalanced by positive ones.
I am just as much against unjustifiable claims for acupuncture as you are. However, I am not convinced that the present state of evidence allows a sensible judgement on what is justifiable. For both back pain and knee pain, systematic reviews have gone from equivocal to positive over recent years with the addition of higher qualty evidence. What other treatment can claim that? One would have expected the opposite.
neoconnell, we use sham controlled studies to investigate whether or not acupunctrue has a biological effect. The duration of effect is not relevant to this question: we decide on clinical effectiveness from comparisons with standardised treatment.
This is exactly the argument set out in the CONSORT extension for pragmatic trials, in this week’s BMJ (no less!) BMJ 2008;337:a2390 .
That is precisely the opposite of the conclusion drawn by Bausell. How do you account for that? If you think that the conclusion of Singh & Ernst is wrong, please say why.
Both Bausell and Ernst have been involved directly in acupuncture research. The big difference is that they don’t make their living from it. They have no vested interest in coming to a particular conclusion.
I guess this discussion does emphasise a real problem. It is really quite hard to expect anyone who has invested much of their life to a particular therapy, and makes their living from it, to say “oops I’ve been wrong all along”. The same applies to universities who run degrees in these things. Perhaps we should be thinking about ways to allow people to withdraw gently from ideas that prove to be wrong, without excessive embarrassment.
It’s not for me to explain ‘why’ people write what they do. These are the references for the back pain reviews from 1998 and 2005, and the relevant parts of the abstracts (I have cut some phrases but you can check the original and I think you will agree I have not altered the essence)
Ernst E, White AR. Acupuncture for back pain: a meta-analysis of randomized controlled trials. Arch Intern Med 1998;158:2235-41.
RESULTS: Twelve studies were included, of which 9 presented data suitable for meta-analysis. The odds ratio of improvement with acupuncture compared with control intervention was 2.30 (95% confidence interval, 1.28-4.13). For sham-controlled, evaluator-blinded studies, the odds ratio was 1.37 (95% confidence interval, 0.84-2.25). CONCLUSION: Acupuncture was shown to be superior to various control interventions, although there is insufficient evidence to state whether it is superior to placebo.
Manheimer E, White A, Berman B, Forys K, Ernst E. Meta-analysis: acupuncture for low back pain. Ann Intern Med 2005;142(8):651-63.
The 33 randomized, controlled trials that met inclusion criteria … For the primary outcome of short-term relief of chronic pain, the meta-analyses showed that acupuncture is significantly more effective than sham treatment (standardized mean difference, 0.54 [95% CI, 0.35 to 0.73]; 7 trials) and no additional treatment (standardized mean difference, 0.69 [CI, 0.40 to 0.98]; 8 trials). … Data are also insufficient for drawing conclusions about acupuncture’s short-term effectiveness compared with most other therapies. LIMITATIONS: The quantity and quality of the included trials varied. CONCLUSIONS: Acupuncture effectively relieves chronic low back pain. No evidence suggests that acupuncture is more effective than other active therapies.
Thus acupuncture doesn’t seem to fit your phrase of ‘ideas that prove to be wrong’, at least according to the evidence.
There you go again, being selective. But even taking the references you have chosen. the first concludes
and the second concludes
If you accept those conclusions them why bother with all that needle palaver? You may or may not yourself believe in all the ancient vitalistic gobbledygook about meridians an “Qi”yourself, but if you allow acupuncture on the NHS the HR department will ensure that students are told that it is true. That is the
training dilemma of alternative medicine
.
The discussion was about acupuncture versus sham acupuncture, addressing your question whether acupuncture has a biological effect or not. That’s where the evidence has shifted between 1998 and 2005.
I am not questioning the fact that there is insufficient evidence to decide whether acupuncture should be reimbursed by the NHS (although you may be interested to know that the German system, recognised for being evidence based, does reimburse acupuncture for back pain).
My conclusions are dismissed as due to financial bias, but the extent of this is always explicit.
Your statement about training is not correct; for some years now, doctors have been taught acupuncture without recourse to vitalistic gobbledygook and qi. Neurophysiology provides a highly acceptable and rational basis for a modern health practitioner ot understand acupuncture.
Well perhaps, but the vast majority of acupuncturists are not doctors, and what you very properly describe as vitalistic gobbledygook is by far the predominant approach.
I dispute strongly that “Neurophysiology provides a highly acceptable and rational basis. . . “. Of course it has been known for a long time that if you stick a needle in yourself it produces a signal in the brain. That is standard sensory physiology. But that casts no light at all on whether or not patients get any benefit from the procedure that is large enough or sufficiently long-lasting, to be worthwhile. There is nothing in neurophysiology that makes such an outcome likely. It still boils down to good trials. And in most good trials it is indistinguishable from sham
May I ask if you have read Bausell’s book? I think you should.
The ‘vast majority of acupuncturists’ are gradually coming round to a neurophysiological approach, actually. It wil of course take time.
And that is precisely why Acupuncture in Medicine – representing a rational, objective approach to acupuncture – should be part of the mainstream science – hence the link with the BMJ!
Well that is odd. The British Acupuncture Council says
Not much sign of a trend away from vitalism there.
I guess “Needleman” must be from the medical acupuncture school whose thinking (“Keep the needles but dump the woo-woo philosophy”) is briefly summarised by medical acupuncturist Dr Anthony Campbell here.
As regards the journal, the key question for me is: how sceptical are the editors and reviewers going to be? Unlike DC I am fairly agnostic about medical acupuncture (which may simply be because I haven’t actually read the studies or meta-analyses on acupuncture). But – experience with the CAM journals repeatedly show that if the new journal becomes a back-slapping club for medical acupuncturists (and thus almost by definition ends up with a whopping positive publication bias) then it will simply end up being a PR sheet rather than a serious journal.
Put another way, the journal will have to use as many non-acupuncturist statistical experts and sceptics (i.e. people like Bausell, Edzard Ernst and DC) as referees and editors as they do acupuncturists if they want to be viewed as the real deal. At least by me.
As I have understood it from the blogosphere, the beneficial effect (over sham intervention) of acupuncture gets less the more convincing the sham intervention is. And even the retractable needles have been argued by some not to be a truly convincing sham intervention. So if there is a tiny or no effect vs. sham intervention with an imperfect sham intervention…. hmmm.
I shall look forward to seeing this issue examined in the new journal’s pages.
PS Oops – first hotlink didn’t work. Correct link is here.
I can’t quite agree with Campbell that acupuncture isn’t CAM. The procedure is, after all, pretty bizarre. Impaling someone with needles sounds a bit like voodoo, Until such time as there is a clear demonstration that there is a real, substantial advantage over other treatments, I think it should be regarded as firmly ‘alternative’.
Needleman himself says
On that, at least, we can agree.
Good news and bad news.
On the Schadenfreude front, I’ve been happy to see both secretaries shivering in the cold, still smoking.
Unfortunately I’ve now learnt that one of the librarians get needled by his GP for back pain (ruined his back working as a gardener). It doesn’t sound like it’s working, obviously: “Well, I think I feel a bit better afterwards.” What’s even more galling is that he works out lightly at a fitness centre too, and from the way he describes it, that sounds to be a lot more effective.
I’m really saddened to learn that we have GP-needlers here in Denmark. I need to start venting in Danish, I think. I seem to recall seeing a headline about the major health insurer considering paying for … what do you call in English? that thing where they rub one’s feet can claim that it’ll help one’s kidneys, lungs and whatnot?
[…] BMAS – a confession 1 December, 2008 Posted by northerndoctor in Uncategorized. trackback OK, I think I had better confess before I go any further. I am GP and I have been on a British Medical Acupuncture Society (BMAS) course. I have been thinking of posting this for a wee while but I feel my hand has been forced as the BMAS has been dragged into the limelight by the good Dr David Colquhoun. […]
I’ve come in late on this thread so apologies but I do have a few points…
One of the major criticisms of acupuncture practice is the lack of an evidence base showing efficacy despite good therapeutic results.
From the point of view of producing more and better quality trials of acupuncture it is a good thing that the BMJ has taken on the BMAS publication. The standard of trials conducted will hopefully increase as a result of the bar being raised by the BMJ.
On the question of sham acupuncture – sham interventions are NOT placebo controls. They are designed to investigate a particular or suspected mechanism of action of acupuncture, not evaluate effectiveness.
They are not inert as they produce measurable physiological effects specific to the tested therapy that bias the trial. (see ref at end)
Trials that show little difference between verum and sham arms are not showing little difference between verum and placebo. In effect they are showing the difference between a constricted version of acupuncture (due to the strict controls applied to the tested therapy which are necessary in order to administer a ‘repeatable dosage’) and another, sub-optimal version of acupuncture (sham needling).
The effectiveness of Traditional Chinese acupuncture (or even Medical acupuncture) is not being investigated in these trials.
Sham controls should be used for example when investigating what depth needles should be inserted, or for how long, or for determining the appropriateness of a particular protocol…
Conclusions that acupuncture is no more effective than placebo on the basis of sham controlled trials are incorrect. It is both an innappropriate judgement by commentators as well as being poor methodology by researchers.
When evaluating the effectiveness of acupuncture then there is no need for a placebo arm. There is obviously a need for a control arm and that can take the form of a standard treatment group (eg – physiotherapy or drug treatment for osteoarthritis of the knee compared to acupuncture therapy). If the overall effectiveness of acupuncture comes out well in this sort of trial then further research can be conducted into what exactly is going on and sham controls can be introduced to help elucidate specific mechanisms and component efficacy.
There are many hurdles in running RCTs evaluating acupuncture, just as there are many problems in evaluating other complex therapies using this model (physiotherapy is one example).
Just because it seems implausible doesn’t mean that it doesn’t work or at least that there isn’t something in it. Hopefully as time goes on the design and interpretation of trials will continue to get better (e.g. – sham will stop being confused as placebo) and that is a good thing for an unbiased appraisal of the therapy.
Some further reading on sham, placebo and the problems of acupuncture trial design and methodology can be found in the following book:
MacPherson, H (2008).
Acupuncture research; Strategies for establishing an evidence base. Edinburgh;
Churchill Livingstone.
This is an excellent book which thoroughly reviews the state of play of acupuncture research, and in my opinion is a much fairer take than that taken by the recent best sellers by Ernst et al…worth reading for a balanced view.
CZ
I see no sign of the BMJ “raising the bar”. The journal is being run by exactly the same people as it was before.
Isn’t that a rather weighted way to put it? The therapeutic results can be described as “good” if there is some specific effect of the needles.
The thing that is quite well established is that acupuncture, in most good trials. is no different from sham acupuncture. That immediately makes nonsense of the alleged principles of acupuncture. I know that the people who run Acupuncture in Medicine disavow all the nonsense about meridians, but the vast majority of acupuncturists do not. If you want a job the HR department will insist you have been examined in “Qi”.
It is true that sham acupuncture has often turned out to be better than non-blind standard treatment. But remember we are talking mostly about conditions where the standard treatment is not very effective.
The simplest interpretation of that still seems to me to be that the needles are a particularly theatrical placebo, Placebos can,of course, produce real physical effects, but they raise all sorts of ethical dilemmas about lying to patients and about therapists lying to themselves. The fact is that even the medical acupuncturists have failed to address that possibility seriously is a cause of concern. The problem, as always, is that if they were to do so they would be out of work.
I agree it is just possible that in a few cases there could be something specific going on, but it is very far from being demonstrated. The fact that you can get the effect with retracting needles that barely penetrate makes a total nonsense of the subject as usually presented
I still think that the most likely interpretation is this. Acupuncture is a rather bizarre form of pre-scientific treatment that would have died out long ago if it had not been revived by Mao Tse-Tung for nationalistic reasons, rather medical reasons, and then bolstered by the post-Reagan fashion for believing bizarre myths,
It would be more interesting, and more profitable, to spend time on honest investigations of placebo effects, and trying to sort out how much of the apparent effects of alternative treatments is a result of real placebo effects and how much of it is just regression to the mean. They are really interesting questions.
Yes, i think research into placebo effects is very interesting…Ted Kaptchuk at Harvard does a lot of research into placebo, healing rituals and acupuncture but what I find especially interesting is the possibility that placebo effects represent a host of “self-healing mechanisms” that are almost completely misunderstood by science.
The fact that people recover and apparently heal better or quicker under the influence of placebo agents is frankly remarkable and is testament to the importance and influence the mind has in ill health.
It’s even more interesting when one gets into expectancy effects and placebo analgesia as some of the work done by Benedetti in this area puts a lot of the accepted theory of biochemical analgesia into the nonsense bracket.
I believe that one of the ways acupuncturists help patients is by encouraging their own self-healing processes. If placebo effects do represent self-healing mechanisms then getting a strong ‘placebo’ response is exactly what is desired, (yes i’m aware of the ethical dilemmas…)
you say, “The thing that is quite well established is that acupuncture, in most good trials, is no different from sham acupuncture. That immediately makes nonsense of the alleged principles of acupuncture.”
This is a good point, and not easily countered in a short blog. As i mentioned before, there are many problems in designing trials and as sham generates specific physiological effects, (yes, even the retractable needles…just check out the book i referenced last post) it may be that greater sample numbers are required to see the difference between the two forms of needling?
Does this mean acupuncture is just a theatrical placebo? No, I don’t believe it does. It definitely means that a part of the efficacy of acupuncture is a result of a strong mobilisation of the body’s self-healing mechanisms (a maximising of all the non-specific or placebo effects) but it also most definitely DOES NOT produce results solely as a result of so called placebo effects as there are clearly demonstrable if still largely misunderstood specific physiological and energetic effects of needling. – all the more reason for more quality research.
Incidently, Mao (in one of his characteristically psychopathic ‘reforms’) tried to wipe out traditional forms of medicine in favour of modern medicine first…until he realised that traditional medicine actually was producing good results and cheaply. He then declared it a ‘treasure house’, unified the different theories into TCM, threw out the more esoteric parts and set up TCM schools and universities…also, don’t believe all that is written in ernst et als books about the history of TCM – it still is practiced in East Asia, and it thrives alongside conventional medicine in modern hospitals…but admittedly the Chinese don’t view it with as much emotional attachment as some people do in the west…they just use what works.
Whilst I appreciate that there are different forms of acupuncture and that perhaps some do not involve quite this sort of woo, there are some alarming statements in the world of acupuncture. The quotes below may belong also on pages concerned with ‘traditional ‘ Chinese medicine being taught in universities. The quotes are from the site ‘Acuxo -Acupuncture Research and Resource’. No comment other than a few interjections in square brackets. I started with this page:
http://www.acuxo.com/meridianPictures.asp?point=GV16&meridian=Governing+Vessel
GV16 • Feng Fu • Governing Vessel 16 Wind Mansion. Meeting Point on the Governing Vessel with the Yang Linking Vessel. Sea of Marrow Point. [The indications for this point are] Expels Wind; Strengthens The Sea Of Marrow [have searched the atlas but can’t find this]
TB1 • Guan Chong • Triple Burner 1 Passage Hub. Jing Well Point on the Triple Energizer Channel. Metal Point on Fire Meridian.
Location: On the ulnar side of the fourth digit, 0.1 cun from the corner of the nailbed.
Clears Upper Burner Heat [sounds more like a job for the polumber]
Benefits The Ears And Tongue
Activates The Channel [?]
BL1 • Jing Ming Bladder 1 Bright Eyes. Meeting Point on Bladder Channel with Small Intestine……….
Location: On the face, 0.1 cun superior to the inner canthus when the eye is closed [sticking a needle into your face somewhere near the eye is supposed to benefit the bladder?]
and so it goes on. From this site is a link to:
http://acugraph.com/?gclid=CJTOysHAs5cCFYwh3god3gvwjg
where the director of a firm does a hard sell for a gadget for acupuncturists. This purports to show the patients how the body’s energies work and how acupuncture can help them. The graphics look a bit like a clip from a sci-fi film.
Thanks Lindy -amazing salesmanship, not so impressive assessment.
On a similar topic, a recent review of The Recent History of Acupuncture, by Ernst in American Journal of Medicine is interesting.
Lindy,
ok, the link to the guy selling some piece of software (or whatever) is a little wacky, does not represent traditional or medical acupuncture but does represent vulgar salesmanship…which is apparent in any walk of life…
it’s interesting that I have approached this forum with the aim of discussing the subject in western scientific terms. I understand that evidence based medicine is the language that means the most to this audience and am comfortable using it.
You however have decided to use the language of traditional chinese medicine which is a completely philosophical and poetic way to view the natural world and the human body…and you have gone to a random website and copied and pasted extracts that sound suitably random and wacky.
The language of TCM does not make any sense from a scientific perspective. Everyone knows that. it’s a boring argument.
what it does, is give you another way to philosophically view health and illness, and that’s all! In case you are interested it is based in daoism and confucianism…but i suppose you are not that interested.
David,
thanks for the link to ernst’s article – i hadn’t seen this one before…he appears to again be saying (despite much contrary evidence) that there is no specific effect to acupuncture, that it is all placebo – i’ve already posted on this so won’t repeat myself.
What is important that he ends the article by saying that “acupuncture has been submitted to rigorous science—and conclusively failed the test.”
This is not true. What is true is that acupuncture has been submitted to rigorous bad science.
Trials have used active sham interventions as placebo arms (yes, the retractable needle does create a physiological effect – just because it is validated doesn’t mean it is inert, it just means naive patients couldn’t tell the difference!!), most trials have small sample sizes and all trials use restricted versions of the verum arms.
It’s true that most trials show little difference btw verum arms and sham arms (NOT placebo!!), but this result shows that more research is needed into the efficacy of specific components of needling in order to refine good practice.
It DOES NOT show that acupuncture is mere placebo, or that it is not effective.
No, but it does show that meridians and Qi are bullshit. That is all that I (or Ernst) have claimed.
It remains possible that pricking anywhere produces some amazing therapeutic effect in a few conditions. We obviously expect some ;expectation’ or placebo effect in the non-blind comparison between regular treatment and sham (or real) acupuncture. But is it really very likely?
“acupuncture has been submitted to rigorous bad science.”
Have you read Bausell’s book? He is a statistician and experimental designer. He describes some really good experiments that have been done in the last few years. Unlike, for example, TCM, acupuncture has been quite well tested, and the tests have been failed in the sense that there is still no good reason to believe that it is more than a rather theatrical and effective placebo.
[…] Eight random needles […]
Sorry to wake a dying thread but thought this might illustrate our point. 2 crackingly revealing abstracts from Acupuncture in Medicine.
In the first installment we see how by providing a rather ambitiously complex account of what sounds like placebo neuropsychology the authors attempt to construct a specific mechanism for acupuncture (genuinely cheeky but ambitious and creative:
http://www.ncbi.nlm.nih.gov/pubmed/17906602?ordinalpos=12&itool=EntrezSystem2.PEntrez.Pubmed.Pubmed_ResultsPanel.Pubmed_DefaultReportPanel.Pubmed_RVDocSum
In the second we see again that there can be no sham, and thus acupuncture must work:
http://www.ncbi.nlm.nih.gov/pubmed/19098696?ordinalpos=1&itool=EntrezSystem2.PEntrez.Pubmed.Pubmed_ResultsPanel.Pubmed_DefaultReportPanel.Pubmed_RVDocSum
If these are representative examples of the journal’s output then it seems unlikely that it will lead to a fair and balanced appraisal of acupuncture.
There’s a nice one about acupuncture for tortoises but I can’t access the full text.
Ha!
“The transposition of acupuncture points from canine charts is a viable alternative for chelonians.”
Phew, now I know what to do the next time my terrapin develops a limp.
Seriously – case studies on tortoises. I predict big impact factors.
Although looking at the publication date it just might be a yuletide spoof!
I doubt if it is a spoof. These people really believe this stuff.
There are loads of article cross-referenced from the link above involving tortoises – the poor animal seem to be much prodded, poked and molested in the name of woo.
I did stop counting them (11) when I got to the one on “””Fecal incontinence treated with acupuncture””” (although that was a study involving 15 women so the poor bloody tortoises got a rest for once).
Amazingly it concluded that “”””Acupuncture offers good opportunities for improving fecal incontinence. The mechanism of action is obscure but might be an effect of the “neuromodulation” of the recto-anal function similar to that explaining the favorable results achieved by sacral nerve stimulation””””. Pile the woo on.
Maybe the women (like the much put upon tortoise) just got better.
I couldn’t bring myself to read the article on acupuncture by Dr Wu.
(Although I eventually gave in to the dark side of the force and read it. I just could not resist the combination of name and topic.)
To give credit where it is due the conclusions were that acupuncture was rubbish and no better than sham needling or doing nothing. And the rest of his research appears to fit the category I would define as “sane”. So well done Doctor Wu.
http://www.ncbi.nlm.nih.gov/pubmed/12614526?ordinalpos=21&itool=EntrezSystem2.PEntrez.Pubmed.Pubmed_ResultsPanel.Pubmed_DefaultReportPanel.Pubmed_RVDocSum
(Still makes me laugh though).
[…] Almost all of the reviews fail to come up with any positive evidence that acupuncture works well enough to be clinically useful. Only two come close, and they are the two singled out as “editor’s picks”. Perhaps that’s not entirely surprising given that the editor is Dr Mike Cummings. […]
[…] is a small group of ‘medical acupuncturists‘ that believes that it is hokum. but who nonetheless maintain that acupuncture works, despite […]
[…] BMJ Group promotes acupuncture: pure greed @bengoldacre BMJ Group's Acupuncture in Medicine one of the highest profile offenders "building the evidence base" http://t.co/7l5kj3mS… Source: http://www.dcscience.net […]
[…] a lobby group representing its members. In a he-said-she-said scenario we have to look for what the evidence supports. It’s the fields that practice some evidence-based health, including: dentists, physios, […]